Overview of Burkitt Lymphoma
Burkitt lymphoma is the most aggressive subtype of lymphoma, and thought to be the fastest growing – or most aggressive type of cancer.
Because it starts and spreads very quickly, it needs to be treated with intensive chemoimmunotherapy very quickly after diagnosis. However, because chemotherapy works best on fast growing cells, it is very affective at destroying Burkitt Lymphoma cells.
Many people with Burkitt Lymphoma can be cured.
Understanding B-cell lymphocytes
Burkitt Lymphoma is a cancer of B-cell lymphocytes, so to understand Burkitt Lymphoma you need to know a bit about your B-Cell lymphocytes.
B-Cell lymphocytes:
- Are a type of white blood cell.
- Fight infection and diseases to keep you healthy.
- Remember infections you had in the past, so if you get the same infection again, your body’s immune system can fight it more effectively and quickly.
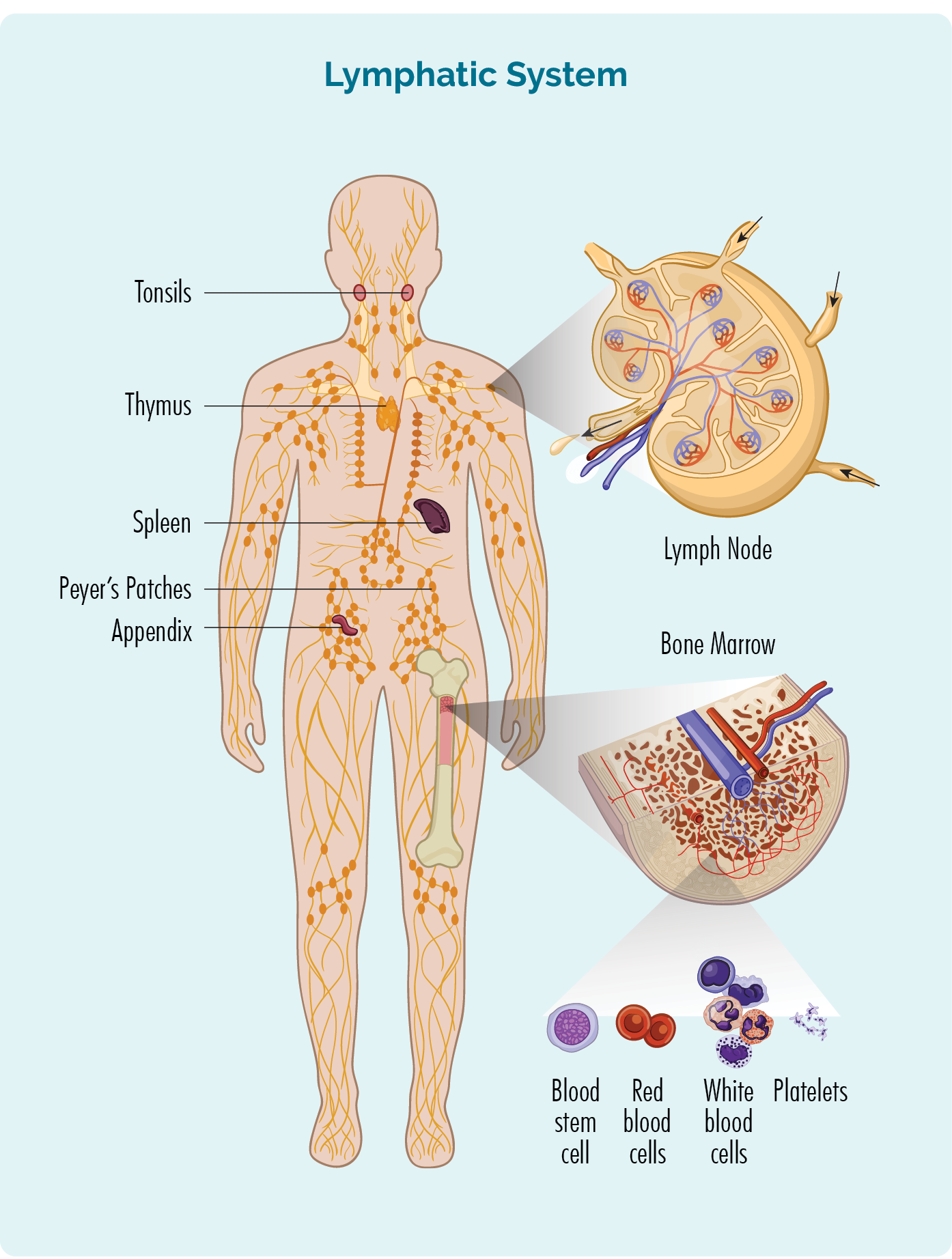
- Are made in your bone marrow (the spongy part in the middle of your bones), but usually live in your spleen and your lymph nodes. Some live in your thymus and blood too.
- Can travel through your lymphatic system, to any part of your body to fight infection or disease.
Burkitt Lymphoma develops when some of your B-cells become cancerous. They grow uncontrollably, are abnormal, and do not die when they should.
