Finding out you have lymphoma is scary and comes with all sorts of life changing decisions.
But, finding out you have lymphoma while you are pregnant, means there are so many more things you need to consider. Not to mention having the joy and excitement of your pregnancy taken over with fear and worry for the future.
This page aims to give you the information you need to make good choices based on your own individual circumstance.
Firstly, many lymphomas respond very well to treatment. Your pregnancy will not make your lymphoma worse. The lymphoma is not fueled by your pregnancy hormones.
However, your doctors will need to consider the timing and type of treatment you receive.

Related pages
Can I keep my baby?
One of the first questions you may have is “Can I keep my baby?”.
In many cases the answer is YES.
Having lymphoma does make things more difficult, however many women have kept their baby when diagnosed with lymphoma during pregnancy, and given birth to healthy babies.
Your doctor will need to consider many things before giving you advice on this though, including:
- What subtype of lymphoma you have.
- The stage and grade of your lymphoma.
- The stage of your pregnancy – 1st, 2nd or 3rd trimester.
- How your body is coping with the lymphoma and pregnancy.
- Any other medical conditions you have, or medicines you take.
- Your overall wellbeing including your mental, emotional and physical health.
- Your own beliefs and choices.
How do I decide if I should have medical termination (abortion)?
A termination is a difficult decision at any time, but if your baby is wanted, or was planned, a decision to terminate the pregnancy due to lymphoma will be even more difficult. Ask what support is available to help you cope with the decision you make, or to help you talk through your options.
Most hospitals will have counselors or psychologists that can help. You can also ask your doctor to refer you to a family planning centre.
This very difficult decision is one only you can make. You may have a partner, parents or trusted family, friends or a spiritual advisor that you can talk to for guidance. Your doctors and nurses can also give you advice, but in the end the decision is yours.
Your healthcare team will not judge you whether you keep your baby, or make the difficult decision to terminate the pregnancy.
Will I be able to get pregnant again after treatment?
Many treatments for lymphoma can affect your fertility, making it difficult to get pregnant. These changes to your fertility may be temporary or permanent. However, there are some options to increase your chances of future pregnancies. We have included a link further down this page to more information on fertility services (See Who should be involved in my care).
How common is lymphoma during pregnancy?
Being diagnosed with lymphoma during pregnancy is rare. About 1 in every 6000 pregnancies can come with a lymphoma diagnosis, either during pregnancy, or in the first year after birth. This means up to 50 families in Australia may face a diagnosis of lymphoma during, or soon after pregnancy each year.
So what is lymphoma anyway?
Now that we’ve answered probably one of the most important questions you have, you are probably wondering what lymphoma is.
Lymphoma is a term used to describe about 80 different types of cancer. It happens when specialised white blood cells called lymphocytes undergo changes and become cancerous.
We have B-cell lymphocytes and T-cell lymphocytes. Your lymphoma will be either B-cell lymphoma or T-cell lymphoma. B-cell lymphomas are much more common in pregnancy.
Although lymphocytes are a type of blood cell, we have very few in our blood, so lymphoma is often not picked up in blood tests.
