B-cell lymphocytes in Diffuse Large B-cell Lymphoma (DLBCL)
To understand DLBCL you need to know a bit about your B-Cell lymphocytes.
B-Cell lymphocytes:
- Are a type of white blood cell
- Fight infection and diseases to keep you healthy.
- Remember infections you had in the past, so if you get the same infection again, your body’s immune system can fight it more effectively and quickly.
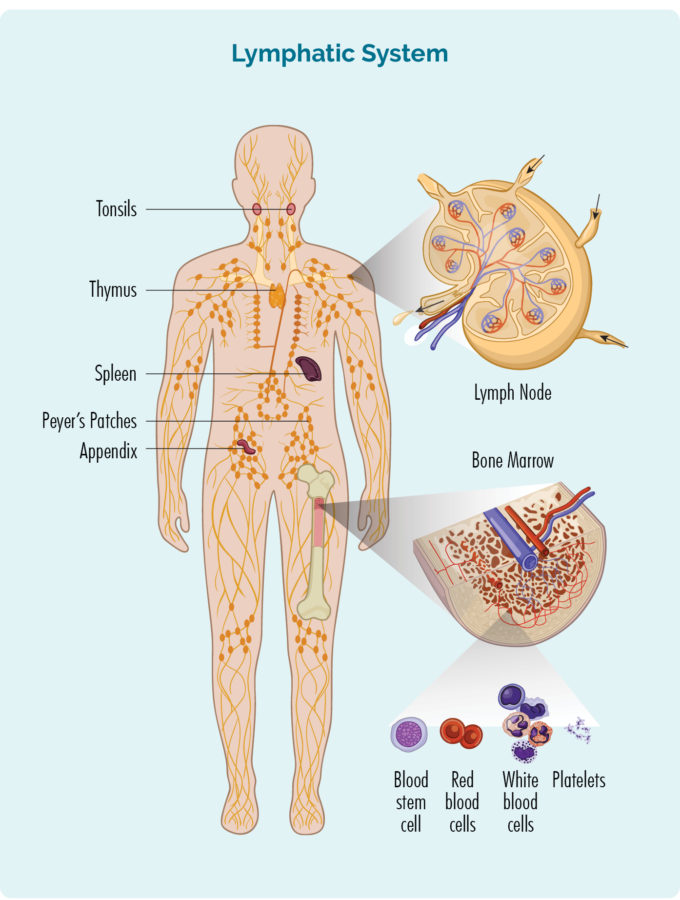
- Are made in your bone marrow (the spongy part in the middle of your bones), but usually live in your spleen and your lymph nodes. Some live in your thymus and blood too.
- Can travel through your lymphatic system, to any part of your body to fight infection or disease.
DLBCL develops when some of your B-cells become cancerous and are spread out (diffuse) rather than grouped closely together. They grow uncontrollably, are abnormal, and do not die when they should.
Although DLBCL is usually a fast growing (aggressive) lymphoma, many people with DLBCL can be cured with treatment, even if you are diagnosed with an advanced stage. An advanced stage of lymphoma is very different to advanced stages of other cancers which cannot be cured.
Causes of Diffuse Large B-cell Lymphoma (DLBCL)
We don’t know what causes DLBCL, but different risk factors are thought to increase your risk of developing it. Some, risk factors for DLBCL are thought to include the following if you:
- Have a condition affecting your immune system such as human immunodeficiency virus (HIV).
- Are taking medicines that suppress your immune system, such as those taken after an organ transplantation.
- Have a family member with lymphoma.
- Have hepatitis C – a virus affecting your liver.
- Were overweight as a child.
*It is important to note, not all people who have these risk factors will develop DLBCL, and some people with none of those risk factors can develop DLBCL.
For an overview of DLBCL presented by haematologist Michael Dickinson please watch the below video.
Symptoms of Diffuse Large B-cell Lymphoma (DLBCL)
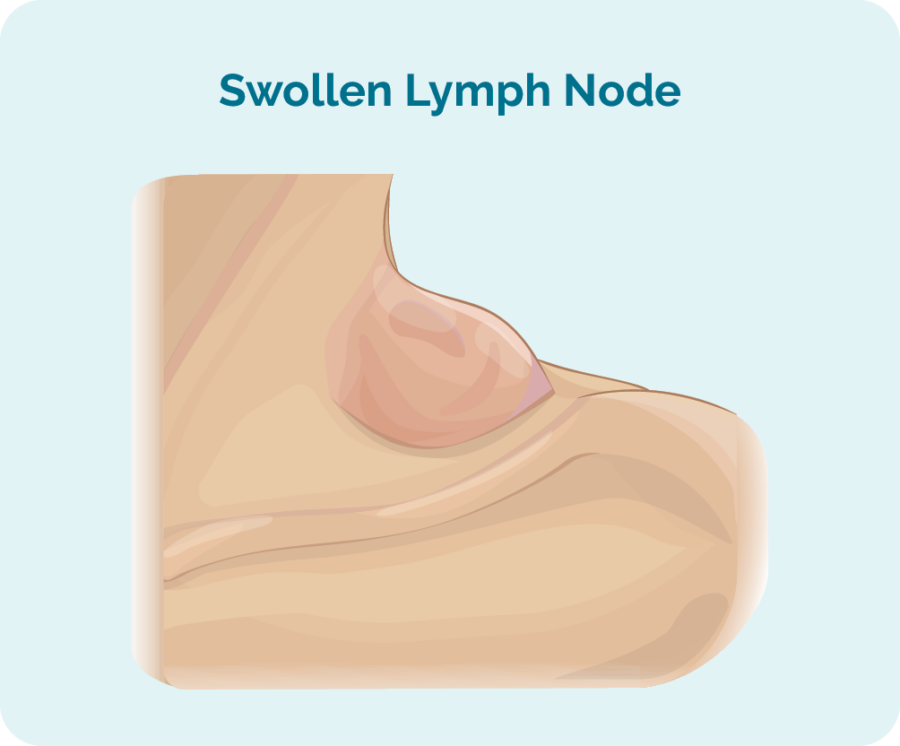
The first sign or symptom of DLBCL you get may be a lump, or several lumps that continue to grow. You might feel or see them on your neck, armpit or groin. These lumps are enlarged lymph nodes (glands), swollen by having too many cancerous B-cells growing in them.
They often start in one part of your body, and then spread throughout your lymphatic system and to other parts of your body including your:
- spleen
- thymus
- lungs
- liver
- bones
- bone marrow
- central nervous system (CNS)
- other organs
Organs of your lymphatic system – Spleen and thymus
Your spleen is an organ that filters your blood and keeps it healthy. It is also an organ of your lymphatic system where your B-cell lymphocytes live and produce antibodies to fight infection. It is on the left side of your upper abdomen under your lungs and near your stomach (tummy).
When your spleen gets too big, it can put pressure on your stomach and make you feel full, even if you haven’t eaten very much.
Your thymus is also part of your lymphatic system. It is a butterfly shaped organ that sits just behind your breast bone in the front of your chest. Some B-cells also live and pass through your thymus.
Depending on where you DLBCL is growing you may have different symptoms as listed below.
