Overview of Anaplastic Large Cell Lymphoma (ALCL)
Anaplastic Large Cell Lymphoma (ALCL) is a rare and aggressive (fast-growing) subtype of PTCL. ALCL develops from white blood cells called T-lymphocytes (T-cells) which are part of our immune system, keeping us healthy by fighting infection and disease, and regulating our immune responses.
The subtypes of ALCL are:
- Systemic ALCL – ALK +ve
- Systemic ALCL – ALK -ve
- Breast implant associated (BIA)ALCL
- Primary cutaneous (Pc)ALCL
Why is it called Anaplastic Large Cell Lymphoma?
- Anaplastic means the cells look very different from regular healthy T-cells.
- Large cell means they have grown larger than healthy T-cells.
- Lymphoma means cancer of white blood cells call lymphocytes.
In ALCL your T-cell lymphocytes become cancerous, causing them to grow much larger, and very differently from your healthy T-cells. This happens because cancerous cells are very disorganised and no longer develop in the way they are designed to grow. As a result, the cancerous lymphoma T-cells can no longer work effectively to protect you from infection and disease, or regulate your immune responses.
There is also a protein found on the surface of the ALCL cell that is called ‘CD30’, which helps differentiate ALCL from other subtypes of PTCL. It is important to know if your cells are CD30 positive, because a certain medication (Brentuximab vedotin) that can be used to treat some lymphomas will only work if your lymphoma cells have this CD30 protein on them.
What causes Anaplastic Large Cell Lymphoma (ALCL)?
As with many types of lymphoma, we don’t know what causes ALCL to develop in most people. One subtype – BIA-ALCL only occurs in people with breast implants and is more common in those with textured silicone implants. However, it is still rare among those with implants, so while the implants increase risk, they do not cause ALCL.
Patient stories living with, or after ALCL
Understanding T-cell Lymphocytes
Understanding T-cell Lymphocytes
To understand ALCL, you need to know about your T-cell lymphocytes.
T-cell lymphocytes are an important part of our immune system that protect us against infection and disease, and regulate our immune system to prevent autoimmune attacks. Auto immune attacks happen when our immune system is overactive or faulty and begins to fight our own body instead of infection and disease.
T-cells are made in our bone marrow, but before they mature, they travel through our lymphatic system to our thymus where they continue to grow and mature.
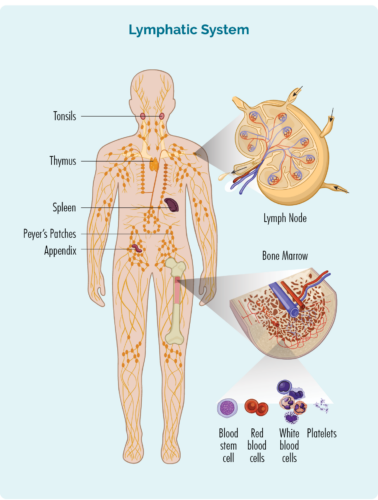
About T-cell Lymphocytes
- T-cells are made in our bone marrow, mature in our thymus, but can live in any part of our lymphatic system – including our lymph nodes.
- T-cells need to be activated to work effectively. They are usually resting in our thymus, lymph nodes or other parts of your lymphatic system, and only wake up and fight infection when other immune cells let them know there is an infection or disease to fight. When they wake up, T-cells can travel to any part of our body to fight the infection or disease.
- Some T-cells are responsible for “regulating” the immune response. This means that once and infection has been destroyed, the “Regulatory T-cells” tell other immune cells to “stand down” so they don’t keep fighting and cause harm to our good cells once the infection is gone.
- After fighting an infection or disease, some T-cells become “Memory T-cells” and they remember everything there is to know about the infection and how to fight it. That way, if we ever get the same infection or disease again, our immune system can fight it a lot more quickly and effectively.
- Some T-cells help other immune cells, such as B-cell lymphocytes to work effectively. These T-cells are called “Helper T-cells”.
Symptoms of ALCL
The symptoms of ALCL vary depending on the subtype of ALCL you have, as well as what parts of your body have lymphoma in them. The symptoms you get, may be very different from someone else with ALCL.