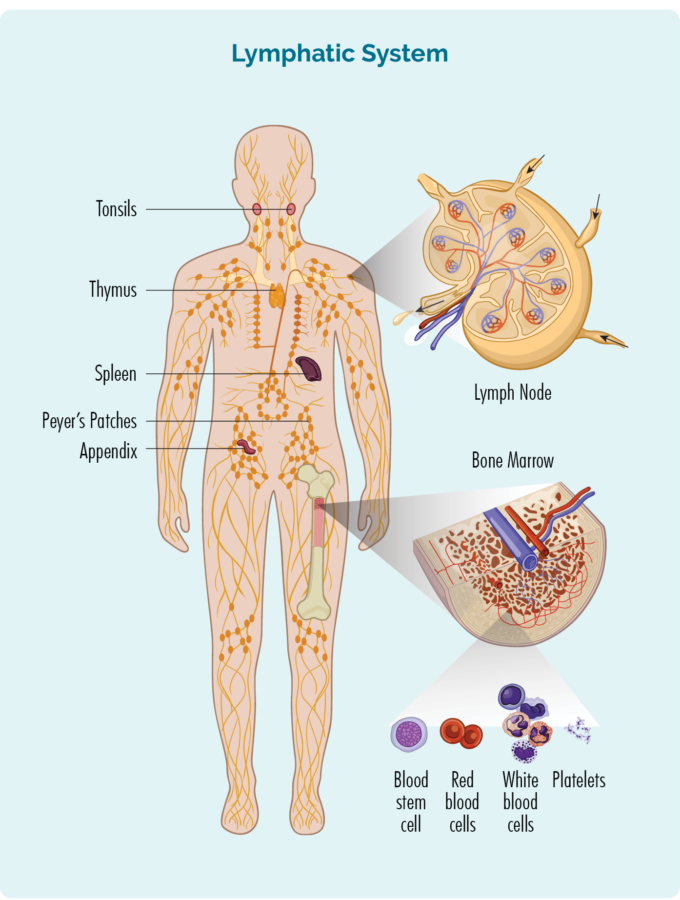
Instead, lymphocytes live in our lymphatic system, and can travel to any part of our bodies. They are an important part of our immune system, protecting us from illness and disease.
This page is dedicated to the special information around lymphoma when it is diagnosed during pregnancy. For a more detailed description of lymphoma, please click the link below.
What is the most common subtype of lymphoma during pregnancy?
As mentioned above, there are over 80 different subtypes of lymphoma. They come under 2 main groups:
Both Hodgkin and Non-Hodgkin Lymphoma can be diagnosed during pregnancy, though Hodgkin Lymphoma is more common. If you are diagnosed with Non-Hodgkin Lymphoma during your pregnancy, it is more likely to an aggressive subtype. Hodgkin Lymphoma is also usually an aggressive type of lymphoma. Aggressive B-cell lymphomas are more common in pregnancy.
Although aggressive lymphoma sounds scary, the good news is that many aggressive lymphomas respond very well to treatment and can be cured or put into long-term remission. Even if you have been diagnosed during pregnancy, you still have a good chance of being cured or going into a long-term remission.
Can I have treatment for lymphoma while I'm pregnant?
Decisions on treatment will vary between people. Some lymphomas do not need treatment straight away whether you are pregnant or not. Indolent lymphomas are slow-growing and often do not need to be treated straight away. About 1 in 5 people with indolent lymphoma will never need treatment.
However, as we mentioned above, if you are diagnosed with lymphoma while you are pregnant, there is good chance your lymphoma will be an aggressive subtype.
Most aggressive lymphomas will need to be treated with medicines called chemotherapy. You will likely have several different types of chemotherapy put together into your treatment protocol. In many cases, depending on the individual proteins found on your lymphoma cells, you may also have another medicine called a monoclonal antibody in your treatment protocol.
Other types of treatment that you may need for lymphoma, either with or without chemotherapy include surgery, radiotherapy, stem cell transplant or CAR T-cell therapy.
What treatment can I have during my pregnancy?
Surgery
Radiotherapy
Chemotherapy and monoclonal antibodies
These are the most common treatments for aggressive B-cell lymphomas, and can be given during some stages of pregnancy.
When is it safe to have treatment during my pregnancy?
Ideally, treatment would start after your baby is born. However, depending how many weeks pregnant you are when you are diagnosed, this may not be possible.
Surgery and radiation treatments may be possible during many stages of your pregnancy.
First trimester – (weeks 0-12)
During the first trimester of your pregnancy your baby is developing. All the cells that will make up your baby are busy multiplying during this time. This means that the number of cells is very quickly increasing as your baby develops.
Chemotherapy works by attacking cells that are multiplying quickly. Therefore, chemotherapy is most likely to cause harm to your unborn baby during the first trimester. Chemotherapy during the first trimester can result in deformities, miscarriage or stillbirth.