Symptoms of DLBCL (Table one)
Area affected | Symptoms |
Gut – including your stomach and bowel | Nausea with or without vomiting (feeling sick in your tummy or throwing up). Diarrhoea or constipation (watery or hard poo). Blood when you go to the toilet. Feeling full even if you haven’t eaten much. |
Central nervous system (CNS) – including your brain and spinal cord | Confusion or memory changes. Personality changes. Seizures. Weakness, numbness, burning or pins and needles in your arms and legs. |
Chest | Shortness of breath Chest pain A dry cough |
Bone marrow | Low blood counts including red cells, white cells and platelets resulting in: o Shortness of breath. o Infections that deep coming back or are difficult to get rid of. o Unusual bleeding or bruising. |
Skin | Red or purple looking rash. Lumps and bumps on your skin which may be skin coloured or red or purple. Itching. |
General symptoms of lymphoma
General symptoms of lymphoma may include:
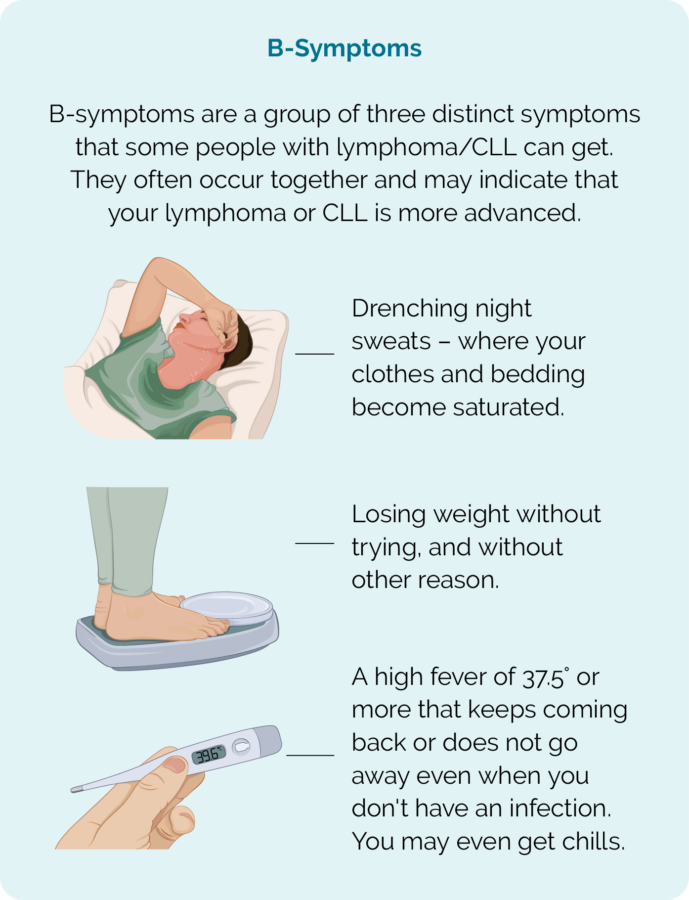
- B-symptoms – see picture below
- swollen lymph nodes (glands)
- feeling unusually tired (fatigued)
- feeling out of breath
- itchy skin
- infections that don’t go away or keep coming back
- changes to your blood tests
- low red cells and platelets
- too many lymphocytes and/or lymphocytes that do not work properly
- lowered white cells (including neutrophils)
- high lactic acid dehydrogenase (LDH) – a type of protein used to make energy. If your cells are damaged by your lymphoma, LDH can spill out of your cells and into your blood
- high beta-2 microglobulin – a type of protein made by lymphoma cells. It can be found in your blood, urine or cerebral spinal fluid
When to contact your doctor
You should contact your doctor if:
- you have swollen lymph nodes that do not go away, or if they are larger than you would expect for an infection
- you are often short of breath without reason
- you are more tired than usual and it does not get better with rest or sleep
- you notice unusual bleeding or bruising (including in our poo, from your nose or gums)
- you develop an unusual rash (a purple of red spotty rash can mean you have some bleeding under your skin)
- your skin is more itchy than usual
- you develop a new dry cough
- you experience B symptoms
It’s important to note that many of the signs and symptoms of DLBCL can be related to causes other than cancer. For example, swollen lymph nodes can also happen if you have an infection. Usually though, if you have an infection, the symptoms will improve and the lymph nodes will return to normal size in a few weeks.
With lymphoma, these symptoms will not go away. They may even get worse.
How is Diffuse Large B-cell Lymphoma (DLBCL) diagnosed
Diagnosing DLBCL can sometimes be difficult and can take several weeks.
If your doctor thinks that you may have lymphoma, they will need to organise a number of important tests. These tests are needed to either confirm or rule out lymphoma as the cause for your symptoms. Because there are several different subtypes of DLBCL, you may have extra tests to find out which one you have. This is important because the management and treatment of your subtype may be different to other subtypes of DLBCL.
Staging and Grading Diffuse Large B-cell Lymphoma (DLBCL)
Once you have been diagnosed with DLBCL, your doctor will have more questions about your lymphoma. These will include:
- What stage is your lymphoma?
- What grade is your lymphoma?
- What subtype of DLBCL do you have?
Click on the headings below to learn more about staging and grading.
Staging refers to how much of your body is affected by your lymphoma – or how far it has spread from where it first started.
B-cells can travel to any part of your body. This means that lymphoma cells (the cancerous B-cells), can also travel to any part of your body. You will need to have more tests done to find this information. These tests are called staging tests and when you get results, you will find out if you have stage one (I), stage two (II), stage three (III) or stage four (IV) DLBCL.
Your stage of DLBCL will depend on:
- How many areas of your body have lymphoma
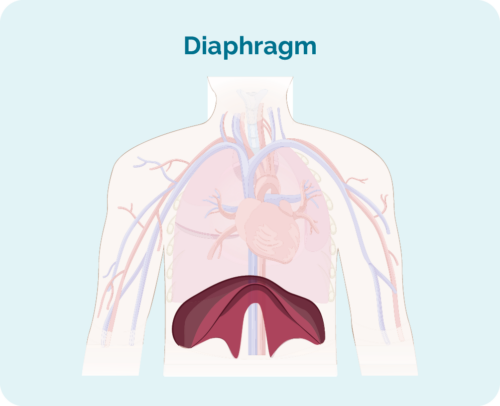
- Where the lymphoma is including if it is above, below or on both sides of your diaphragm (a large, dome-shaped muscle under your rib cage that separates your chest from your abdomen)
- Whether the lymphoma has spread to your bone marrow or other organs such as your liver, lungs, skin or bone.
Stages I and II are called ‘early or limited stage’ (involving a limited area of your body).
Stages III and IV are called ‘advanced stage’ (more widespread).
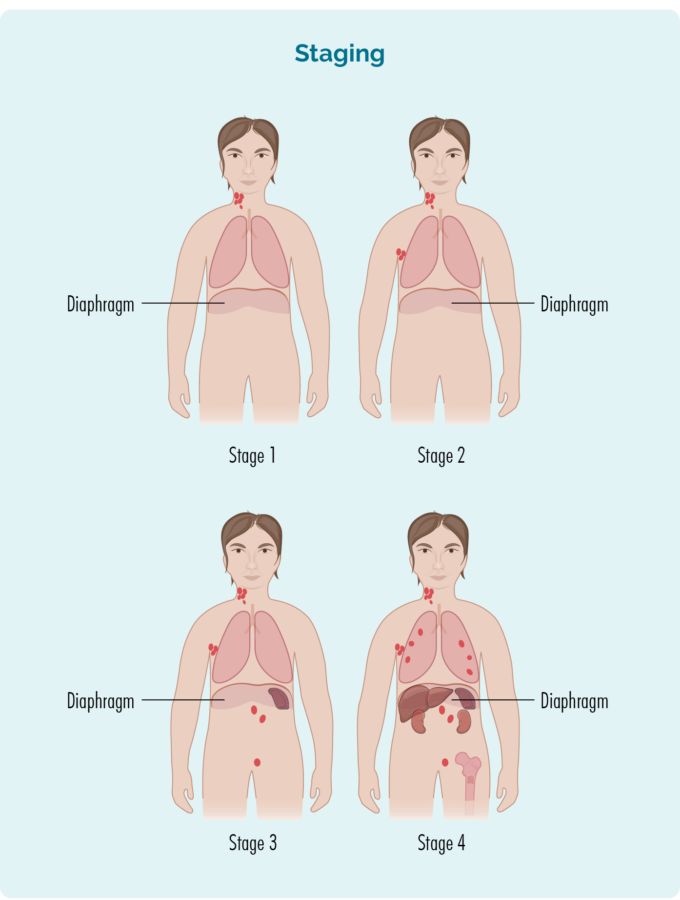
Stage 1 | One lymph node area is affected, either above or below the diaphragm*. |
Stage 2 | Two or more lymph node areas are affected on the same side of the diaphragm*. |
Stage 3 | At least one lymph node area above and at least one lymph node area below the diaphragm* are affected. |
Stage 4 | Lymphoma is in multiple lymph nodes and has spread to other parts of the body (e.g. bones, lungs, liver). |
Extra staging information
Your doctor may also talk about your stage using a letter, such as A,B, E, X or S. These letters give more information about the symptoms you have or how your body is being affected by the lymphoma. All this information helps your doctor find the best treatment plan for you.
Letter | Meaning | Importance |
A or B |
|
|
E & X |
|
|
S |
|
(Your spleen is an organ in your lymphatic system that filters and cleans your blood, and is a place your B-cells rest and make antibodies) |
Tests for staging
To find out what stage you have, you may be asked to have some of the following staging tests:
Computed tomography (CT) scan
These scans takes pictures of the inside of your chest, abdomen or pelvis. They provide detailed pictures that provide more information than a standard X-ray.
Positron emission tomography (PET) scan
This is a scan that takes pictures of the inside of your whole body. You will be given and needle with some medicine that cancerous cells – such as lymphoma cells absorb. The medicine that helps the PET scan identify where the lymphoma is and the size and shape by highlighting areas with lymphoma cells. These areas are sometimes called “hot”.