There are some symptoms of lymphoma that are common among many people with lymphoma regardless of subtype though. These more common symptoms are outlined below.
General symptoms of lymphoma
Some symptoms are common in all types of lymphoma so you may also get any of the following symptoms:
Swollen lymph nodes that look or feel like a lump under your skin. These are most often found in your neck, armpits or groin, because these lymph nodes are closer to your skin than other lymph nodes. However, any lymph node can be affected, but might only be found during CT or other scan.
Fatigue – extreme tiredness not improved by rest or sleep.
Loss of appetite – not wanting to eat.
Itchy skin.
Shortness of breath.
Pain in your stomach or abdomen.
Bleeding or bruising more than usual.
B-symptoms.
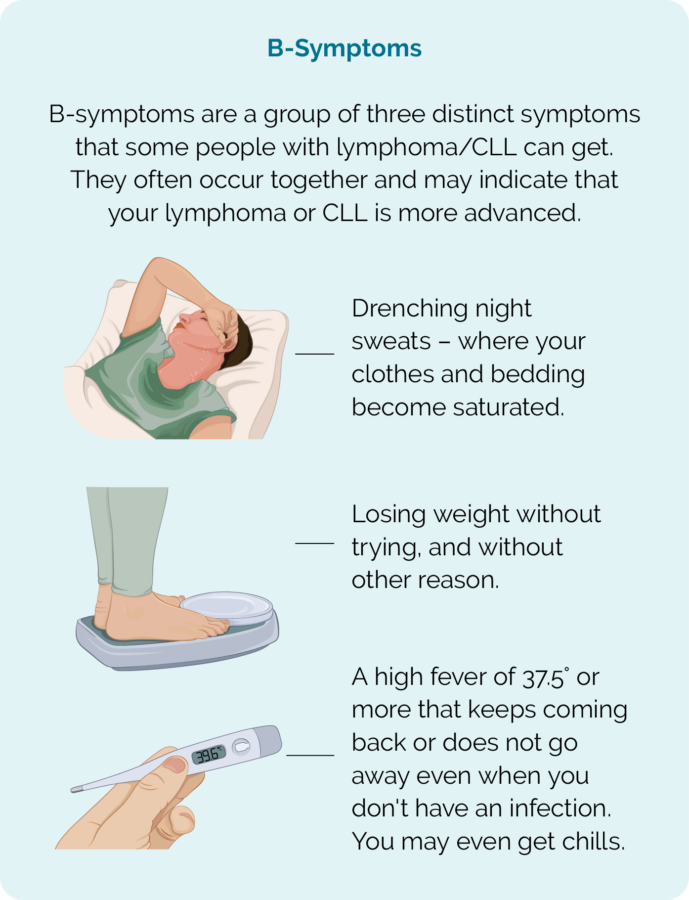
Symptoms specific to your subtype of ALCL are covered below in the section overview of ALCL subtypes.
How is Anaplastic Large Cell Lymphoma diagnosed?
If your doctor thinks that you may have lymphoma, they will need to organise a number of important tests. These tests are needed to either confirm or rule out lymphoma as the cause for your symptoms.
Blood tests
Blood tests are taken when trying to diagnose your lymphoma, but also throughout your treatment to make sure your organs are working properly, and can cope with treatment.