Your doctor may consider if it is safe to wait until your second trimester to start treatment with chemotherapy.
Monoclonal antibodies work by attaching to specific proteins on the lymphoma cell, and mark the cell for destruction by your immune system. In some cases, these proteins may be present on the cells of your developing baby. However, your doctor will consider the risk versus the benefit to decide if it is better to give you the medicine or wait until the baby is born.
Corticosteroids are medicines that are similar to natural chemicals our bodies make. They are toxic to lymphoma cells, and safe to use during pregnancy. If you need to wait until your second trimester for treatment, you may be given corticosteroids to slow the progression and possibly shrink the lymphoma while you wait for treatment. However, corticosteroids alone will not cure you or put you into remission.
Second trimester – (weeks 13-28)
Third trimester (week 29 until birth)
Treatment in your third trimester is similar to that in your second trimester. The extra consideration during your third trimester is that you will be giving birth. Your doctor may choose to delay your treatments toward the end of your pregnancy, so that your immune system and platelets have time to recover before the birth.
They may also suggest inducing your labour, or performing a caesarean at a time that will allow the least disruption to your treatment while keeping you and your baby safe.
Who should be involved in my healthcare
When you’re pregnant with lymphoma, you will have several healthcare teams involved in your, and your baby’s care. Below are some of the people who should be involved in the decisions about your treatment options, pregnancy and delivery of your baby. There are others listed who can provide supportive care to help with the changes that happen as a result of your pregnancy, or lymphoma and its treatments.
You can ask your doctors to have a ‘multidisciplinary team meeting’ with representatives from each of the teams below involved to help make sure your, and your unborn babies needs are met.
Your support network
Your support network are the people closest to you who you want involved in your care. These can include a partner if you have one, family member, friends or carers. Make sure you let all of your healthcare teams know who you would like involved in your decision making, and what information you are happy for them to share (if any).
Healthcare teams
General practitioner (GP)
Your GP or local doctor should be involved in every aspect of your care. They are often the one who will arrange referrals and can put together management plans for your care. Having lymphoma means you are eligible to have a chronic health management plan done by your GP. This looks at your needs over the next year, and helps you work with your GP to make a plan to make sure all your (and your baby’s) health care needs are met. It allows you to see an allied health service for 5 appointments either free, or heavily discounted. These can include a physiotherapist, occupational therapist, dietician, podiatrist, sexologist and more.
They can also help prepare a mental health care plan that provides you with up to 10 psychology sessions for free or at a discounted rate.
Ask your GP about these health plans.
Haematology/Oncology team
A haematology team is a group of doctors and nurses with a special interest in, and extra training in disorders of the blood including cancers of blood cells. Many people with lymphoma will have a haematology team involved in their care. However, in some cases you may see an oncology team instead. This also consists of doctors and nurses with a special interest in, and extra training in different types of cancer.
Your haematologist or oncologist (doctor) will be involved in helping to diagnose your lymphoma and making decisions about the type of treatment that will be most effective for you.
Radiation oncology or surgical team
If you are having radiation treatment or surgery, you have another team of doctors, nurses and radiation therapists that will be involved in your care. The surgical team may only be involved for a short time before and after treatment. However, your radiation team will become familiar as radiation is usually given everyday, Monday – Friday for between 2 and 7 weeks.
Antenatal team
Your antenatal team are the doctors (obstetrician) and nurses or midwives that have a special interest in looking after you and your baby during your pregnancy. They should be involved in, and kept informed of the decisions made about your treatment while pregnant, and in the weeks and months after pregnancy. They may continue to care for you and your baby after the delivery too.
Psychologist, or counselor
Going through lymphoma or pregnancy is a big deal at any time. Both have life changes outcomes. But when you are going through both at the same time you have a double load to deal with. It is a good idea to speak with a psychologist or counselor to help talk through your feelings and thoughts. They can also help you plan strategies to cope during and after the birth of your baby and lymphoma treatments.
