Overview of PCNSL
PCNSL develops when cancerous B-cell lymphocytes (B-cells) form in the lymphoid tissue of the brain and/or spinal cord. PCNSL may also start in the layers that form the outer covering of the brain (meninges) or in the eyes (ocular lymphoma).
Sometimes lymphoma can start in other areas of the body and spread to the CNS. This is defferent to PCNSL and is treated differently too. If it has started outside of the CNS and spread to the CNS it is called secondary CNS lymphoma.
The cause of PCNSL is unknown as is the case of many lymphomas. People are more likely to be affected between the age of 50 to 60 years, with the average age of diagnosis around 60 years, however it can occur at any age. PCNSL is also slightly more common in people who have a weakened immune system, which may be caused by:
- HIV (human immunodeficiency virus) infection – this is less common now due to the availability of effective antiviral treatments
- Medications – those that are used to suppress the immune system, such as after an organ transplant or other types of immunosuppressive treatments for autoimmune conditions e.g. rheumatoid arthritis.
Is PCNSL curable?
Many aggressive lymphomas can respond well to treatments with chemotherapy because chemotherapy works by killing off fast growing cells. There are many factors however, that impact whether you will be cured from your lymphoma or not. Many people can be cured, others may have periods of remission – where there is no sign of lymphoma left in your body, but then it can relapse (come back) and need more treatment.
To find out more about your chances of a cure, talk to your haematologist or oncologist.
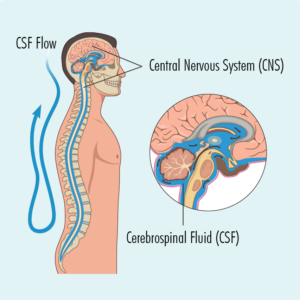
What does the Central Nervous System (CNS) do?
The central nervous system (CNS) is the part of our body that controls all our bodily functions. It includes our brain, spinal cord and eyes.
The brain
Our brain is made up of:
- Cerebrum – this controls our speech and understanding, our sensations and voluntary movement (the movements we decide to make)
- Cerebellum – helps with movements and controls our balance
- Brainstem – controls essential body functions, such as our breathing, heart rate and blood pressure
The spinal cord
Our spinal cord runs from our brain down our back within the bones of the spine. A series of nerves join directly onto the spinal cord. The nerves carry information about sensation from around the body and carries messages to and from our brain to the rest of our body, to control our muscles, and all our body functions.
How is our CNS protected?
Our CNS is separated from the rest of our body and protected from trauma, infection and disease in several ways.
- The meninges are protective layers of tissue that cover the brain and spinal cord – this is what becomes inflamed in ‘meningitis’
- A special fluid called ‘cerebrospinal fluid’(CSF) surrounds the brain and spinal cord to cushion them – it is found in the space between the meninges and the brain and spinal cord.
- The blood-brain barrier surrounds our brain – it is a barrier of cells and blood vessels that only lets certain substances reach the brain. This protects it from harmful chemicals and infections, and it also prevents or interferes with many chemotherapy drugs passing from the blood to the brain.
To understand PCNSL you need to know a bit about your B-Cell lymphocytes.
B-Cell lymphocytes:
- Are a type of white blood cell
- Fight infection and diseases to keep you healthy.
- Remember infections you had in the past, so if you get the same infection again, your body’s immune system can fight it more effectively and quickly.