When you have Burkitt Lymphoma, your cancerous B-cell lymphocytes:
- Grow and multiply very quickly.
- Will not work as effectively to fight infections and disease.
- Look and behave very differently to your healthy B-cells.
- Can cause lymphoma to develop and grow in many parts of your body.
Subtypes of Burkitt Lymphoma
There are different subtypes of lymphoma. Click on the headings below to learn about the different subtypes.
Endemic Burkitt Lymphoma, which is more common in people with an African background, and is the most common lymphoma in African children. It is also more common in people who have had malaria or Epstein-Barr virus (EBV).
Endemic Burkitt Lymphoma often starts in your jaw, or on other bones of your face, but can also start in your abdomen (tummy).
Sporadic Burkitt Lymphoma can occur in any part of the world and like many lymphomas is thought to be more common in people who have had an infection with the Epstein-Barr virus. It often starts in your abdomen, so it can be common to pain or discomfort in your tummy.
Sporadic Burkitt Lymphoma can spread to your central nervous system, including your brain and spinal cord, your thyroid gland, tonsils and the bones in your face.
Immunodeficiency-associated Burkitt Lymphoma is more common in people with a weakened immune system, and is found in people who have human immunodeficiency virus (HIV) or who have develop acquired immunodeficiency syndrome (AIDS).
However, this subtype can also develop if you take medications that eaken you immune system such as those taken after an organ transplant or if you have an autoimmune disease.
How common is Burkitt Lymphoma?
Burkitt lymphoma affects people of any age, including children and adults. It is the most common type of lymphoma in children aged between 5 and 10 years and makes up 30% of all childhood lymphomas – that means 3 out of every 10 children with lymphoma will have Burkitt Lymphoma.
It is much rarer in adults with only 1 or 2 adults out of every 100 (1-2%) with lymphoma having Burkitt Lymphoma. In adults it is more common in in those aged between 30-50 years.
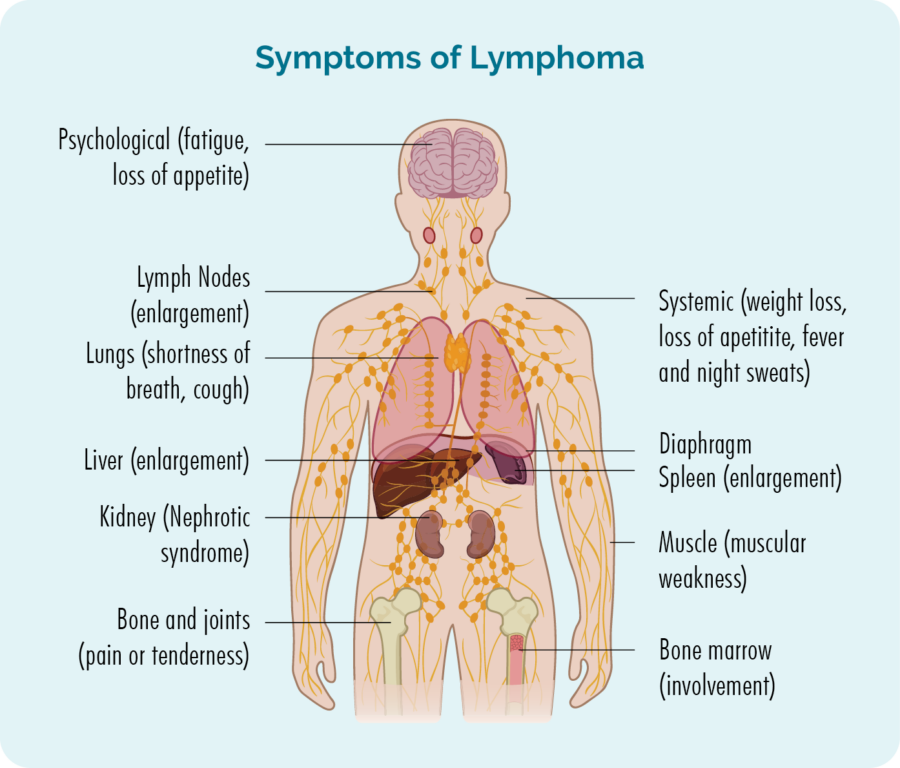
Symptoms of Lymphoma
Some symptoms of Burkitt lymphoma are similar to symptoms of other lymphomas, and others may be related to where the lymphoma is growing.
Common places Burkitt Lymphoma can be found include:
- lymph nodes in your neck, armpit and groin
- your abdomen and bowel
- your central nervous system (CNS) – brain and spinal cord
- bone marrow
- spleen, liver and other organs of your body
- your jaw or other bones in your face.

Nodal and extra nodal Burkitt Lymphoma
Burkitt Lymphoma can start in your lymph nodes or outside of your lymph nodes. When it starts in your lymph nodes it is called “nodal”. When it starts outside of your lymph nodes – such as in your organs or bone marrow it is called “extra nodal”.