Lactation specialist
If you are having treatment for lymphoma in the weeks leading up to your baby’s birth, or after the birth, you should see a lactation specialist. These can help you as your milk comes in, and help you manage:
- Breastfeeding your baby (if this is safe)
- Expressing your milk to keep producing it.
- Strategies to manage the milk production as you try to stop producing milk.
- How to discard the milk if it cannot be used.
Physiotherapy and/or occupational therapist
A physiotherapist can help you with exercises, strength building and pain management during and after your pregnancy. A physiotherapist may also be able to help with your recovery after childbirth.
An occupational therapist can help assess your extra needs and provide strategies to make your everyday living easier.
Sexologist or sexual health nurse
Pregnancy, childbirth, lymphoma and treatments for lymphoma can change how you feel about your body and sex. It can also change how your body responds to sex and sexual arousal. Sexologists and sexual health nurses are able to help you learn how to cope with changes happening to your body and relationships. They can help you with strategies, advice, exercises and counselling.
Many hospitals have a sexologist or sexual health nurse that specialise in the changes in your body image and sexuality during illness or injury. If you would like to see one, ask your doctor or nurse to arrange a referral for you. If you would like more information on sex, sexuality and intimacy please click the link below.
Fertility Team and family planning
Am I more likely to die from lymphoma because of my pregnancy?
No – not necessarily. Many studies show that your chance of cure or remission are about the same as anyone else who is not pregnant, but has the same:
- subtype of lymphoma
- stage and grade of lymphoma
- age and gender
- treatment
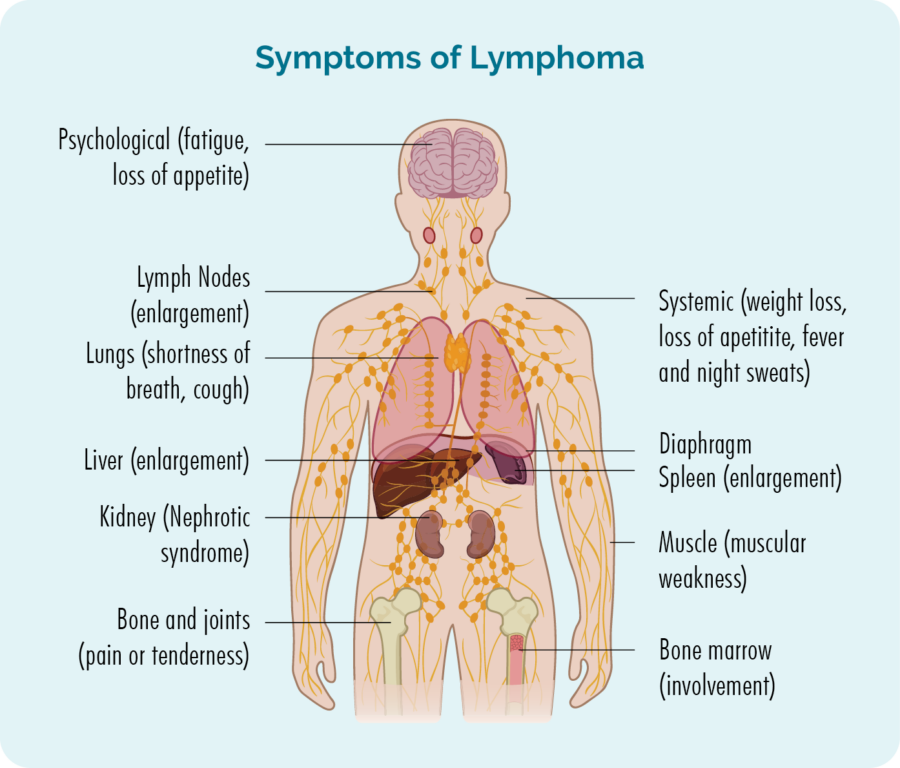
In some cases, it may be harder to diagnose lymphoma during pregnancy, because many of the symptoms of lymphoma are similar to symptoms you get during pregnancy. However, many advanced stage lymphomas can still be cured.
Is there any special consideration for the birth of my baby?