Lumbar puncture
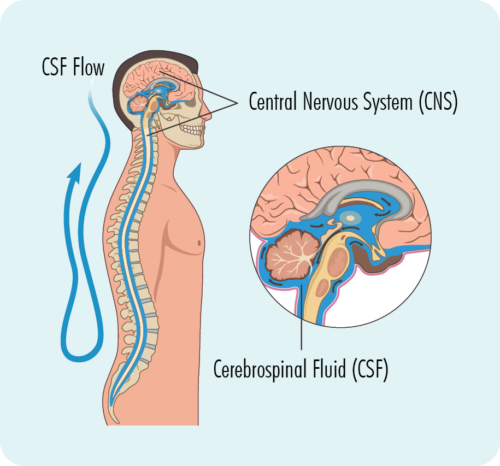
A lumbar puncture is a procedure done to check if you have any lymphoma in your central nervous system (CNS), which includes your brain, spinal cord and an area around your eyes. You will need to stay very still during the procedure, so babies and children may have a general anaesthetic to put them to sleep for a little while when the procedure is done. Most adults will only need a local anaesthetic for the procedure to numb the area.
Your doctor will put a needle into your back, and take out a little bit of fluid called “cerebral spinal fluid” (CSF) from around your spinal cord. CSF is a fluid that acts a bit like a shock absorber to your CNS. It also carries different proteins and infection fighting immune cells such as lymphocytes to protect your brain and spinal cord. CSF can also help drain any extra fluid you may have in your brain or around your spinal cord to prevent swelling in those areas.
The CSF sample will then be sent to pathology and checked for any signs of lymphoma.
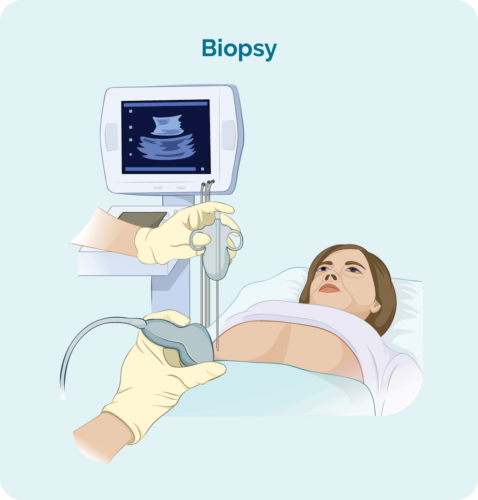
Bone marrow biopsy
- Bone marrow aspirate (BMA): this test takes a small amount of the liquid found in the bone marrow space.
- Bone marrow aspirate trephine (BMAT): this test takes a small sample of the bone marrow tissue.
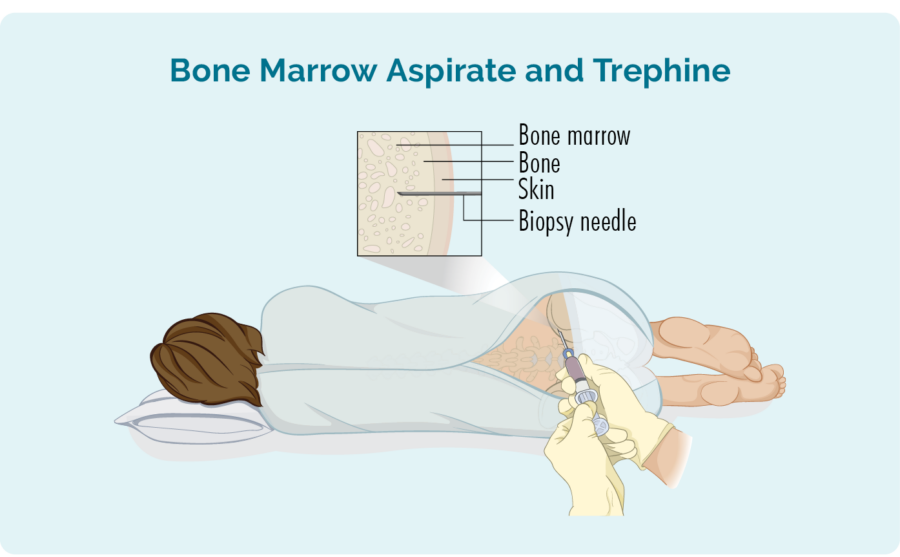
The samples are then sent to pathology where they are checked for signs of lymphoma.
The process for bone marrow biopsies can differ depending on where you are having your treatment, but will usually include a local anaesthetic to numb the area.
In some hospitals, you may be given light sedation which helps you to relax and can stop you from remembering the procedure. However many people do not need this and may instead have a “green whistle” to suck on. This green whistle has a pain killing medication in it (called Penthrox or methoxyflurane), that you use as needed throughout the procedure.
Make sure you ask your doctor what is available to make you more comfortable during the procedure, and talk to them about what you think will be the best option for you.
More information on bone marrow biopsies can be found at our webpage here.
Your lymphoma cells have a different growth pattern, and look different to normal cells. The grade of your lymphoma is how quickly your lymphoma cells are growing, which affects the way look under a microscope. The grades are Grades 1-4 (low, intermediate, high). If you have a higher grade lymphoma, your lymphoma cells will look the most different from normal cells, because they are growing too quickly to develop properly. An overview of the grades is below.
- G1 – low grade – your cells look close to normal, and they grow and spread slowly.
- G2 – intermediate grade – your cells are starting to look different but some normal cells exist, and they grow and spread at a moderate rate.
- G3 – high grade – your cells look fairly different with a few normal cells, and they grow and spread faster.
- G4 – high grade – your cells look most different to normal, and they grow and spread the fastest.
All this information adds to the whole picture your doctor builds to help decide the best type of the treatment for you.
It is important that you talk to your doctor about your own risk factors so you can have clear idea of what to expect from your treatments.
Subtypes of Diffuse Large B-cell Lymphoma (DLBCL)
There are many subtypes of DLBCL. The two main subtypes are named based on the specific cell your lymphoma began growing from. The most common is “Activated B-cell (ABC)”, with about half of all patients with DLBCL having this subtype. The other main subtype of DLBCL is “Germinal Cell B-cell (GCB)”, with about 3 in every 10 people with DLBCL having this subtype.
Your doctor can tell whether you have the GCB or ABC subtype by looking at your lymphoma cells in pathology. The two subtypes look different by having different proteins on the surface of the cells, and different genetic mutations.
Once your doctor and treating team know if you have GCB or ABC, they may do additional cytogenetic tests on your lymphoma cells. These tests check for other genetic changes in your chromosomes and genes (called rearrangements). You can find more information on this further down this page under the heading “Understanding your lymphoma genetics”.
DLBCL can also be called nodal or extra-nodal. Nodal means that it started in your lymph nodes, whereas extra-nodal means it started outside of your lymphatic system. Some extra-nodal places that DLBCL can start include your skin, breasts, testicles, liver, lung, bone, brain, stomach or bowels.
Click on the banners below if you would like to learn more about the other subtypes of DLBCL that make up the remainder of cases.
Primary mediastinal B-cell lymphoma (PMBCL) is a rare aggressive (fast-growing) type of non-Hodgkin Lymphoma. It used to be classified as a sub-type of DLBCL, but has now been reclassified by the World Health Organisation as a subtype on its own.
For more information on PMBCL, please see our Primary Mediastinal B – cell lymphoma (PMBCL) webpage here, or our factsheet here.
T-cell/histiocyte rich B-cell lymphoma (T/HRBCL) is a rare subtype of DLBCL that can be very difficult for your doctor to diagnose. It is difficult to diagnose because it looks a lot like two other subtypes of lymphoma. For this reason, some people with T/HRBCL can get a wrong diagnosis of Hodgkin’s lymphoma or peripheral T-cell lymphoma, before getting the right diagnosis. You will need some special tests to diagnose T/HRBCL called immunohistochemistry tests. This is a special test done on your biopsies so your doctor can learn more about your lymphoma.
T-cells are another type of lymphocyte cell that helps your immune system remember infections you’ve had in the past. They help to keep your immune system in check so it doesn’t work too hard, and also supports other cells of your immune system to work more effectively. Histiocytes are also a type or immune cell called a phagocyte. Phagocytes help to protect you from infection and disease because they recognise the bad cells and eat them.
If you have T/HRBCL – you have too many T-cells and histiocytes (which is why it’s called “rich” – T/HR) while also having cancerous B-cell lymphocytes (BCL).
Standard treatment for T/HRBCL is the same as most other subtypes of diffuse large B-cell lymphoma (DLBCL), discussed later on this webpage.