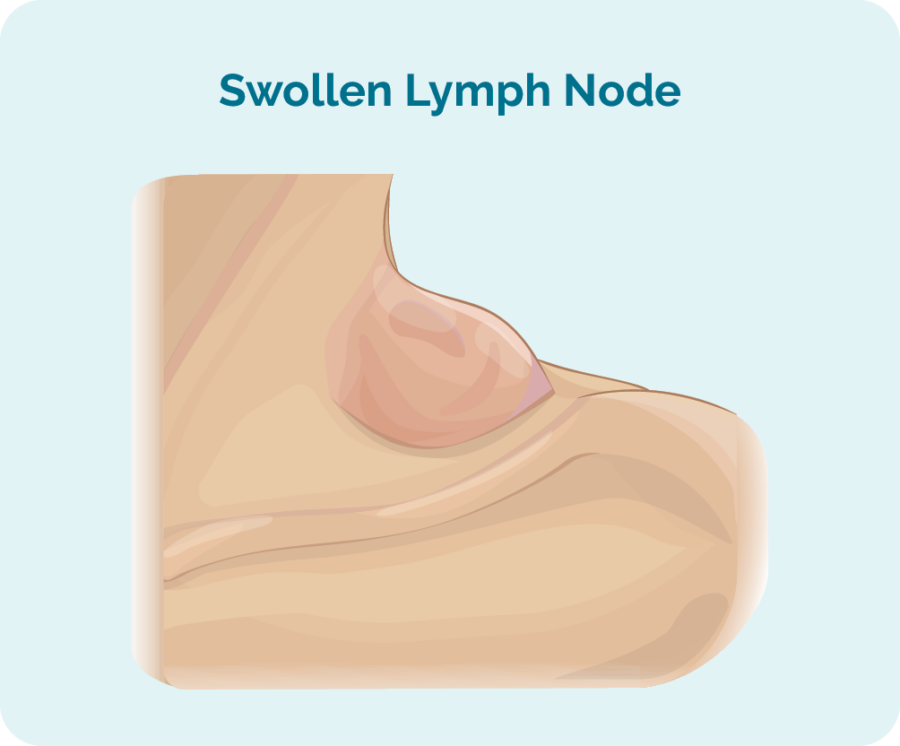
The most common symptom of nodal Burkitt Lymphoma is swollen lymph nodes that can happen in any part of your body. They are more commonly felt in your neck, armpit or groin, because these lymph nodes are closer to your skin.
But we also have lymph nodes in our chest, abdomen, arms, legs and head. Because Burkitt Lymphoma grows and spreads so quickly you may notice lymph nodes in many areas of your body becoming swollen.
Other symptoms of swollen lymph nodes or extranodal lymphoma
Depending on which parts of your body has swollen lymph nodes you may experience different symptoms. Many swollen lymph nodes related to lymphoma are not painful, but they can be painful if they put pressure on other organs, nerves or if they became too big.
In addition to lymph nodes, we also have lymphoid tissue in different parts of our bodies such as our mouth, stomach, bowels, lungs. Lymphoid tissue are areas of immune cells that stay in aareas of our bodies to keep watch for and fight infections. Burkitt Lymphoma can also start or spread to any of these areas too.
Symptoms may include the following.
Area affected | Symptoms |
Chest or neck | Shortness of breath Changes to your voice A persistent cough Pain, pressure or discomfort in chest or neck Changes to heart rhythm if pressure is on your heart |
Central nervous system (Brain, spinal cord and area at the back of your eyes) | Confusion or memory changes Dizziness Changes to your vision Weakness, tingling or burning Difficulty walking Difficulty going to the toilet Seizures (fits) Personality changes |
Gut – (Mouth, stomach & bowels) | Nausea with or without vomiting Diarrhea or constipation Swollen abdomen (you might even look pregnant) Blood when you go to the toilet Feeling full even if you haven’t eaten, or eaten very little Difficulty swallowing. |
Bone Marrow | Changes to your good blood counts including:
|
Organs of your lymphatic system – Spleen and thymus
Your spleen is an organ that filters your blood and keeps it healthy. It is also an organ of your lymphatic system where your B-cell lymphocytes live and produce antibodies to fight infection. It is on the left side of your upper abdomen under your lungs and near your stomach (tummy).
When your spleen gets too big, it can put pressure on your stomach and make you feel full, even if you haven’t eaten very much. You can also get:
- Low blood counts.
- Extreme tiredness.
- Weight loss.
- Jaundice (yellowing of your skin and eyes).
- Pain in your abdomen or a feeling of “bloating”.
Your thymus is also part of your lymphatic system. It is a butterfly shaped organ that sits just behind your breast-bone in the front of your chest. Some B-cells also live and pass through your thymus. If lymphoma is in your thymus you can have a lump in your chest taht can pot pressure on other organs in your chest. Sympoms can be similar as those listed in the table above.
Liver
- Jaundice.
- Pain or discomfort that can radiate up to your left shoulder.
- Loss of appetite and weight loss.
- Swelling of your abdomen due to fluid build-up (ascites).
- Unusual bleeding.