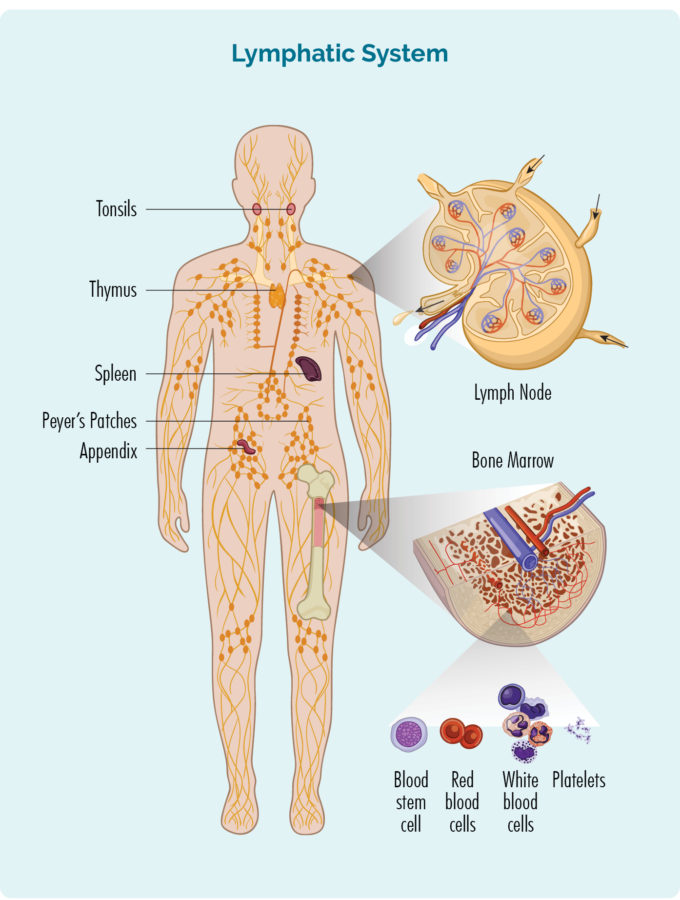
- Are made in your bone marrow (the spongy part in the middle of your bones), but usually live in your lymphatic system which includes your:
- lymph nodes
- lymphatic vessels and lymph fluid
- organs – spleen, thymus, tonsils, appendix
- lymphoid tissue
- Can travel through your lymphatic system, to any part of your body to fight infection or disease.
What happens when PCNSL develops?
PCNSL develops when cancerous lymphocytes are found in your central nervous system (CNS), which includes your brain, spinal cord, eyes, cranial nerves and the protective layer of tissue that covers your brain and spinal cord called meninges.
When you have PCNSL, your cancerous lymphocytes:
- Grow uncontrollably
- Will not work as effectively to fight infections and disease
- Can become larger than they should and can look different to your healthy B-cells
- Can cause lymphoma to develop in your brain, spinal cord and eyes.
- Because of the protective barriers around our CNS, PCNSL does not usually spread to other parts of your body like other types of lymphoma can however, they can sometimes to spread the testes in males.
Symptoms when lymphoma is in your Central Nervous System (CNS)
Symptoms of lymphoma in your CNS are related to the functions of your brain, eyes and spinal cord. They will depend on what part of your CNS affected and may include the following:
- headaches
- changes to your vision
- confusion or memory changes
- a change in consciousness (becoming drowsy and unresponsive)
- difficulty speaking or swallowing
- changes in your mood or personality
- seizures (fits)
- nausea and vomiting
- loss appetite (not wanting to eat) and weight loss
- difficulty going to the toilet
- difficulty walking, unsteadiness or falls
- weakness, numbness or tingling feelings.
Diagnosis, staging and grading of PCNSL
If your doctor suspects you may have lymphoma you will need to have several tests done. Unlike other subtypes of lymphoma, staging is not done if you have PCNSL because the lymphoma is confined to your central nervous system (CNS). Any spread outside of the CNS is usually only in males and only to the testes.
PCNSL is always considered a high-grade lymphoma meaning that it is aggressive. It grows quickly and can move through your CNS quickly. The cancerous B-cells (lymphoma cells) also look very different from your healthy B-cells because they grow too fast and do not have time to form properly.
Click on the heading below to learn more about the kind of tests you may have to diagnose, and learn more about your PCNSL.
Biopsy
To diagnose PCNSL you will need a biopsy. A biopsy is a procedure to remove part, or all of an affected lymph node or affected tissue. During the procedure you may have either a general or local anaesthetic to make you more comfortable, or to ensure you are not awake while it is done.
The type of biopsy to be done will depend on where the lymphoma is located.
If the lymphoma is thought to be in your:
- Brain – a neurosurgeon (a specialist in diagnosing and treating problems with the CNS) takes a brain biopsy. Lumps (or samples of the lumps) within your brain will be removed using a CT scan to help guide the biopsy needle to the right area. This is called a ‘stereotactic biopsy’. You will have a general anaesthetic for this procedure as it is important not to move.
- Eye – an ophthalmologist (specialist in diseases and injuries of the eye) may take a little of the vitreous (gel-like substance inside your eye) to check for lymphoma cells.
- Spine – a specialist radiologist may take a biopsy from your spine.
Blood tests
Blood tests are also taken when trying to diagnose your lymphoma, but also throughout treatment so the doctor can get a better understanding of your overall health, and make sure your organs are working properly to cope with treatment.
