Doxorubicin is a type of chemotherapy drug called an anthracycline. It slows or stops the growth of cancer cells by blocking an enzyme called topoisomerase 2. Cancer cells need this enzyme to divide and grow.
Doxorubicin can be given in combination with other chemotherapy drugs.
Indications
- Diffuse large B-cell lymphoma (DLBCL)
- Burkitt lymphoma (BL)
- Hodgkin lymphoma (HL)
- Mantle cell lymphoma (MCL)
- Non-Hodgkin lymphoma (NHL)
Baseline tests
Prior to administration, the doctor will order a heart scan before to ensure that the patient’s heart is functioning well. Heart scans will be given during and after treatment to ensure that doxorubicin is not harming the heart. See precautions below for more information.
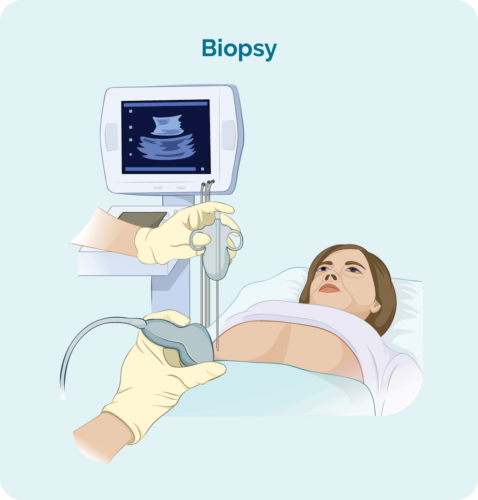
Administration
The amount of doxorubicin depends on many factors including:
- Height and weight
- General health or other health problems
- Type of lymphoma being treated
Doxorubicin is given in the chemotherapy day unit or during a stay in hospital.
The nurse will give the patient anti-sickness drugs before starting and patients have the doxorubicin (a red fluid) infused via a cannula or central line.
Doxorubicin is given via a gravity infusion rather than pushed through the IV pump. This is because doxorubicin is called a ‘vesicant’ where if the drug leaks out of the vein and into the surrounding tissue, it can cause tissue damage.
The nurse will stay with the patient to ensure the drug has no issues being administered and they will stop the infusion if there is any pain or if there is an interruption of flow.
Doxorubicin is then given in one of the following ways:
- Through a short, thin tube (cannula) the nurse puts this into a vein in the arm or hand
- Through a fine tube that goes under the skin of the chest and into a vein close by (central line)
- Through a fine tube that is put into a vein in the arm and goes up into a vein in the chest (PICC line).
Sometimes, it is given over a few days through a small pump, which is connected to your line and the pump can be carried on a belt or in a bag.
Possible side-effects
- Increased risk of getting an infection
- Anaemia (decreased red blood cells)
- Thrombocytopenia (decreased platelets)
- Tiredness and weakness (fatigue)
- Hair loss
- Sore mouth
- Loss of appetite
- Diarrhoea or constipation
- Fever (High temperature)
- Nausea and vomiting
- Doxorubicin may colour the urine red for 1-2 days after treatment. This is no cause for alarm
- Redness, soreness and peeling on hands and soles of feet. This is called hand-foot syndrome or palmar plantar syndrome.
- Heart changes
- Liver changes
Precautions
- Doxorubicin can cause cardiotoxicity that may cause a reduction in heart function. This can occur from the first dose of doxorubicin (acute), and can occur over the course of treatment or late (after treatment) effects.
- A scan to test the left ventricular ejection fraction (LVEF) is given to see how well the heart is pumping blood out of the heart.
- Before receiving the drug, the doctor will order a heart scan to determine the heart’s baseline function. This is to identify any underlying heart issues before the start of treatment. The heart scan will be repeated during and after treatment to ensure that doxorubicin is not causing any harm.
- If there is a change to the heart function, the doctor will either reduce the doxorubicin dose or will stop the drug all together.
The total lifetime amount of doxorubicin is 450mg/m2 .
The doctor will keep a record of how much has been given to a patient eg. 6 cycle of CHOPO = 300mg/m2