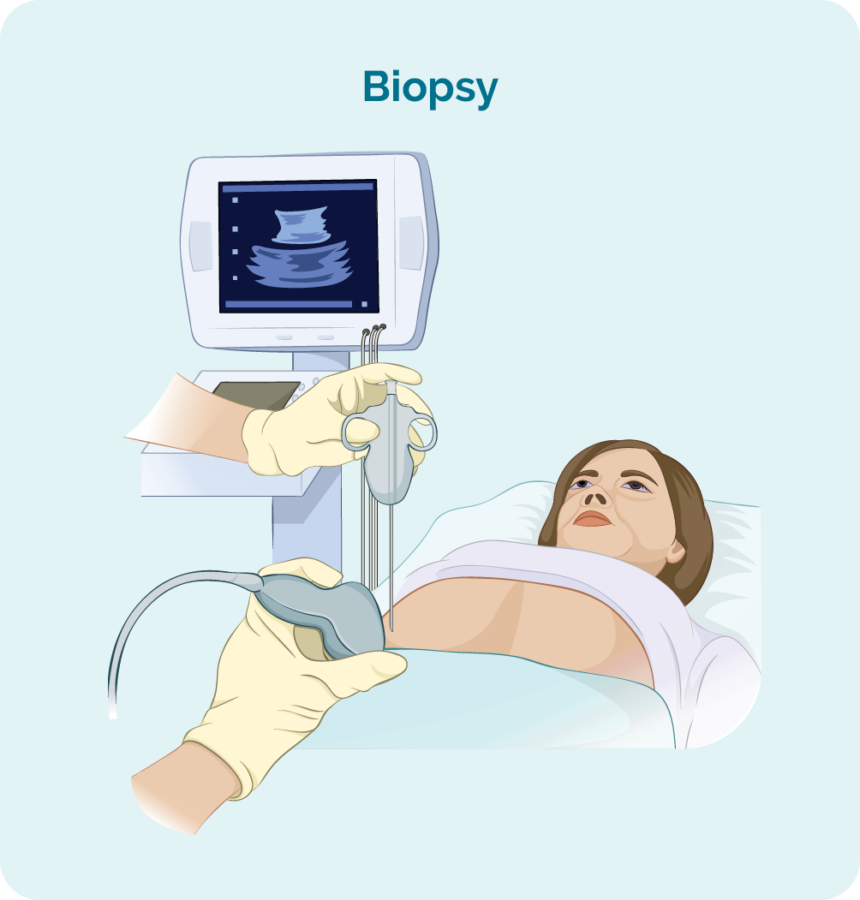
Biopsies
To diagnose ALCL you will need a biopsy. A biopsy is a procedure to remove part, or all of an affected lymph node and/ or a bone marrow sample. The biopsy is then checked by scientists in a laboratory to see if there are changes that help the doctor diagnose ALCL.
When you have a biopsy, you may have a local or general anaesthetic. This will depend on the type of biopsy and what part of your body it is taken from. There are different types of biopsies, and you may need more than one to get the best sample.
Core or fine needle biopsy
Core or fine needle biopsies are taken to remove a sample of swollen lymph node or tumour to check for signs of GZL.
Your doctor will usually use a local anaesthetic to numb the area so you don’t feel any pain during the procedure, but you will be awake during this biopsy. They will then put a needle into the swollen lymph node or lump and remove a sample of tissue.
If your swollen lymph node or lump is deep inside your body the biopsy may be done with the help of ultrasound or specialised x-ray (imaging) guidance.
You might have a general anaesthetic for this (which puts you to sleep for a little while). You may also have a few stitches afterwards.
Core needle biopsies take a bigger sample than a fine needle biopsy, so are a better option when trying to diagnose lymphoma.
Overview of ALCL subtypes
From your biopsies, and by examining where in your body the lymphoma has started, your doctor will be able determine which subtype of ALCL you have. The subtype is important to know, because it provides information on what type of treatments may work best for you. If you don’t already know, ask your doctor what subtype of ALCL you have, and how this impacts your treatment.
Primary cutaneous ALCL is an indolent (slow-growing) lymphoma that starts in the T-cells in the layers of your skin. Unlike other subtypes of ALCL, you may not need any treatment for PcALCL. Like most types of indolent lymphoma, you may live with PcALCL for the rest of your life, but it is important to know, that you can live well with it, and it may not have any negative effect on your health. It usually only affects your skin and very rarely spreads past your skin to other parts of your body.
It usually starts with a rash or lumps on your skin that may be itchy or painful, but may also not cause you any discomfort. Sometimes, it may be more like a sore that doesn’t heal as you would expect it to. Any treatment of PcALCL is likely to be to improve any itching or pain, or to improve the look of the lymphoma rather than to treat the lymphoma itself. However, if the PcALCL only affects a very small area of skin, it may be removed with surgery or through radiotherapy.
PcALCL is more common in people aged between 50-60 years, but can affect anyone of any age, including children.