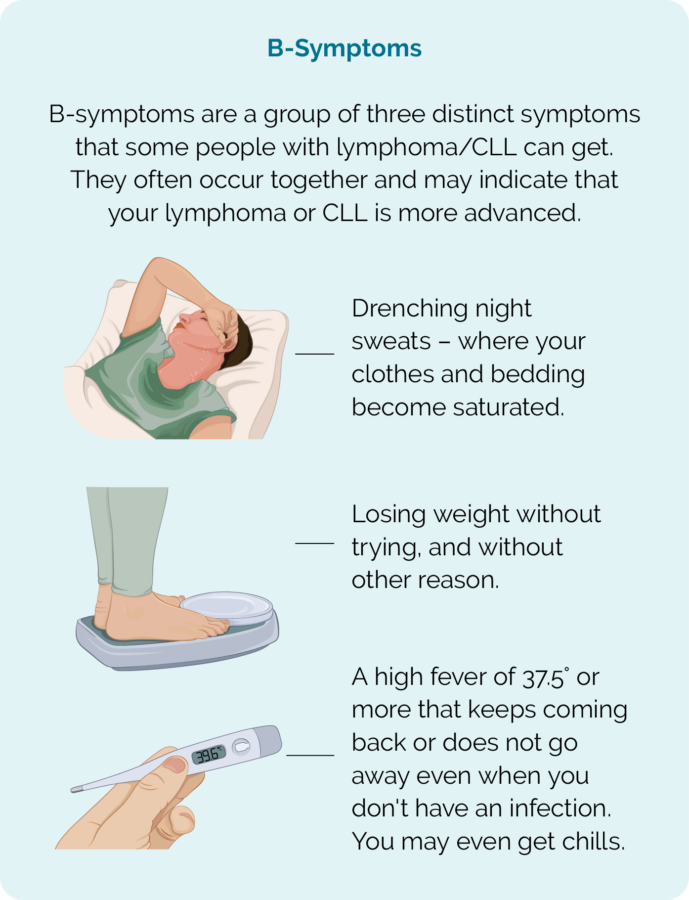
B-symptoms
B-symptoms can occur when lymphoma is actively growing. It can indicate that the lymphoma is using up your energy reserves or is producing chemicals that affect the way your body regulates your temperature. Always report B-symptoms to your doctor.
Diagnosis and Staging of Burkitt Lymphoma
If your doctor thinks that you may have lymphoma, they will need to organise a number of important tests. These tests are needed to either confirm or rule out lymphoma as the cause for your symptoms.
To diagnose Burkitt Lymphoma you will need a biopsy. A biopsy is a procedure to remove part, or all of an affected lymph node and/ or a bone marrow sample. The biopsy is then checked by scientists in a laboratory to see if there are changes that help the doctor diagnose Burkitt’s.
When you have a biopsy, you may have a local or general anaesthetic. This will depend on the type of biopsy and what part of your body it is taken from. There are different types of biopsies and you may need more than one to get the best sample.
Blood tests
Blood tests are taken when trying to diagnose your lymphoma, but also throughout your treatment to make sure your organs are working properly and can cope with our treatment.
Core or fine needle biopsy
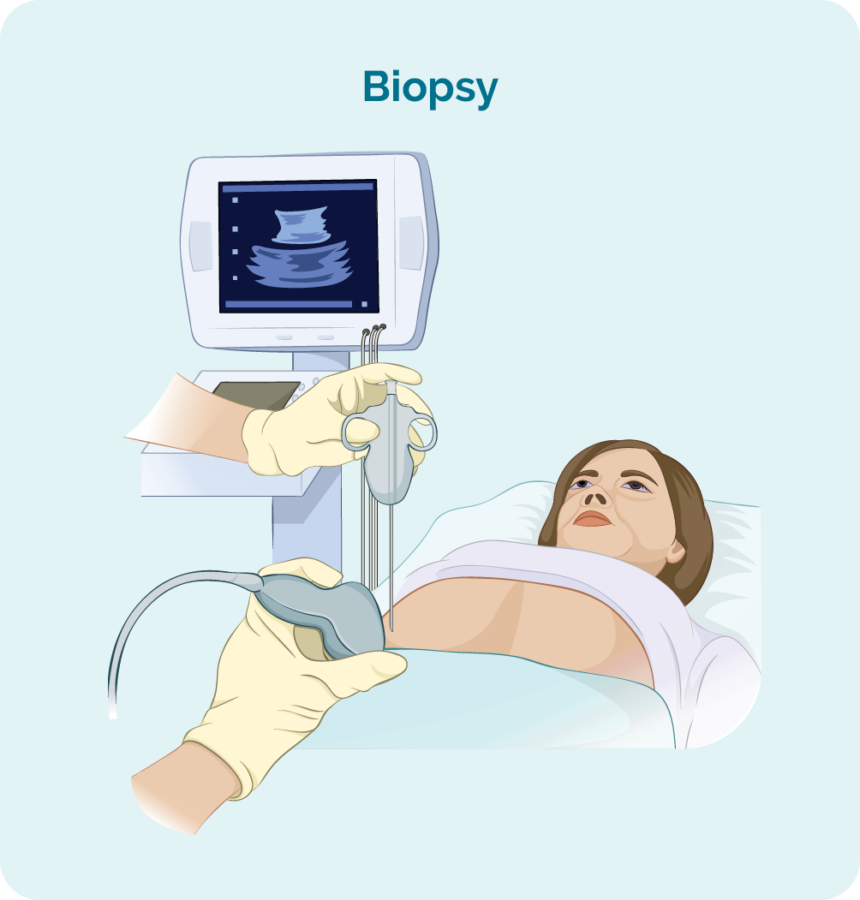
Core or fine needle biopsies are taken to remove a sample of swollen lymph node or tumour to check for signs of lymphoma.