EBV-positive DLBCL not otherwise specified is a subtype of DLBCL that can occur in young people, but most commonly affects people over 50 years of age. It occurs in some people who have had a virus called Epstein-Barr virus (EBV), which affects B-cells. EBV causes glandular fever (also called “mono” or the kissing disease). However, only a very small number of people who have had EBV go on to develop EBV-positive DLBCL. Unfortunately we currently have no way of knowing who will develop this lymphoma after infection with EBV.
Symptoms will depend on where your lymphoma is growing. It usually starts in your lymph nodes (called nodal lymphoma) which can cause a new lump to come up. This is usually in your neck, armpit, groin or tummy, but can be anywhere in your body.
Other places it can grow and the symptoms associated with it are similar to those listed above in table one.
Standard treatment for intravascular large B-cell lymphoma is the same as most other subtypes of diffuse large B-cell lymphoma (DLBCL), discussed later on this webpage.
ALK-positive large B-cell lymphoma is a very rare subtype of DLBCL. It can affect people of any age and is more common in men. The lymphoma cells have a gene mutation that makes a protein on the surface of their B-Lymphocyte cells called ‘anaplastic large-cell kinase’ (ALK).
Most subtypes of DLBCL have a protein on the lymphoma cells called CD20. However, ALK positive large B-cell lymphomas do not usually have the CD20 protein. For this reason, treatment will be slightly different from other DLBCL subtypes. Although most of the medications will be the same, if you have this subtype, you will not receive a monoclonal antibody medicine called rituximab. Rituximab only works when CD20 is found on the lymphoma cells. So, if you’re wondering why you may not be getting the extra medicines other patients are getting….this may be the reason.
ALK-positive large B-cell lymphoma usually starts in your lymph nodes, so a common symptom you might experience is swollen lymph nodes.
However, it can also start in areas outside of your lymphatic system, including your:
- tongue
- nasopharynx (the area at the back of your nose and mouth)
- ovaries
- liver
- breasts
- bones
- stomach
- brain or epidural space (an area surrounding your spine)
Your symptoms will related to where the lymphoma is growing.
Intravascular large B-cell lymphoma is a rare form of an *extra-nodal DLBCL. It mostly affects older adults between 50-70 years of age. This subtype occurs equally in both men and women. The lymphoma cells are found within the inside lining of your small blood vessels. These small blood vessels are called capillaries.
Intravascular large B-cell lymphoma does not usually cause enlarged lymph nodes. It may affect small blood vessels in your skin or your brain. You may have central nervous system (CNS) symptoms. Your central nervous system includes your brain and spinal cord, so the symptoms you experience may include:
- confusion
- seizures
- dizziness
- weakness
Other symptoms you may experience specific to your subtype include:
- reddened patches or lumps on your skin
- an enlarged liver and/or spleen
These symptoms are in addition to the general lymphoma symptoms listed above.
Standard treatment for intravascular large B-cell lymphoma is the same as most other subtypes of diffuse large B-cell lymphoma (DLBCL), discussed later on this webpage.
*Extra-nodal means your lymphoma developed outside of your lymph nodes.
Primary Central Nervous System Lymphoma (PCNSL) is a rare subtype of DLBCL that is considered aggressive because it grows quickly. It is more common in people aged between 50 and 60 years of age, but can occur at any age.
If you have PCNSL your lymphoma likely started in your central nervous system, which includes your brain and spinal cord.
In more than 9 out 10 people that have PCNSL the lymphoma develops in the brain, spinal cord, eye or leptomeninges (the inner two membranes surrounding the brain and spinal cord).
The most common site is in the brain.
If your lymphoma has started in other parts of your body first then at some stage has spread to the brain or spinal cord, it is referred to as ‘secondary’ CNS lymphoma (SCNSL).
Treatment and management of PCNSL is different from other subtypes of DLBCL as the standard treatments cannot reach your brain and spinal cord. You can read more about the treatments for PCNSL later in the webpage under the heading Treatments.
Cutaneous (skin) B-cell lymphoma is a rare subtype of DLBCL that develops from the B-cells in your skin. Less than 1 out of 100 people with NHL will be diagnosed with this subtype.
For you doctor to diagnose you with this subtype, the lymphoma needs to be only affecting your skin.
Because this lymphoma starts in your skin, the main symptoms you may notice include are lumps, patches or a rash anywhere on your skin.
As cutaneous B-cell lymphomas are managed differently to other DLBCL subtypes, we have dedicated a different webpage to these subtypes.
You can find more specific information about cutaneous B-cell lymphoma here.
Please note that if you have been diagnosed with another subtype of DLBCL and it has spread to your skin, you should continue to look at the information on that first subtype. If the lymphoma has spread to your skin after starting somewhere else, it is considered secondary cutaneous lymphoma. Primary and secondary cutaneous lymphomas are managed differently.
Additionally, if you have cutaneous T-cell lymphoma, this is different again.
You can find more information on cutaneous T-cell lymphoma here.
Understanding your lymphoma genetics
Cytogenetic tests are done to check for genetic variances that may be involved in your disease. For more information on these please see our section on understanding your lymphoma genetics further down on this page. The tests used to check for any genetic mutations are called cytogenetic tests. These tests look to see if you have any changed in chromosomes and genes.
We usually have 23 pairs of chromosomes, and they are numbered according to their size. If you have DLBCL, your chromosomes may look a little different.
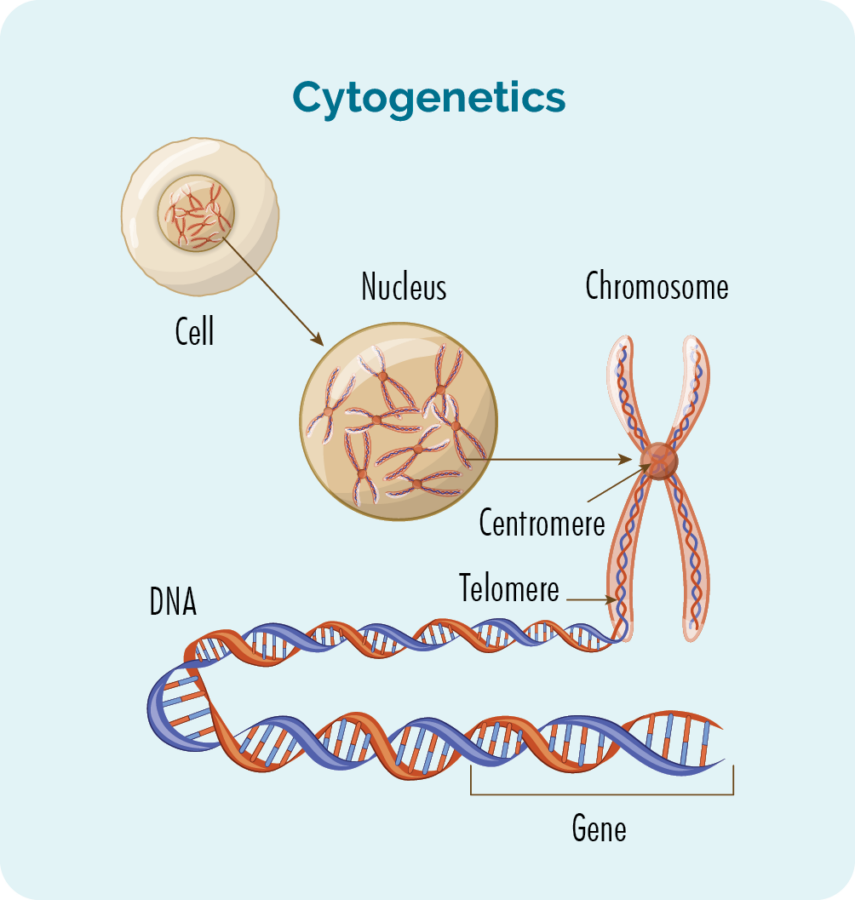
What are genes and chromosomes
Each cell that makes up our body has a nucleus, and inside the nucleus are the 23 pairs of chromosomes. Each chromosome is made from long strands of DNA (deoxyribonucleic acid) that contain our genes. Our genes provide the code needed to make all the cells and proteins in our body, and tells them how to look or act.
If there is a change (variation) in these chromosomes or genes, your proteins and cells will not work properly.
Lymphocytes can become lymphoma cells due to genetic changes (called mutations or variations) within the cells. Your lymphoma biopsy may be looked at by a specialist pathologist to see if you have any gene mutations.
Double Hit and Triple Hit mutations in DLBCL
Some people with DLBCL may have mutations in 2 or 3 specific genes which makes the lymphoma more aggressive than DLBCL without the mutations. These mutations are called rearrangements. The genes involved always involve a gene called MYC, and a gene called BCL2 and / or BCL6.
Double Expressor
In some cases, you may not have a rearrangement in your genes, but proteins the genes control may be over expressed on your lymphoma cells. This means you have too much of the MYC or BCL proteins on your cells, which may make it a little more difficult to treat.