ALK +ve ALCL is the most common subtype of ALCL. It is aggressive (fast-growing) lymphoma that can start and spread to any part of your body, which is why it is called systemic. In ALK-positive ALCL, the abnormal T-cells have a genetic change (mutation) that causes them to make a protein called ‘anaplastic lymphoma kinase’ (ALK). Because they produce this protein, it is called ALK positive.
ALK +ve ALCL is more common in children and young adults less than 40 years old, although it can affect anyone of any age. It affects males three times more commonly than females.
If you have ALK +ve ALCL you may get any of the symptoms listed above. Other symptoms may relate to where your lymphoma is. For example, if the ALCL is in your gut, you may get tummy pains or changes to how your bowels work, or blood in your stool (poo).
ALK -ve ALCL affects about 3 out of every 10 people with ALCL. It is called ALK -ve because unlike ALK +ve ALCL, the lymphoma cells do not produce the protein ‘anaplastic lymphoma kinase’ (ALK). However, like ALK +ve ALCL, it is an aggressive (fast-growing) subtype that can start and spread to any part of your body, which is why it is called systemic.
ALK -ve ALCL is more common in middle-aged adults around 40-65 years of age, but can affect people of any age.
If you have ALK -ve ALCL you may get any of the symptoms listed above. Other symptoms may relate to where your lymphoma is.
Breast Implant Associated ALCL is so named because it only affects people with breast implants. It has only been identified in the last few years, so more is still being learned about it, but seems to be more common if you have textured silicone implants. It starts in the breast with the implant and is usually slow-growing (indolent) and is often only found in the breast. However, it can rarely act more aggressively and spread outside the breast.
Despite starting in the breast with the implant, BIA-ALCL is NOT a type of breast cancer, it is a lymphoma that begins when T-cell lymphocytes in the breast (not breast cells) become cancerous. It is thought that it develops as a result of long-term inflammation around the breast implant.
You may not have any symptoms with BIA-ALCL and it may only be detected when you have an ultrasound or mammogram. If you do have symptoms in early-stage BIA-ALCL, you may notice a lump or swelling in your breast around the implant. IN later stage disease, you may have any of the symptoms listed above.
Staging of lymphoma
Once you know you have Anaplastic Large Cell Lymphoma, your doctor will want to do more tests to see if the lymphoma has spread to other parts of your body. These tests are called staging.
Other tests will look at how different your lymphoma cells are from your normal T-cells and how quickly they are growing. This is called grading.
Click on the headings below to learn more.
Staging refers to how much of your body is affected by your lymphoma or, how far it has spread from where it first started.
T-cells can travel to any part of your body. This means that lymphoma cells (the cancerous T-cells), can also travel to any part of your body. You will need to have more tests done to find this information. These tests are called staging tests and when you get results, you will find out if you have stage one (I), stage two (II), stage three (III) or stage four (IV) ALCL.
Your stage of ALCL will depend on:
- How many areas of your body have lymphoma.
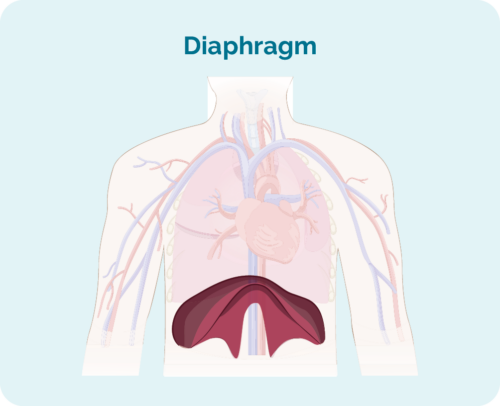
- Where the lymphoma is including if it is above, below or on both sides of your diaphragm (a large, dome-shaped muscle under your rib cage that separates your chest from your abdomen).
- Whether the lymphoma has spread to your bone marrow or other organs such as the liver, lungs, skin or bone.
Stages I and II are called ‘early or limited stage’ (involving a limited area of your body).
Stages III and IV are called ‘advanced stage’ (more widespread).