This type of scan is often used in combination with a CT scan to detect active lymphoma elsewhere in your body. It takes a picture of the inside of your whole body. You will be given a needle with some medicine that cancerous cells such as lymphoma cells, absorb. The medicine helps the PET scan to identify where the lymphoma is and the size and shape by highlighting areas with lymphoma cells. These are sometimes called “hot”.
As PCNSL can affect the eyes you may also need various ophthalmic tests. An ophthalmologist (eye specialist) will use an ophthalmoscope – an instrument with a light and small magnifying lens – to get a good look inside your eye. Certain imaging tests may be done and these help the ophthalmologist look at the tumour as well as see if the cancer has spread.
A biopsy of the eye may be needed. This is called a vitrectomy. A tiny instrument is inserted into the eye and it takes samples of the jelly-like vitreous, which is the substance that fills the middle of the eye.
A testicular ultrasound for men is a test that takes images of the testicles and the surrounding tissues in the scrotum.
This is done because some lymphomas start in the testes and spread to the central nervous system (CNS). If the lymphoma is found in your testes, then it is most likely that your CNS lymphoma is secondary rather than primary, and will therefore need different treatment.
Most testicular lymphomas are a subtype of Diffuse Large B-cell Lymphoma (DLBCL), but some are a subtype of Burkitt’s lymphoma, Mantle Cell Lymphoma (MCL), Follicular Lymphoma, or T-cell lymphoma.
Click on the links below to find more information on these subtypes.
Results
Waiting for all your results to come in can be a very stressful time for you and your loved ones. It is important to talk about how you are feeling and be open with those around you about what you need. Many people want to help, but don’t know how so by letting them know what you need, you can help them to provide the support you need.
It may also help to start planning out what you may need in the coming months if you do need to have treatment. We have put some tips together on our Living with Lymphoma – The Practical Stuff webpage. Click on the link below to be directed to that page.
You can also contact our Nurse Hotline to talk to one of our Lymphoma Care Nurses. Just click on the Contact us button at the bottom of this page.
You may also like to join one of our social media pages to chat with other people living with. Connect with our social media pages by clicking the links at the top of the page.
Treatment for PCNSL
Having the right information can help you feel more confident and know what to expect, and can help you plan ahead for what you may need. But it can be difficult to know what questions to ask when you are starting treatment. If you don’t know, what you don’t, how can you know what to ask?
We have put together a list of questions you may find helpful. Of course, everyone’s situation is unique, so these questions do not cover everything, but they do give a good start. Click on the link below to find a PDF copy that you can download and print if you like.
Fertility preservation
Whether you are male or female, many anti-cancer treatments can affect your fertility – your ability to make babies. If you would like to have babies after treatment, or are not sure if you would, talk to your doctor about what options are available to help protect your fertility during treatment.
Overview of treatment types
Click through the slides below for an overview of the different types of treatment that you may be offered to treat your PCNSL.
However, if you are having severe symptoms and your doctor is fairly confident you have PCNSL, they may to choose to start steroids to improve your symptoms even before your biopsy.
Steroids are also toxic to lymphoma cells so they can help to shrink the lymphoma while waiting for other treatment to start.
Steroids can be given intravenously (through a vein) or orally (by mouth). A common steroid is dexamethasone.
The chemo you get for PCNSL may be different to people with other subtypes of lymphoma, as the medications need to cross your blood-brain barrier to get to your lymphoma. It is common to have chemotherapy with an immunotherapy such as rituximab.
You may have a MAB infusion at a cancer clinic or hospital. MABs attach to the lymphoma cell and attract other diseases-fighting white blood cells and proteins to the cancer so your own immune system can fight the PCNSL.
Whole-brain radiotherapy is usually used as a consolidation treatment after chemotherapy.
Until the mid-nineties it was the main treatment for PCNSL, however now it is given in combination with chemotherapy. Consolidation treatments aim to reduce the risk of relapse (the lymphoma returning). Radiotherapy can be used on its own if you are unable to tolerate chemotherapy.
A SCT is done to replace your diseased bone marrow with new stem cells that can grow into new healthy blood cells. With a SCT, the stem cells are removed from the blood. The stem cells may be removed from a donor or collected from you after you’ve had chemotherapy.
If the stem cells come from a donor, it is called an allogeneic stem cell transplant. If your own stem cells are collected, it is called an autologous stem cell transplant.