Your doctor will usually use a local anaesthetic to numb the area so you don’t feel any pain during the procedure, but you will be awake during this biopsy. They will then put a needle into the swollen lymph node or lump and remove a sample of tissue.
If your swollen lymph node or lump is deep inside your body the biopsy may be done with the help of ultrasound or specialised x-ray (imaging) guidance.
You might have a general anaesthetic for this (which puts you to sleep for a little while). You may also have a few stitches afterwards.
Core needle biopsies take a bigger sample than a fine needle biopsy.
Excisional node biopsy
Excisional node biopsies are done when your swollen lymph node or tumour are too deep in your body to be reached by a core or fine needle biopsy. You will have a general anaesthetic which will put you to sleep for a little while so you stay still, and feel no pain.
During this procedure, the surgeon will remove the whole lymph node or lump and send it to pathology for testing.
You will have a small wound with a few stitches, and a dressing over the top.
Stitches usually stay in for 7-10 days, but your doctor or nurse will give you instruction on how to care for the dressing, and when to return to have the stitches out.
Burkitt Lymphoma Diagnosis
Once your doctor gets the results from you blood tests and biopsies they will be able to tell you if you have Burkitt Lymphoma and may also be able to tell you what subtype of Burkitt’s you have. They will then want to do more tests to stage and grade your lymphoma.
Staging and Grading Burkitt Lymphoma
Once you have been diagnosed with Burkitt Lymphoma, your doctor will have more questions about your lymphoma. These will include:
- What stage is your lymphoma?
- What subtype of Burkitt’s do you have?
Click on the headings below to learn more about staging and grading.
Staging refers to how much of your body is affected by your lymphoma – or, how far it has spread from where it first started.
B-cells can travel to any part of your body. This means that lymphoma cells (the cancerous B-cells), can also travel to any part of your body. You will need to have more tests done to find this information. These tests are called staging tests and when you get results, you will find out if you have stage one (I), stage two (II), stage three (III) or stage four (IV) Burkitt Lymphoma. However, because Burkitt’s is so aggressive it is often already an advanced stage (stage 3 or 4) when you are diagnosed,
Your stage of lymphoma will depend on:
- How many areas of your body have lymphoma
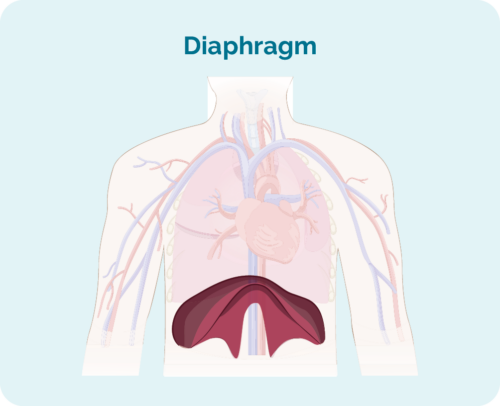
- Where the lymphoma is including if it is above, below or on both sides of your diaphragm (a large, dome-shaped muscle under the rib cage that separates the chest from your abdomen)
- Whether the lymphoma has spread to your bone marrow or other organs such as the liver, lungs, skin or bone.
Stages I and II are called ‘early or limited stage’ (involving a limited area of your body).
Stages III and IV are called ‘advanced stage’ (more widespread).
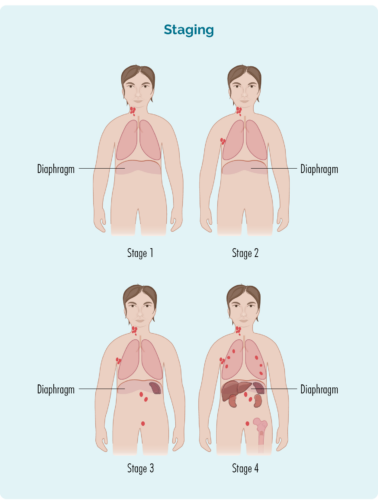
Stage 1 | one lymph node area is affected, either above or below the diaphragm* |
Stage 2 | two or more lymph node areas are affected on the same side of the diaphragm* |
Stage 3 | at least one lymph node area above and at least one lymph node area below the diaphragm* are affected |
Stage 4 | lymphoma is in multiple lymph nodes and has spread to other parts of the body (e.g. bones, lungs, liver) |
Extra staging information
Your doctor may also talk about your stage using a letter, such as A,B, E, X or S. These letters give more information about the symptoms you have or how your body is being affected by the lymphoma. All this information helps your doctor find the best treatment plan for you.