Rearrangement and protein expression in Double & Triple Hit, and Double Expressor Lymphomas |
||||
MYC Rearrangement |
BCL2 Rearrangement |
BCL6 Rearrangement |
Overexpression of MYC and BCL proteins |
|
Double Hit |
YES |
YES |
No |
Usually, but not always |
Triple Hit |
YES |
YES |
YES |
Usually, but not always |
Double Expressor |
No |
No |
No |
YES |
Ask your doctor to explain you individual changes and how these may impact your treatment. |
||||
Normal MYC and BCL genes help make proteins needs for your cells to grow and develop properly. If you have a rearrangement in these genes, the protein is unable to support healthy cell growth and lymphoma can develop. DLBCL with these rearrangements are called either double hit lymphoma (DHL) or triple hit lymphoma (THL). They are also sometimes called high-grade B-cell lymphoma (HGBL).
Testing for mutations
If you have a high-grade lymphoma your doctor may wish to do further tests on your biopsies to see if you have any genetic rearrangements or double expressing proteins. The test is called Flourescence In Situ Hybridization (FISH) and looks at the different genetic markers on your biopsy samples.
However, this test is not covered by the Medicare benefits scheme so is often done at additional cost to patients, meaning you will have to pay for the tests. It can be quite expensive, and the cost can vary depending on where you get it done. Often, the treatment will not change, but in some cases it might. If the treatment would change if you had these variations, then you may consider getting the test done, or you may like to know just for interest sake.
If you choose not to have the test you will still have good care and treatment options.
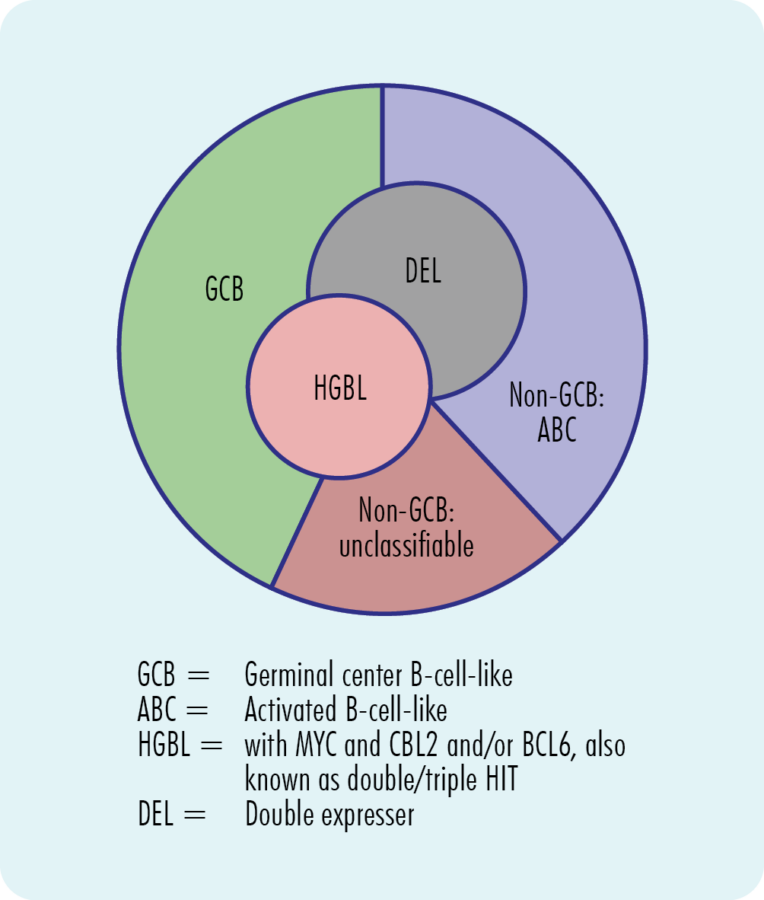
Other mutations found in DLBCL
Another genetic change that can occur in DLBCL is “double expressor”. This is different to double hit DLBCL because instead of having a rearrangement of genes, the genes are in the right place but are overexpressed, meaning there are too many of the two genes.
It is also important for your doctor to know what proteins (or receptors) are on your lymphoma cells. While chemotherapy works by killing fast growing cells, other medications work by targeting a specific protein on the lymphoma cell.
So if you have particular receptors, you may receive chemotherapy and one of the targeted monoclonal antibodies. For example:
- If you have protein called CD20 on your lymphoma cells, you may receive a monoclonal antibody medication that targets CD20, such as rituximab (Mabthera or Rituxan), obinutuzumab or ofatumumab. An additional medication that targets CD20, that is only available in clinical trials is mosunetuzumab.
- If you have a protein called CD79b on your lymphoma cells you may receive a medication that targets that protein, called polatuzumab vedotin.
As you can see, understanding some of the genetics of your lymphoma is important to understand your treatment options. Please always ask your doctor to explain your results to you and how these results impact your options.
Before you start treatment
Once all of your results from the biopsy, cytogenetic testing and the staging scans have been completed, the doctor will review these to decide the best possible treatment for you. At some cancer centres, the doctor will also meet with a team of specialists to discuss the best treatment option. This is called a multidisciplinary team (MDT) meeting.
Your doctor will consider many factors about your DLBCL. Decisions on when or if you need to start and what treatment is best are based on your:
- individual stage of lymphoma, genetic changes and symptoms
- age, past medical history and general health
- current physical and mental wellbeing and patient preferences.
More tests may be ordered before you start treatment to make sure your heart, lungs and kidneys are able to cope with the treatment. These may include an ECG (electrocardiogram), lung function test or 24-hour urine collection.
Your doctor or cancer nurse can explain your treatment plan and the possible side-effects to you, and are there to answer any question you might have. It is important you ask your doctor and/or cancer nurse questions about anything you don’t understand.
You can also phone or email the Lymphoma Australia Nurse Helpline with your questions and we can help you to get the right information.
Lymphoma care nurse hotline:
Phone: 1800 953 081
Email: nurse@lymphoma.org.au
Questions to ask your doctor before you start treatment for DLBCL
It can be difficult to know what questions to ask when you are starting treatment. If you don’t know, what you don’t know, how can you know what to ask?
Having the right information can help you feel more confident and know what to expect. It can also help you plan ahead for what you may need.
We put together a list of questions you may find helpful. Of course, everyone’s situation is unique, so these questions do not cover everything, but they do give a good start.
Click on the link below to download a printable PDF of questions for your doctor.
DLBCL treatment overview
There are different treatments available for Diffuse Large B cell lymphoma and they can differ depending on your specific subtype. The best treatment for you will depend on many factors including your:
- subtype of DLBCL
- stage and grade of your DLBCL
- age
- overall health
- other treatments you have, either for your DLBCL or other illnesses
- your own preference once your doctor has explained the options to you.
If you’ve had treatment for your lymphoma in the past, your doctor will consider how well it worked for you, and how bad any side-effects were for you. Your doctor will then be able to offer the best treatment options for you. If you’re not sure why the doctor has made the decisions they’ve made, please make sure to ask them to explain it to you – they are there to help you.
Treatment cycles
Treatment for DLBCL is given in cycles. This means, instead of getting all the treatment at once, you will have some treatment, then a break (usually 2 or 3 weeks) and then more treatment.
Treatment is given like this to keep you safe. If we gave you all the chemo in one go, to destroy all the lymphoma – it would be very dangerous for you because chemo also attacks healthy cells.
So, it is given in cycles so that it can destroy a lot of the lymphoma, and then you have a few weeks for your healthy cells to recover or replace themselves. The number of cycles you have will depend on what treatment you have, and how well you respond to it.
Healthy cells at much better at recovering than the lymphoma cells, so each time you have treatment you will have less and less lymphoma in your body.
Lines of treatment
Sometimes lymphoma doesn’t respond to the first type of treatment you have. When this happens, the lymphoma may stay the same, or get worse even with the treatment. When this happens, the lymphoma is called refractory.
In some cases, DLBCL responds very well to treatment, and you may go into remission. This means that there are no signs of lymphoma left in your body. However, after some time – it could months or even a few years later it may come back. When this happens it is called a relapse.
The first time you have a treatment for DLBCL it is called first-line treatment. First line treatment usually involves around 6 cycles of treatment. But the final number of cycles will depend on the treatment protocol and how well you respond.
If your lymphoma is refractory or relapses, the next time you have treatment it is called second-line treatment. Many people can still be cured or achieve long-term remission after second-line treatment. If it happens again, it is called third-line treatment.
Many people will actually be cured after first-line treatment. But some may need second, third line treatment or more.