All procedures and childbirth come with risks. However, when you have lymphoma there are extra considerations. The extra things you and your doctors will need to think about, and be prepared for are listed below.
Inducing labour
Your doctor may suggest inducing labour, so that your baby is born earlier than it normally would be. This may be a consideration if:
- Your baby is at a stage of development where they should survive and be healthy if born early.
- Your treatment is urgent.
- Your treatment is likely to do more harm to your baby than an early birth.
Infection risk
Having lymphoma and its treatments puts you at increased risk of infection. This needs to be considered when you have your baby. Childbirth can also increase your risk of infection.
Your doctor may recommend that you stop your treatments several weeks before giving birth to let your immune system recover before the birth.
Bleeding
Your treatments for lymphoma may lower your platelet levels which will increase your risk of bleeding during the birth of your baby.
You may be given a platelet transfusion to increase your platelets before or during the birth. Platelet transfusions are similar to a blood transfusion where you are given platelets that are collected from a donors blood.
Caesarean versus Natural Birth
You may be offered a caesarean. This will depend on your individual circumstances. Talk with your doctor about what the risk are for you for each type of birth.
Can I breastfeed while having treatment?
Many medicines are safe to have while breast feeding. However, some medicines that treat lymphoma may pass to your baby through your breastmilk.
You may need to stop breastfeeding while you are having treatment. If you would like to continue breast feeding after treatment, you may be able to express and discard your milk during treatment to make sure your milk production continues. Talk to you nurses about the best way to discard the milk as you may need to take special precautions if you are having chemotherapy.
Ask to see a lactation specialist for help with managing your breastmilk and breastfeeding (if this is an option). Lactation specialists are nurses that have been specifically trained to help with breast feeding. They can help if you need to stop breastfeeding, or if you would like to continue breastfeeding AFTER treatment.
What support is available for new parents with cancer?
You will have some needs similar to many people with lymphoma or many expectant parents. However, being pregnant and having lymphoma will mean you have some extra needs. There are many organisations, apps and websites that can help. We have listed some of them below.
Lymphoma care nurses – Our nurses are experienced cancer nurses who can help you with information, support and let you know what resources you may be able to access. Click the contact us button at the bottom of the screen for contact details.
Mummies wish – this is an organisation that helps with support and other practical needs of mums with cancer.
Sony Foundation – You can fertility program provides free storage of eggs, sperm embryos and other ovarian and testicular tissue for people aged 13-30 years of age having treatment for cancer.
Apps and websites to help with planning
Frequently asked questions
It is unlikely that you will need to abort your pregnancy if you are diagnosed with lymphoma.
It is only recommended if the lymphoma is creating an immediate threat to your life, and the baby is too young to survive being born.
There are extra considerations with timing of your treatment. However, many babies are born healthy despite the treatments for lymphoma.
Chemotherapy, steroids, and targeted drugs can get into breast milk. Your health care team will give you advice following your treatment on the safety of breastfeeding.
It is rare for a clinical trials to allow participants to join when they are pregnant. This is because your health, and health of your unborn baby is the priority, and it is not known how the products being trialed will affect you or your pregnancy.
However, if you are interested in clinical trials, talk to your doctor. There may be some available for after your baby is born.
Current data suggests that pregnancy does not affect the prognosis of women who have had lymphoma.
Summary
- Healthy babies can still be born when you are diagnosed with lymphoma during pregnancy.
- It is rare that a medical termination (abortion) is needed.
- You may still be able to have treatment when you are pregnant, without it affecting your unborn baby.
- Some treatments may be delayed until you reach the second trimester or until after birth.
- Your doctor may recommend inducing labour to deliver your baby early, if it is safe to do so.
- Many medicines can be passed through your breastmilk, ask your team if it is safe to breastfeed and what precautions you need to take. Ask to see a lactation specialist.
- There is a lot of support available to you, but you may also need to ask for some of the services listed above, as not all will be routinely offered.
- You are not alone. Reach out if you need support. Click the contact us button for contact details.