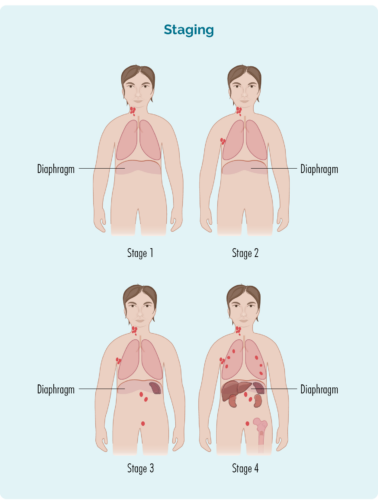
Stage 1 | one lymph node area is affected, either above or below the diaphragm |
Stage 2 | two or more lymph node areas are affected on the same side of the diaphragm |
Stage 3 | at least one lymph node area above and at least one lymph node area below the diaphragm are affected |
Stage 4 | lymphoma is in multiple lymph nodes and has spread to other parts of the body (e.g. bones, lungs, liver) |
Extra staging information
Your doctor may also talk about your stage using a letter, such as A,B, E, X or S. These letters give more information about the symptoms you have or how your body is being affected by the lymphoma. All this information helps your doctor find the best treatment plan for you.
Letter | Meaning | Importance |
A or B |
|
|
E & X |
|
|
S |
|
(Your spleen is an organ in your lymphatic system that filters and cleans your blood, and is a place your B-cells rest and make antibodies) |
Tests for staging
To find out what stage you have, you may be asked to have some of the following staging tests:
Computed tomography (CT) scan
These scans takes pictures of the inside of your chest, abdomen or pelvis. They provide detailed pictures that provide more information than a standard X-ray.
Positron emission tomography (PET) scan
This is a scan that takes pictures of the inside of your whole body. You will be given and needle with some medicine that cancerous cells – such as lymphoma cells absorb. The medicine that helps the PET scan identify where the lymphoma is and the size and shape by highlighting areas with lymphoma cells. These areas are sometimes called “hot”.
Lumbar puncture
A lumbar puncture is a procedure done to check if the lymphoma has spread to your central nervous system (CNS), which includes your brain, spinal cord and an area around your eyes. You will need to stay very still during the procedure, so babies and children may have a general anaesthetic to put them to sleep while the procedure is done. Most adults will only need a local anaesthetic for the procedure to numb the area.
Your doctor will put a needle into your back, and take out a little bit of fluid called “cerebral spinal fluid” (CSF) from around your spinal cord. CSF is a fluid that acts a bit like a shock absorber to your CNS. It also carries different proteins and infection fighting immune cells such as lymphocytes to protect your brain and spinal cord. CSF can also help drain any extra fluid you may have in your brain or around your spinal cord to prevent swelling in those areas.
The CSF sample will then be sent to pathology and checked for any signs of lymphoma.
Bone marrow biopsy
- Bone marrow aspirate (BMA): this test takes a small amount of the liquid found in the bone marrow space.
- Bone marrow aspirate trephine (BMAT): this test takes a small sample of the bone marrow tissue.
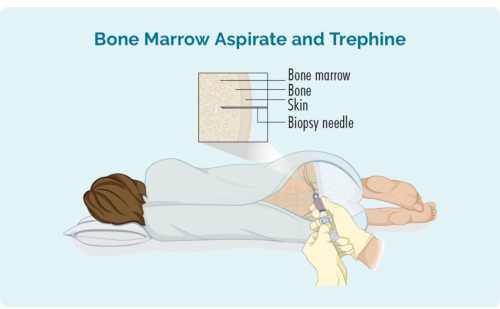
The samples are then sent to pathology where they are checked for signs of lymphoma.
The process for bone marrow biopsies can differ depending on where you are having your treatment, but will usually include a local anaesthetic to numb the area.
In some hospitals, you may be given light sedation which helps you to relax and can stop you from remembering the procedure. However many people do not need this and may instead have a “green whistle” to suck on. This green whistle has a pain killing medication in it (called Penthrox or methoxyflurane), that you use as needed throughout the procedure.
Make sure you ask your doctor what is available to make you more comfortable during the procedure, and talk to them about what you think will be the best option for you.