Types of treatment
Some of the different types of treatments you may be offered are listed below. Click on the headings to learn more about the treatment type you are interested in.
Chemo is the most common treatment for DLBCL, and is often give along with a monoclonal antibody – a type of immunotherapy. When you do have both types of treatments together it is called chemoimmunotherapy.
Chemo kills fast growing cells which makes it very effective at fighting DLBCL. But, it can also affect some of your good cells that grow fast causing side effects.
Immunotherapy is a broad term to describe medicines that help your own immune system find, and fight the lymphoma more effectively.
Types of immunotherapy that may used to fight DLBCL include:
- Monoclonal antibodies
- Bispecific Antibodies
- Conjugated Antibodies
- CAR T-cell Therapy
When immunotherapy is given with chemotherapy, it is called chemoimmunotherapy.
Treatment protocol that includes chemotherapy and immunotherapy. For example:
R-CHOP includes the MAB rituximab (immunotherapy) which is given along with 3 chemotherapy medicines.
You may have a MAB infusion at a cancer clinic or hospital. MABs attach to the lymphoma cell and attract other diseases fighting white blood cells and proteins to the cancer so your own immune system can fight the DLBCL.
MABS will only work if you have specific proteins or markers on your lymphoma cells. A common marker in DLBCL is CD20. If you have this marker you may benefit from treatment with a MAB called rituximab or obinutuzumab.
Bispecific antibodies are a type of immunotherapy, and subclass of monoclonal antibodies.
To make them, scientists join two different antibody parts into one molecule. One-part of the antibody attaches to the lymphoma cell, and the other part attaches to a T-cell – a strong disease fighting immune cell. By doing this, the Bispecific Antibody brings the T-cells straight to the lymphoma cell so it can destroy the lymphoma.
Examples of Bispecific Antibodies include epcoritamab, blinatumomab and glofitamab.
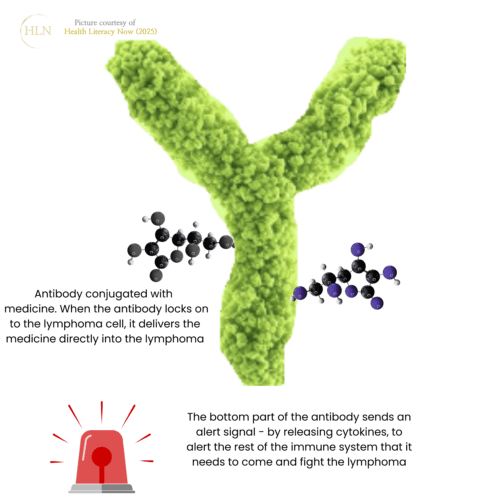
Antibody Conjugates are a subclass of monoclonal antibodies.
They are antibodies joined in a lab to another medicine such as a toxin, chemotherapy, or a radioactive particle. The antibody acts like a taxi, driving the attached medicine past your healthy cells and straight to the lymphoma cell. The antibody attaches to the antigen on the lymphoma cell (e.g. CD20 or CD19) and then releases the toxin whcih destroys the lymphoma cell.
The antibody also sets of an alert, by releasing chemicals called cytokines that attract other immune cells to come and fight the lymphoma.
This helps deliver the lymphoma fighting medicine straight to the lymphoma while protecting healthy cells.
Examples of Antibody conjugates includes brentuximab vedotin and polatuzumab vedotin.
Immunomodulators are medicines taken as a tablet. We don’t know exactly how they work, but we think they have several effects against lymphoma. These include:
- directly destroying lymphoma cells
- helping your immune system work more efficiently
- stopping the lymphoma tumor from developing blood vessels. This stops it from getting the oxygen and nutrients it needs to grow
- changing the cytokines (small chemical messengers) that the lymphoma sends to help it grow
- preventing lymphoma growing in your bone marrow.
CAR T-cell therapy is a newer treatment that will only be offered if you have already had at least one other treatment for your DLBCL.
In some cases, you may be able to access CAR T-cell therapy by joining a clinical trial.
CAR T-cell therapy involves an initial procedure similar to a stem cell transplant, where your T-cell lymphocytes are removed from you blood during an apheresis procedure. Like you B-cell lymphocytes, T-cells are part of your immune system and work with your B-cells to protect you from disease and illness.
When the T-cells are removed, they are sent to a laboratory where they are re-engineered. This happens by joining the T-cell to an antigen that helps it recognise the lymphoma more clearly and fight it more effectively.
Chimeric means having parts with different origins so the joining of an antigen to the T-cell makes it chimeric.
Once the T-cells have been re-engineered they will be returned to you to start fighting the lymphoma.
For more information on CAR T-cell therapy please click here.
A stem cell or bone marrow transplant is done to replace your diseased bone marrow with new stem cells that can grow into new healthy blood cells. Bone marrow transplants are usually only done for children with DLBCL, while stem cell transplants are done for both children adults.
In a bone marrow transplant, stem cells are removed straight from the bone marrow, where as with a stem cell transplant, the stem cells are removed from the blood.
The stem cells may be removed from a donor or collected from you after you’ve had chemotherapy.
If you the stem cells come from a donor, it is called an allogeneic stem cell transplant.
If your own stem cells are collected, it is called an autologous stem cell transplant.
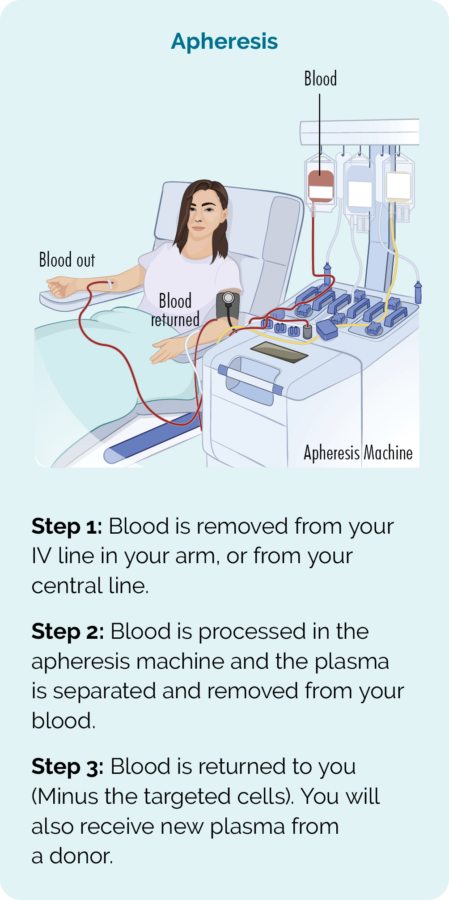
Stem cells are collected through a procedure called apheresis. You (or your donor) will be connected up to an apheresis machine and your blood will be removed, the stem cells separated and collected into a bag, and then the rest of your blood is returned to you.
Before the procedure, you will get high-dose chemotherapy or full-body radiotherapy to kill off all your lymphoma cells. However this high dose treatment will also kill off all the cells in your bone marrow. So the collected stem cells will then be returned to you (transplanted). This happens in much the same was as blood transfusion is given, through a drip into your vein.
For more information on Stem Cell transplants, please click here.
Supportive care can help patients have fewer side-effects, and recover more quickly from the effects of lymphoma treatment. It can also help manage symptoms of the lymphoma.
Supportive care may include:
- Blood or platelet transfusion to replace cells lost from the lymphoma or its treatment
- Growth factors (like filgrastim or pegfilgrastim) which stimulates the bone marrow to create more white blood cells to prevent infection
- Antinausea medication to help stop you feeling sick
- Anti-infective agents such as antibiotics, antivirals or antifungals to treat or prevent infection
- Pain management
- Social worker to help with all the planning and organisation needed during lymphoma and treatment
- Psychologist or counsellor to help manage the emotional changes from a lymphoma diagnosis or mood changes related to treatment effects
- Other support as needed.
Let your treating team know what extra support you may need. The earlier you let them know, the sooner they can help.
Supportive care can also include palliative care which helps to improve your symptoms and side-effects, as well as end of life care if needed
It is important to know that the Palliative Care team can be called on at any time during your treatment pathway not just at the end of life. They can help control and manage symptoms (like hard to control pain and nausea) you might be experiencing as a result of your disease or its treatment.
If you and your doctor decide to use supportive care or stop curative treatment for your lymphoma, many things can be done to help you to stay as healthy and comfortable as possible for some time.
Radiation therapy is not a standard treatment in DLBCL as it is best used for small areas of cancer that are only in 1 or 2 parts of your body. Because of the fast- growing nature of DLBCL it is often larger or in many areas of your body when you are first diagnosed.