Letter | Meaning | Importance |
A or B |
|
|
E & X |
|
|
S |
|
(Your spleen is an organ in your lymphatic system that filters and cleans your blood, and is a place your B-cells rest and make antibodies) |
Tests for staging
To find out what stage you have, you may be asked to have some of the following staging tests:
Computed tomography (CT) scan
These scans takes pictures of the inside of your chest, abdomen or pelvis. They provide detailed pictures that provide more information than a standard X-ray.
Positron emission tomography (PET) scan
This is a scan that takes pictures of the inside of your whole body. You will be given and needle with some medicine that cancerous cells – such as lymphoma cells absorb. The medicine that helps the PET scan identify where the lymphoma is and the size and shape by highlighting areas with lymphoma cells. These areas are sometimes called “hot”.
Lumbar puncture
A lumbar puncture is a procedure done to check if you have any lymphoma in your central nervous system (CNS), which includes your brain, spinal cord and an area around your eyes. You will need to say very still during the procedure, so babies and children may have a general anaesthetic to put them to sleep for a little while the procedure is done. Most adults will only need a local anaesthetic for the procedure to numb the area.
Your doctor will put a needle into your back, and take out a little bit of fluid called “cerebral spinal fluid” (CSF) from around your spinal cord. CSF is a fluid that acts a bit like a shock absorber to your CNS. It also carries different proteins and infection fighting immune cells such as lymphocytes to protect your brain and spinal cord. CSF can also help drain any extra fluid you may have in your brain or around your spinal cord to prevent swelling in those areas.
The CSF sample will then be sent to pathology and checked for any signs of lymphoma.
Bone marrow biopsy
- Bone marrow aspirate (BMA): this test takes a small amount of the liquid found in the bone marrow space.
- Bone marrow aspirate trephine (BMAT): this test takes a small sample of the bone marrow tissue.
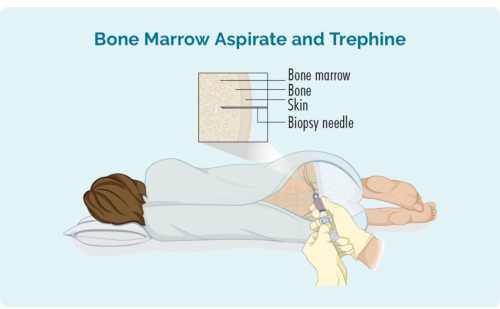
The samples are then sent to pathology where they are checked for signs of lymphoma.
The process for bone marrow biopsies can differ depending on where you are having your treatment, but will usually include a local anaesthetic to numb the area.
In some hospitals, you may be given light sedation which helps you to relax and can stop you from remembering the procedure. However many people do not need this and may instead have a “green whistle” to suck on. This green whistle has a pain killing medication in it (called Penthrox or methoxyflurane), that you use as needed throughout the procedure.
Make sure you ask your doctor what is available to make you more comfortable during the procedure, and talk to them about what you think will be the best option for you.
More information on bone marrow biopsies can be found at our webpage here.
Burkitt Lymphoma is the most aggressive lymphoma subtype and most aggressive cancer. Therefore, it is always considered a high-grade lymphoma.
The grade refers to how quickly the cells are multiplying, what they look like and how they behave.
High grade lymphoma cells multiply very quickly, look very different from your normal B-cell lymphocytes and are unable to function the way lymphocytes should function.
Low risk and High risk Burkitt Lymphoma
Your doctor may also refer to your Burkitt’s as high risk or low risk. This is extra information they use to determine the best treatment for you. Your risk will be determined based on the following:
- Whether you have lymphoma in your central nervous system (CNS).
- If your blood tests show a high lactate dehydrogenase (LDH).
- If you have any genetic rearrangements or changes.
Cytogenetic testing
Cytogenetic tests are done to check for genetic variances that may be involved in your disease. For more information on these please see our section on understanding your lymphoma genetics further down on this page. The tests used to check for any genetic mutations are called cytogenetic tests. These tests look to see if you have any changed in chromosomes and genes.
We usually have 23 pairs of chromosomes, and they are numbered according to their size. When you have Burkitt Lymphoma, your chromosomes may look a little different.