More information on bone marrow biopsies can be found at our webpage here
Your lymphoma cells have a different growth pattern, and look different to normal cells. The grade of your lymphoma is how quickly your lymphoma cells are growing, which affects the way look under a microscope. The grades are Grades 1-4 (low, intermediate, high). If you have a higher grade lymphoma, your lymphoma cells will look the most different from normal cells, because they are growing too quickly to develop properly. An overview of the grades is below.
- G1 – low grade – your cells look close to normal, and they grow and spread slowly.
- G2 – intermediate grade – your cells are starting to look different but some normal cells exist, and they grow and spread at a moderate rate.
- G3 – high grade – your cells look fairly different with a few normal cells, and they grow and spread faster.
- G4 – high grade – your cells look most different to normal, and they grow and spread the fastest.
All this information adds to the whole picture your doctor builds to help decide the best type of the treatment for you.
It is important that you talk to your doctor about your own risk factors so you can have clear idea of what to expect from your treatments.
Waiting for Results
Waiting for your results can be a stressful and worrying time. It is important to talk about how you are feeling. If you have a trusted friend or family member it can be good to talk to them. But, if you don’t feel you can talk to anyone in your personal life, talk to your local doctor, they can help organise counselling or other support so you are not alone as you go through the waiting times and treatment for ALCL.
You can also contact our Lymphoma Care Nurses by clicking on the Contact Us button at the bottom of the screen. Or if you are on Facebook and would like to connect other patients living with lymphoma you can join our Lymphoma Down Under page.
Before you start treatment
Aggressive subtypes of ALCL can spread quickly, so you will need to start treatment soon after you are diagnosed. However, there are some things to consider before you start treatment.
Fertility
Some treatments for lymphoma can affect your fertility, making it harder to get pregnant, or get someone else pregnant. This can happen with several different types of anticancer treatments including:
- chemotherapy
- radiotherapy (when it is too your pelvis)
- antibody therapies (monoclonal antibodies and immune checkpoint inhibitors)
- stem cell transplants (because of the high-dose chemotherapy you will need before the transplant).
Questions to ask your Doctor
Treatment of ALCL
Once all the results from your biopsy and staging scans have been completed, your doctor will review them to decide the best possible treatment options for you. They may even meet with other specialists in a multidisciplinary meeting to make sure all your needs are covered.
Some things they will consider when deciding the best treatment options to offer you include:
- the subtype and stage of lymphoma you have
- any symptoms you’re getting
- how the lymphoma is affecting your body
- your age
- any other medical conditions you have, medications you’re taking, and your over health and wellbeing
- your own preferences once you have all the information.
Before treatment is started it is important that adequate information is provided about the treatment that is planned, the possible side effects and what to expect. Education from the cancer nurses prior to receiving treatment, can be extremely helpful and should include instructions about becoming unwell or needing medical or nursing assistance.
If your PcALCL is confined to your skin, and not causing you any symptoms or distress, you may not need any treatment at all. This is because PcALCL that is confined to your skin is not harmful to your health and will not make you unwell or shorten your life.
If your PcALCL is causing pain, itching or bleeding or the look of it is causing you distress you may be able to have treatment to improve these symptoms. The treatment will not be to cure you of the PcALCL, but to manage the symptoms.
Treatment for early stage PcALCL
Topical treatments – creams or lotions that you run into the area of skin affected.
Intralesional steroids – These may be used if the topical treatments don’t work. Your doctor will inject a small amount of steroid into the area of your skin affected by the PcALCL. Steroids are toxic to lymphoma cells, so can reduce the number of lymphoma cells in the area and improve your symptoms.
Radiotherapy – You may be offered radiotherapy, which is a treatment that uses radiation such as X-ray, proton beams or gamma rays destroy the lymphoma cells.
Surgery – Your PcALCL may be able to removed completely with surgery. This will depend on the size and location of your PcALCL.
Treatment for advanced stage PcALCL
BIA-ALCL can be indolent and localised to your breast, or can be more aggressive and spread to other areas of your body including your lymph nodes and organs.
The treatment plan your doctor offers, will be tailored to how your BIA-ALCL behaves and how far it has spread.