In some cases though, it may be useful if there is one small area that has not responded to other treatments, or if the lymphoma is pressing on a vital organ like your airway or spinal cord and you can’t start chemo right away.
It is a targeted treatment that uses high doses of radiation to kill lymphoma cells and shrink tumours. Before having radiation, you will have a planning session. This session is important for the radiation therapists to plan how to target the radiation to the lymphoma, and avoid damaging healthy cells. Radiation therapy usually lasts between 2-4 weeks. During this time, you will need to go to the radiation centre everyday (Monday-Friday) for treatment.
*If you live a long way from the radiation centre and need help with a place to stay during treatment, please talk to your doctor or nurse about what help is available to you. You can also contact the Cancer Council or Leukemia Foundation in your state and see if they can help with somewhere to stay.
Starting treatment
Starting Treatment
You will need to start treatment soon after all your test results come back. In some cases, you may start before all of the results are in.
It can be quite overwhelming when you start treatment. You may have many thoughts about how you will cope, how to manage at home, or how sick you might get.
Let your treating team know if you’d like extra support. They can refer you to a social worker or other supportive service to make sure you get the help you need.
You can also reach out to the Lymphoma care nurses by clicking on the “Contact us” button at the bottom of this page.
First-line treatment protocols
Treatment for first-line DLBCL is pretty standard. Meaning there are set protocols that have been tested and prove to me effective for most people with DLBCL.
The first time you have treatment you will likely be offered one of the below treatment protocols.
Click on the headings to learn more about each protocol or skip straight to the one you know you will be having.
R-CHOP, R-mini-CHOP or SMARTE-R-CHOP
R-CHOP is the most common first-line treatment protocol for people with DLBCL. It includes:
- Rituximab – a monoclonal antibody – attaches to the CD20 marker on the lymphoma cell
- Doxorubicin – a chemotherapy
- Vincristine – a chemotherapy
- Cyclophosphamide – a chemotherapy.
As well as these, you will have medicine to take at home including a corticosteroid called Prednisolone, which are tablets that you take for 5 days. You will also have anti-nausea tablets to stop you feeling sick.
Four days after the chemo, you will need to have a small injection (called pegfilgrastim) under the skin – usually in your tummy. This is to help your white blood cells recover more quickly. This helps to stop you getting an infection.
You will usually have 6 cycles of R-CHOP but may have anywhere between 4 and 8 cycles. Each cycle will either be 14 or 21 days long. You will have the rituximab and chemo on day 1 of each cycle.
R-mini-CHOP and SMARTE-R-CHOP
These 2 treatments use all the same medicines as in R-CHOP, but the doses and timing of the medicine may be different. These are given to older people (over 60years old) or people who are unwell and may not be able to tolerate the full dose of R-CHOP.
DA-R-EPOCH
You may be offered DA-R-EPOCH if you have a high grade DLBCL with genetic variations in the MYC and BCL-2 or BCL-6 genes.
The DA stands for Dose Adjusted. This means your haematologist will change the dose of your chemotherapy each cycle depending on your side-effects.
DA-R-EPOCH includes:
- Rituximab – a monoclonal antibody – attaches to the CD20 marker on the lymphoma cell
- Doxorubicin – a chemo
- Vincristine – a chemo
- Etoposide – a chemo
- Cyclophosphamide- a chemo.
On day 6, you will start having a small injection called Filgrastim under the skin (usually in your tummy). Filgrastim helps your white cells recover to help prevent infections. You will have this injection every day until your white cells recover.
R-CHOEP
This protocol uses all the same medicines as in DA-R-EPOCH but with regular doses each cycle.
It may be offered to people less than 60 years of age who have stage 3 or 4 DLBCL when first diagnosed.
Each cycle is 14 days (2 weeks), and you will have all the chemo on the first 3 days.
Pola-R-CHP
Pola-R-CHP is a newer treatment protocol that uses similar medicines to other protocols, but also includes a Conjugated Antibody called Polatuzumab Vedotin (Polivy®).
- Rituximab – a monoclonal antibody – attaches to the CD20 marker on the lymphoma cell
- Polatuzumab Vedotin – a Conjugated Antibody
- Doxorubicin – a chemo
- Cyclophosphamide – a chemo
You will likely have 6 cycles including all these medicines and then another 2 cycles with just the rituximab.
As well as the above, you will have medicine to take at home including a corticosteroid called Prednisolone. You will take these for 5 days. You will also have anti-nausea tablets to stop you feeling sick.
Each cycle, on the day after chemo, you will have a small needle in under the skin, usually in your tummy. This medicine is called Filgrastim and helps your white cells recover quickly to avoid infection. You will have this each day until your white cells recover.
Your nurses may teach you, or a trusted friend/family member to give yourself these injections.
♦ Polatuzumab Vedotin is not yet listed on the Pharmaceutical Benefit Scheme (PBS), so you may need to pay for this part of the protocol. Ask your doctor if there are any access schemes that may help lower the cost for you.
Clinical Trial
Clinical trials are how researchers test new treatments, or new combinations of treatments to see if they ork better than current treatments.
They may also test if having certain treatments earlier might result in better outcomes.
Talk to your doctor about clinical trials. They can let you know if there are any you are eligible for.
For more information on clinical trials please click here.
Second-line treatment protocols
You may be offered any of the above treatments listed under first-line treatment, or one of the below second-line treatments after a relapse, or if your lymphoma has been refractory to the first-line treatment.
Before deciding on the best options for you, your doctor will consider:
- Your personal situation and goals for treatment
- Any changes to your lymphoma cells during previous treatments, such as new genetic changes
- How the lymphoma has responded to pother treatments
- How long you’ve been remission.
Bendamstine, Polatuzumab Vedotin and Rituximab
This treatment protocol may be offered to you if you are:
- unable to have a stem-cell transplant
- waiting to have CAR T-cell therapy.
It includes:
- Rituximab – a Monoclonal Antibody
- Polatuzumab vedotin – an Antibody Conjugate
- Bendamustine – a chemo.
It is given every 21 days (3 weeks), and you will have all these medicine on the first 2 or 3 days of each cycle. You may have up to 6 cycles.
♦ Polatuzumab Vedotin is not yet listed on the Pharmaceutical Benefit Scheme (PBS), so you may need to pay for this part of the protocol. Ask your doctor if there are any access schemes that may help lower the cost
DHAC +/- Rituximab
DHAC may be given with or without rituximab. Your doctor will do tests before you start treatment to see if the lymphoma cells still have the CD20 antigen on them.
Sometimes, after treatment with rituximab in the first-line treatment, lymphoma cells can stop the CD20 from showing.
You will only have rituximab as part of this treatment if the lymphoma still has the CD20 antigen.
DHAC includes 2 types of chemotherapy including cytarabine and carboplatin. You will also have a type of corticosteroid called dexamethasone for 4 days.
This treatment is given every 21 days (3 weeks), and you will have the chemo on the first 2 days of each cycle. You may have 2-6 cycles.
Gemcitabine & Vinorelbine
This protocol includes the 2 chemo’s gemcitabine and vinorelbine. It is given every 21 days (3 weeks) and you will have chemo on the first, and 8th day of each cycle.
On the 9th day you will have Pegfilgrastim, a small injection under the skin (usually in your tummy), to help your white cells recover and help prevent infection.
You may have between 4 and 6 cycles.
R-DHAOx
R-DHAOx is given every 21 days (3 weeks) and you will have treatment on days 1-3 of each cycle. This protocol includes:
- Rituximab – a CD20 targeting monoclonal antibody
- Oxaliplatin – a chemo
- Cytarabine – a chemo.
In addition to these, you will also have another medicine (a corticosteroid) called dexamethasone for 4 days, starting the 1st day of the cycle before you start chemo. You may also be given anti-nausea tablets to take home to stop you feeling sick.
You may have up to 6 cycles of this treatment protocol, or as little as 1 or 2 cycles. Your doctor will assess you regularly to see how the treatment is working, and what side-effects before deciding if you need another cycle.
♦ When having treatment with Oxaliplatin it is important not to touch or eat anything that is cold. It can give you pain, or make it feel like you can’t breathe well. These symptoms are temporary, but unpleasant.
If you are taking something out of the fridge or freezer, use oven mitts.
R-GemOx
You may be offered this treatment if you’re unable to have stem cell transplant, or if you have relapsed after a stem cell transplant.
It includes 8 cycles that is 14 days long (2 weeks). You will have all the treatment on the first day of the cycle. Treatment includes:
- Rituximab – a CD20 targeting monoclonal antibody
- Gemcitabine – a chemo
- Oxaliplatin – a chemo
♦ When having treatment with Oxaliplatin it is important not to touch or eat anything that is cold. It can give you pain, or make it feel like you can’t breathe well. These symptoms are temporary, but unpleasant.