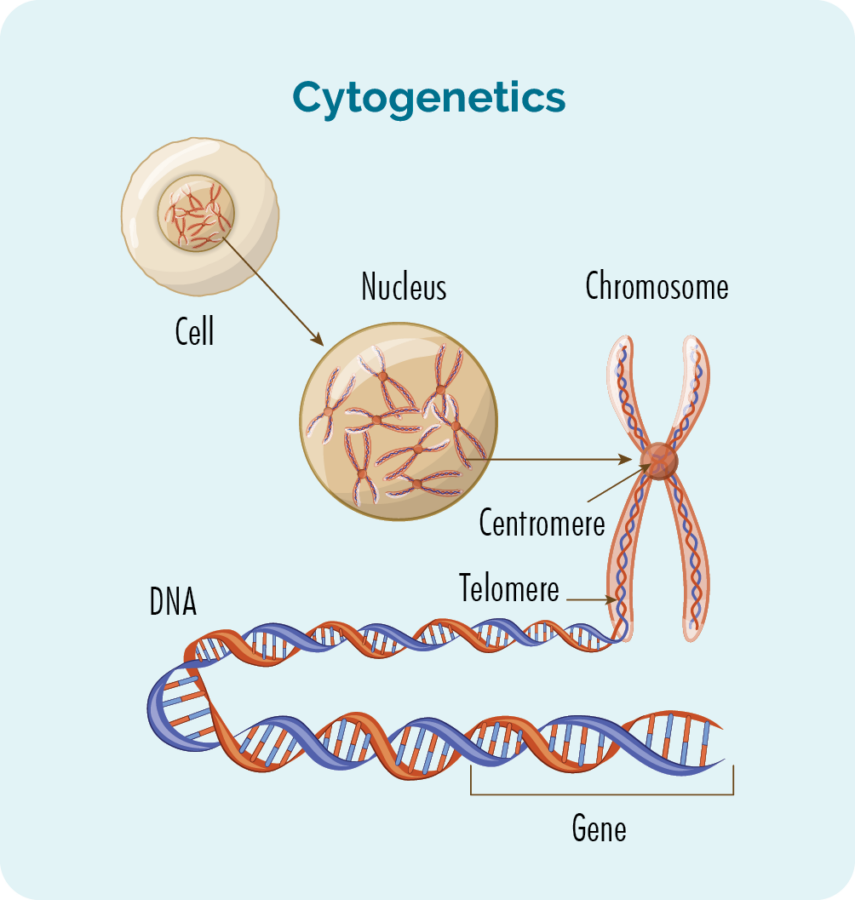
What are genes and chromosomes
Each cell that makes up our body has a nucleus, and inside the nucleus are the 23 pairs of chromosomes. Each chromosome is made from long strands of DNA (deoxyribonucleic acid) that contain our genes. Our genes provide the code needed to make all the cells and proteins in our body, and tells them how to look or act.
If there is a change (variation) in these chromosomes or genes, your proteins and cells will not work properly.
Lymphocytes can become lymphoma cells due to genetic changes (called mutations or variations) within the cells. Your lymphoma biopsy may be looked at by a specialist pathologist to see if you have any gene mutations.
Translocation in Burkitt Lymphoma
In Burkitt Lymphoma you will have variation in your genes called a translocation. This happens when a small part of two chromosomes swap places. The gene always affected Burkitt Lymphoma includes the MYC gene on 8th chromosome with the translocation happening with a gene on the 14th chromosome. You will see it written as t(8:14).
Treatment for Burkitt Lymphoma
Once all of your results from the biopsy, cytogenetic testing and the staging scans have been completed, the doctor will review these to decide the best possible treatment for you. At some cancer centres, the doctor will also meet with a team of specialists to discuss the best treatment option. This is called a multidisciplinary team (MDT) meeting.
Your doctor will consider many factors about your Burkitt Lymphoma, but you will need to start treatment with chemo-immunotherapy very soon after diagnosis. Without treatment Burkitt Lymphoma is fatal, however with treatment there is a very good chance of being cured.
Chemo-immunotherapy means having medications that called chemotherapy and a monoclonal antibody. Monoclonal antibodies are often called immunotherapy because they help your immune system fight the cancer. Chemotherapy works by directly attacking fast growing cells.
Other things your doctor will consider when planning your treatment include your:
- individual stage of lymphoma, genetic changes and symptoms
- age, past medical history and general health
- current physical and mental wellbeing and patient preferences
- any symptoms you are getting.
Other tests
More tests may be ordered before you start treatment to make sure your heart, lungs and kidneys are able to cope with the treatment. These may include an ECG (electrocardiogram), lung function test or 24-hour urine collection.
Your doctor or cancer nurse can explain your treatment plan and the possible side-effects to you, and are there to answer any question you might have. It is important you ask your doctor and/or cancer nurse questions about anything you don’t understand.
You can also phone or email the Lymphoma Australia Nurse Helpline with your questions and we can help you to get the right information.
Lymphoma care nurse hotline:
Phone: 1800 953 081
Email: nurse@lymphoma.org.au
Questions to ask your doctor before you start treatment
It can be difficult to know what questions to ask when you are starting treatment. If you don’t know, what you don’t, how can you know what to ask?
Having the right information can help you feel more confident and know what to expect. It can also help you plan ahead for what you may need.
We put together a list of questions you may find helpful. Of course, everyone’s situation is unique, so these questions do not cover everything, but they do give a good start.
Click on the link below to download a printable PDF of questions for your doctor.
Fertility Preservation
Treatment for Burkitt Lymphoma can affect your fertility (ability to have babies). This can happen for both adults and children, males and females. If you (or your child) would like children later in life, talk to your doctor about whether your fertility can be protected for later on.