Early-stage BIA-ALCL
For early-stage BIA-ALCL that is only in your breast, you may only need surgery to remove the implant and areas affected by lymphoma within the breast. You may be able to have different implants inserted following the surgery or may decide not to. This is a conversation you should have with your surgeon and hematologist to help you understand risks and benefits of different implants.
There are many reasons people have breast implants, and the thought of having them removed, as well as having a lymphoma diagnosis can be very overwhelming and upsetting. If you are struggling with your emotions during this time, please reach out to your medical team. There is help available to get you through, and help you make good decisions about your health.
Late-stage BIA-ALCL
BvCHP – cyclophosphamide, doxorubicin, prednisolone and a monoclonal antibody called brentuximab vedotin (Bv). Bv is only effective against lymphomas with a protein called CD30 on them.
CHOP – combination chemotherapy of cyclophosphamide, doxorubicin, vincristine and a steroid called prednisolone.
CHOEP – similar to CHOP but with an extra chemotherapy called etoposide.
Systemic ALK +ve ALCL is a systemic and aggressive type of lymphoma so you will need to start treatment soon after you are diagnosed. Treatment may include chemotherapy with or without radiotherapy.
- Chemotherapy – common chemotherapy protocols used for systemic ALCL include:
BvCHP – cyclophosphamide, doxorubicin, prednisolone and a monoclonal antibody called brentuximab vedotin (Bv). Bv is only effective against lymphomas with a protein called CD30 on them.
CHOP – combination chemotherapy of cyclophosphamide, doxorubicin, vincristine and a steroid called prednisolone.
CHOEP – similar to CHOP but with an extra chemotherapy called etoposide.
- Clinical trial participation
Treatment for children with ALK +ve ALCL
Many children with lymphoma will be offered to participate in clinical trials. It is best to talk to your child’s haematologist about the best treatment options for you child, as they may differ from those listed here.
Systemic ALK -ve ALCL is a systemic and aggressive type of lymphoma so you will need to start treatment soon after you are diagnosed. Treatment for systemic ALK -ve ALCL is similar to systemic ALK +ve ALCL and may include chemotherapy with or without radiotherapy.
- Chemotherapy – common chemotherapy protocols used for systemic ALCL include:
BvCHP – cyclophosphamide, doxorubicin, prednisolone and a monoclonal antibody called brentuximab vedotin (Bv). Bv is only effective against lymphomas with a protein called CD30 on them.
CHOP – combination chemotherapy of cyclophosphamide, doxorubicin, vincristine and a steroid called prednisolone.
CHOEP – similar to CHOP but with an extra chemotherapy called etoposide.
- Stem cell transplant – You may also be offered high-dose chemotherapy followed by a stem cell transplant if you have systemic ALK -ve ALCL. Learn more about stem cell transplants by clicking here.
- Clinical trial participation
Clinical Trials
It is recommended that anytime you need to start new treatments, you ask your doctor about clinical trials you may be eligible for. Clinical trials are important to find new medicines, or combinations of medicines to improve treatment of ALCL in the future.
They can also offer you a chance to try a new medicine, combination of medicines or other treatments that you would not be able to get outside of the trial.
There are many treatments and new treatment combinations that are currently being tested in clinical trials around the world for patients with both newly diagnosed and relapsed ALCL.
Common side effects of treatment
The side-effects of treatment will depend on the type of treatment you are having, the location and size of your lymphoma as well as other factors. It is important to understand what the most common, and the most serious side-effects of your treatment are. Talk to your doctor or specialist cancer nurse about the expected side-effects of you treatment are.
Some questions you should consider consider them include:
- What is the name of the treatment I am having?
- What type of treatment is it (is it chemotherapy, or a monoclonal antibody etc.)?
- What are the common and possible side effects for the treatment?
- What side effects do you need to report to the medical team?
- What are the contact numbers, and where to attend in case of emergency 7 days a week and 24 hours per day?
For generic information on common side-effects and how to manage them, please click the link below.