If you are taking something out of the fridge or freezer, use oven mitts.
ICE or R-ICE
ICE includes 3 chemo’s including Etoposide, carboplatin, and ifosphamide. Ifosphamide can cause some inflammation and bleeding in your bladder, so you will also have a medicine called Mesna that protects your bladder, and extra fluids through a cannula or central line, into your veins (IV Fluids) to help flush the chemo out.
In addition to the above, if your lymphoma cells still have the CD20 marker on them, you may have rituximab too (R-ICE).
You may have up to 6 cycles.
ESHAP
ESHAP includes 3 chemo’s – cisplatin, etoposide and cytarabine and a high-dose steroid called Methylprednisolone. You will have the steroids and chemo over the first 5 days of your cycle.
Then, on the 6th day you will have a small injection (called pegfilgrastim) under the skin – usually in your tummy. This is to help your white blood cells recover more quickly. This helps to stop you getting an infection.
Depending on your situation, you may have between 3 and 6 cycles which will 3 or 4 weeks long.
DHAP or R-DHAP
DHAP includes a corticosteroid called dexamethasone, and 2 chemo’s called cytarabine and cisplatin. You may also have a MAB (rituximab) if the lymphoma cells still have the CD20 marker on them. If you have the MAB, the protocol is called R-DHAP.
You may have between 2 and 6 cycles. Each cycle is 21 days (3 week) long and you will have the chemo and MAB on the first 2 days of the cycle. You will have the dexamethasone for the first 4 days of each cycle.
GDP or R-GDP
GDP includes 2 chemos gemcitabine and cisplatin, and a corticosteroid called dexamethasone. If the lymphoma cells still have e CD20 marker on them you will also have rituximab (R-GDP)
Each cycle is 21 days long and you will have the dexamethasone for the first 4 days of each cycle. You will have both chemo’s on the first day of the cycle and then only the gemcitabine on day 8. If you have rituximab, you will have this on day 1 of each cycle.
You may have up to 6 cycles.
Tafasitamab & Lenolidamide
You may be offered this treatment if you are unable to have a stem cell transplant and your lymphoma has maker called CD19 on it. It includes:
- Tafasitimab – a monoclonal antibody that targets the CD19 marker
- Lenolidamide – an immunomodulatory tablet.
There is no set number of cycles for this protocol. You can continue on this treatment for as long as it is effective, and your side-effects are well managed.
Each cycle is 4 weeks (28 days) and the first few cycles are more intensive.
For the 1st cycle you will have:
- Lenolidamide tablets at home for 21 days
- Tafasitamab at the clinic or hospital on days 1, 4, 8, 15 and 22.
Cycle 2 and 3 you will have:
- Lenolidamide tablets at home for 21 days
- Tafasitamab at the clinic or hospital on days 1, 8, 15, 22.
Cycles 4-12 you will have:
- Lenolidamide tablets at home for 21 days
- Tafasitamab at the clinic or hospital on days 1 and 15.
Any further cycles you will have:
- Tafasitamab only on days 1 and 15.
CAR T-cell Therapy
CAR T-cell therapy is a type of immunotherapy. The name stands for:
- CAR stands for Chimeric Antigen Receptor. A CAR is a special, man-made protein designed to recognise and stick to another receptor called CD19 on your lymphoma cells.
- T-cells are a type of white blood cell in our body that help fight infections and cancer.
It is a complex treatment that happens in stages. including:
- Checking your eligibility
- Collection T-cells from your blood in a procedure called apheresis
- Sending the T-cells to a lab where they have the CAR attached to them
- Getting ready to have the CAR T-cells
- The infusion of CAR T-cells
- Staying in or close to the hospital for up to 2 months
For more information on CAR T-cell therapy please click here.
Stem-cell Transplant
Stem-cell transplants are a “rescue” treatment rather than a treatment for DLBCL.
What does that mean you ask?
It means that they are given to rescue or help your bone marrow recover after very high dose chemotherapy. The chemotherapy is the treatment, and the stem-cells help you recover by making new healthy cells.
Usually, we give smaller doses of chemo to make sure you still have enough healthy cells to live, while still destroying the lymphoma over each cycle.
Sometimes, having a higher dose of chemo may give you a better a chance for a cure, or give you a longer-lasting remission. In these cases, your doctor may offer a stem cell transplant.
For more information on stem-cell transplants please click here.
Third & Later line treatment protocols
If you have a second relapse, or don’t respond to 2 other treatments, you may be offered any of the above listed treatment protocols, or one of the below treatments.
Before deciding on the best options for you, your doctor will consider:
- Your personal situation and goals for treatment
- Any changes to your lymphoma cells during previous treatments, such as new genetic changes
- How the lymphoma has responded to pother treatments
- How long you’ve been remission.
Epcoritamab
Epcoritamab is a bispecific antibody that is given as in injection under the skin – usually in your tummy.
To avoid serious side-effects, on cycle 1 you will start with a lower dose and gradually increase to the regular dose by the end of cycle 1.
There is no set number of cycles, and you can continue to have epcoritamab unless it stops working, or your side-effects become too difficult to manage.
Each cycle is 28 days (4 weeks long).
- Cycles 1-3 You will have the epcoritamab on days 1, 8,15, and 22
- Cycles 4-9 You will have the epcoritamab on days 1 and 15
- Cycle 10 and more You will have epcoritamab on day 1.
Glofitamab & Obinutuzumab
Glofitamab is a bispecific antibody and obinutuzumab is MAB.
You will have up to 12 cycles every 21 days (3 weeks), and you will only have the obinutuzumab in the 1st cycle.
- Cycle 1 – Obinutuzumab day 1, Glofitamab days 8 and 15
- Cycles 2-12 – Glofitamab only on day 1.
Clinical trials
Many clinical trials are looking at how to improve treatment for people need third, or later line treatments.
We recommend you talk to your doctor about clinical trials, and if there are any you may be eligible for.
For more information on clinical trials please click here.
Clinical trials & Alternative access to treatments
It is recommended that anytime you need to start new treatments you ask your doctor about clinical trials you may be eligible for.
Clinical trials are important to find new medicines, or combinations of medicines to improve treatment of DLBCL in the future.
They can also offer you a chance to try a new medicine, combination of medicines or other treatments that you would not be able to get outside of the trial. If you are interested in participating in a clinical trial, ask your doctor what clinical trials you are eligible for.
There are many treatments and new treatment combinations that are currently being tested in clinical trials around the world for patients with both newly diagnosed and relapsed DLBCL.
For more information on clinical trials, wach the video.
For medicine to be routinely available in Australia it needs to be registered with the Therapeutics Goods Administration (TGA). For it to be public funded, making them more affordable, they need to listed on the Pharmaceutical Benefits Scheme (PBS)
These processes can take years, and not all medicines registered with the TGA will be listed on the PBS. This means, that even when they are available, some treatments may be a lot more expensive than others.
However, there are some options that may help you access some of these medicines if your haematologist believes they offer a better chance at cure, remission, or disease management. Watch the video to see how options work.
Prognosis for DLBCL – and what happens when treatment ends
Prognosis is the term used to describe the likely path of your disease, how it will respond to treatment and how you will do during and after treatment.
There are many factors that contribute to your prognosis and it is not possible to give an overall statement about prognosis. However, DLBCL often responds very well to treatment and many patients with this cancer can be cured – meaning after treatment, there is no sign of DLBCL in your body.
Factors that can impact prognosis
Some factors that may impact your prognosis include:
- You age and overall health at time of diagnosis.
- How you respond to treatment.
- What if any genetic mutations you have.
- The subtype of DLBCL you have.
If you would like to know more about your own prognosis, please talk with your specialist haematologist or oncologist. They will be able to explain your risk factors and prognosis to you.
Survivorship - Living with, and after cancer
A healthy lifestyle, or some positive lifestyle changes after treatment can be a great help to your recovery. There are many things you can do to help you live well with DLBCL.
Many people find that after a cancer diagnosis, or treatment, that their goals and priorities in life change. Getting to know what your ‘new normal’ is can take time and be frustrating. Expectations of your family and friends may be different to yours. You may feel isolated, fatigued or any number of different emotions that can change each day.
The main goals after treatment for your DLBCL is to get back to life and:
- be as active as possible in your work, family, and other life roles
- lessen the side effects and symptoms of the cancer and its treatment
- identify and manage any late side effects
- help keep you as independent as possible
- improve your quality of life and maintain good mental health
Different types of cancer rehabilitation may be recommended to you. This could mean any of a wide range of services such as:
- physical therapy, pain management
- nutritional and exercise planning
- emotional, career and financial counselling.