Common Treatment Protocols for Adults with Burkitt Lymphoma
Your treatment usually works very well against your lymphoma, but can also affect your good cells. So you need time for your good cells to recover. Healthy cells revocer much more quickly than lymphoma cells because they are lot more organised.
Common treatment protocols you may be offered include:
DA-R-EPOCH (dose adjusted rituximab, etoposide, prednisolone, vincristine, cyclophosphamide, doxorubicin)
R-CODOX-M (rituximab, cyclophosphamide, vincristine, doxorubicin, methotrexate)
- R-CODOX-M is alternated with R-IVAC (rituximab, ifosfamide, etoposide, cytarabine)
GMALL 2002 (patients over 55 years)
GMALL 2002 (patients under 55 years)
Hyper CVAD part A
- Hyper CVAD part A is alternated with Hyper CVAD Part B
Common Treatment Protocols for Children with Burkitt Lymphoma
- R-COPADM: rituximab, cyclophosphamide, vincristine, methotrexate, cytarabine, Prednisolone, doxorubicin, etoposide.
- SFOP LMB 89: cyclophosphamide, vincristine, methotrexate, doxorubicin), cytarabine, etoposide
Other variations of chemotherapy protocols used in paediatric Burkitt lymphoma include:
- CHOP: cyclophosphamide, daunorubicin, vincristine and prednisolone
- COPAD: cyclophosphamide, cytarabine, doxorubicin, vincristine, etoposide, Prednisolone
- COPADM: cyclophosphamide, methotrexate, cytarabine, doxorubicin, vincristine, etoposide
Relapsed or Refractory Burkitt Lymphoma
In some cases, your lymphoma may not respond to the first-line of treatment you have. When this happens, your lymphoma is called refractory.
Other times, you may get a good response from your treatment, but the lymphoma can relapse (come back) after a period of time.
For both refractory and relapsed Burkitt Lymphoma you will be offered more treatment.
Treatments in the second or third-line can include:
- more immuno-chemotherapy
- stem cell transplant
- CAR T-cell therapy
For more information on treatments and things to consider see our treatments page.
Clinical trials
It is recommended that anytime you need to start new treatments you ask your doctor about clinical trials you may be eligible for.
Clinical trials are important to find new medicines, or combinations of medicines to improve treatment of Burkitt Lymphoma in the future.
They can also offer you a chance to try a new medicine, combination of medicines or other treatments that you would not be able to get outside of the trial. If you are interested in participating in a clinical trial, ask your doctor what clinical trials you are eligible for.
There are many treatments and new treatment combinations that are currently being tested in clinical trials around the world for patients with both newly diagnosed and relapsed Burkitt Lymphoma.
Prognosis for Burkitt Lymphoma – and what happens when treatment ends
Prognosis is the term used to describe the likely path of your disease, how it will respond to treatment and how you will do during and after treatment.
There are many factors that contribute to your prognosis and it is not possible to give an overall statement about prognosis. However, Burkitt Lymphoma often responds very well to treatment and many patients with this cancer can be cured – meaning after treatment, there is no sign of Burkitt Lymphoma in your body. However, there is a small group of people that may not respond as well to treatment.
Factors that can impact prognosis
Some factors that may impact your prognosis include:
- You age and overall health at time of diagnosis.
- How you respond to treatment.
- What if any genetic mutations you have.
- The subtype of Burkitt Lymphoma you have.
If you would like to know more about your own prognosis, please talk with your specialist haematologist or oncologist. They will be able to explain your risk factors and prognosis to you.
Survivorship - Living with, and after cancer
A healthy lifestyle, or some positive lifestyle changes after treatment can be a great help to your recovery. There are many things you can do to help you live well after Burkitt’s.
Many people find that after a cancer diagnosis, or treatment, that their goals and priorities in life change. Getting to know what your ‘new normal’ is can take time and be frustrating. Expectations of your family and friends may be different to yours. You may feel isolated, fatigued or any number of different emotions that can change each day.
The main goals after treatment for your lymphoma is to get back to life and:
- be as active as possible in your work, family, and other life roles
- lessen the side effects and symptoms of the cancer and its treatment
- identify and manage any late side effects
- help keep you as independent as possible
- improve your quality of life and maintain good mental health
Different types of cancer rehabilitation may be recommended to you. This could mean any of a wide range of services such as:
- physical therapy, pain management
- nutritional and exercise planning
- emotional, career and financial counselling.
Summary
- Burkitt Lymphoma is the most aggressive type of cancer you can get – but this means it usually responds very well to treatment.
- Many people with Burkitt Lymphoma can be cured.
- Burkitt Lymphoma happens when your B-cell lymphocytes become cancerous and can affect children and adults.
- You will need treatment with chemo-immunotherapy very soon after you are diagnosed.
- In some cases, your lymphoma may not respond to treatment, or it may relapse after treatment and you will need more treatment if this happens.
- Ask your doctor about clinical trials you may be eligible for.