Relapsed or refractory ALCL
After treatment, many patients can have a period of remission (no signs of lymphoma or when the lymphoma is under control). In some patients the lymphoma comes back (relapses) or in rare cases does not respond to the initial treatment (refractory).If this happens there are other treatments that can be successful and can include:
- Pralatrexate
- Romidepsin
- Vorinostat (for relapsed or refractory PcALCL)
- Brentuximab vedotin (Adcetris)
- Combination chemotherapy
- Targeted therapy
- Stem cell transplant
Clinical Trials
It is recommended that anytime you need to start new treatments, you ask your doctor about clinical trials you may be eligible for. Clinical trials are important to find new medicines, or combinations of medicines to improve treatment of ALCL in the future.
They can also offer you a chance to try a new medicine, combination of medicines or other treatments that you would not be able to get outside of the trial.
There are many treatments and new treatment combinations that are currently being tested in clinical trials around the world for patients with both newly diagnosed and relapsed ALCL.
What to expect when treatment finishes
When you finish your treatment your haematologist will still want to see you regularly. You will have regular check-ups including blood tests and scans. How often you have these tests will depend on your individual circumstance, and your haematologist will be able to tell you how often they want to see you.
It can be an exciting time or a stressful time when you finish treatment – sometimes both. There is no right or wrong way to feel. But it is important to talk about your feelings and what you need with your loved ones.
Support is available if you are having a difficult time coping with the end of treatment. Talk to your treating team – your haematologist or specialist cancer nurse as they may be able to refer you for counselling services within the hospital. Your local doctor (general practitioner – GP) can also help with this.
Lymphoma Care Nurses
You can also speak to our Lymphoma Care Nurses. Just click on the “Contact Us” button at the bottom of the screen for contact details.
Late Effects
Sometimes a side-effect from treatment may continue, or develop months or years after you finish treatment. This is called a late-effect. It is important to report any late effects to your medical team so they can review you and advise you how best to manage these effects. Some late effects can include:
- Changes to your heart rhythm or structure
- Effects to your lungs
- Peripheral neuropathy
- Hormonal changes
- Mood changes.
If you experience any of these late effects, your haematologist or general practitioner may recommend you see another specialist to manage these effects and improve your quality life. It is important though to report all new, or lasting effects as early as possible for the best outcomes.
Survivorship - Living with and after cancer
A healthy lifestyle, or some positive lifestyle changes after treatment can be a great help to your recovery. There are many things you can do to help you live well with ALCL.
Many people find that after a cancer diagnosis or treatment, that their goals and priorities in life change. Getting to know what your ‘new normal’ is can take time and be frustrating. Expectations of your family and friends may be different to yours. You may feel isolated, fatigued or any number of different emotions that can change each day.
The main goals after treatment for your ALCL is to get back to life and:
- be as active as possible in your work, family, and other life roles
- lessen the side effects and symptoms of the cancer and its treatment
- identify and manage any late side effects
- help keep you as independent as possible
- improve your quality of life and maintain good mental health.
Different types of cancer rehabilitation may also be recommended to you. This could mean any of a wide range of services such as:
- physical therapy, pain management
- nutritional and exercise planning
- emotional, career and financial counselling.
It can also help to talk to your local doctor about what local wellness programs are available for people recovering from a cancer diagnosis. Many local areas run exercise or social groups or other wellness programs to help you get back to your pre-treatment self.
Summary
- Anaplastic Large Cell Lymphoma (ALCL) is a type of Non-Hodgkin Lymphoma and a subtype of Peripheral T-cell Lymphoma (PTCL).
- It starts when your T-cell lymphocytes mutate and become cancerous.
- T-cells are made in our bone marrow but travel to, and mature in our thymus. They can travel to any part of our body to fight infection and disease.
- There are four different subtypes of ALCL and they can be indolent or aggressive.
- Treatment for ALCL will depend on the subtype and stage of ALCL you have, and whether it is indolent or aggressive.
- ALCL can respond well to treatment and you may go into a time of remission however, relapse is not uncommon so you may need treatment more than once.
- Report all new or worsening symptoms to your doctor including B-symptoms.
- You are not alone. Reach out to your haematology team or GP if you need to, or contact our Lymphoma Care Nurses by clicking on the “Contact Us” button at the bottom of the screen.