First-line treatment
You will need to start treatment soon after all your test results come back. In some cases, you may start before all the test results are in. It can be quite overwhelming when you start treatment. You may have many thoughts about how you will cope, how to manage at home, or how sick you might get.
Let your treating team know if you feel you may need extra support. They may be able to help by referring you to see a social worker or other health care professional to help you work out some everyday living challenges you may face. You can also reach out to the Lymphoma Care Nurses by clicking on the “Contact us” button at the bottom of this page.
When you do start treatment for the first time, it is called ‘first-line treatment’. You may have more than one medicine, and these may include radiotherapy, chemotherapy or a monoclonal antibody.
The standard first-line treatment can include:
High-dose methotrexate
This may be combined with or without the monoclonal antibody, rituximab.
MATRix
This is a combination of different chemotherapy medicines and a monoclonal antibody – methotrexate, cytarabine, thiotepa and rituximab – for newly diagnosed PCNSL.
R-MPV (Part one and Part two)
Part one – Monoclonal antibody (rituximab) and combination of chemotherapy including methotrexate, procarbazine and vincristine.
Part two – High-dose chemotherapy – cytarabine
Methotrexate and cytarabine
A combination of two chemotherapies for newly diagnosed PCNSL.
Intrathecal chemotherapy
This is chemotherapy that is given in the spinal fluid by a means of a lumbar puncture. This is done if lymphoma is found in your spinal fluid.
Clinical trial participation
These may include clinical trials for targeted therapies and other treatments. Ask your doctor if you are eligible for any first-line treatment clinical trials.
Radiotherapy or Stem Cell Transplant
If the lymphoma responds to chemotherapy, your medical team may suggest whole-brain radiotherapy or an autologous stem cell transplant (see above). These are consolidation treatments, which means they are used to reduce the risk of relapse after successful treatment.
Second-line and ongoing treatment
If your CNS lymphoma relapses (comes back) or is refractory (does not respond) to treatment, there may be other treatments available.
Treatment you have if you relapse or have refractory PCNSL is called second-line treatment. The treatment depends on how fit you are at the time, what treatment you have already had and how the lymphoma is affecting you. Your specialist can talk you through your options, which may include:
- More intense (stronger) chemotherapy, possibly followed by an autologous stem cell transplant (not suitable for some people).
- Radiotherapy – if it hasn’t already been given.
- Palliative treatments given with the aim to relieve symptoms.
- Clinical trial participation.
Clinical Trials
It is recommended that anytime you need to start new treatments you ask your doctor about clinical trials you may be eligible for.
Clinical trials are an important way to find new medicines, or combinations of medicines to improve treatment of PCNSL in the future. They can also offer you a chance to try a new medicine, combination of medicines or other treatments that you would not be able to get outside of the trial. If you are interested in participating in a clinical trial, ask your doctor what clinical trials you are eligible for.
Prognosis for PCNSL
Prognosis is the term used to describe the likely path of your disease, how it will respond to treatment and how you will do during and after treatment.
There are many factors that contribute to your prognosis and it’s not possible to give an overall statement about prognosis.
Factors that can impact prognosis
Some factors that may impact your prognosis include:
- Your age and overall health at the time of diagnosis
- How you respond to treatment
Sometimes the symptoms of CNS lymphoma resolve quickly with treatment. Initial treatment with steroids can be very effective in relieving symptoms. However, nerve tissues grow very slowly, and it can sometimes take a while for symptoms to improve. Some of you may see gradual improvements in symptoms, some however, may find symptoms may never fully resolve, especially if they were present before treatment.
Getting support
Your medical team can support your recovery by referring you to the appropriate specialists. If you experience muscle weakness and strength loss or do not recover quickly, you should consider seeing a physiotherapist and/or occupational therapist as they can offer help and advice to improve quality of life. Their help might also stop symptoms from worsening or other problems developing in the longer term.
Psychologists can offer support if there are cognitive (thinking) problems, such as memory or attention problems. Psychologists and counsellors can also support with the emotional impact of your lymphoma.
It is important to note that treatment strategies for PCNSL have improved greatly over recent years. However, PCNSL can be difficult to treat, and some treatments have a risk of causing long-term neurological problems (problems with the brain and eyes). These problems become more likely if you are diagnosed with CNS lymphoma when you are older.
Survivorship - Living with, and after cancer
A healthy lifestyle, or some positive lifestyle changes after treatment can be a great help to your recovery. There are many things you can do to help you live well after Burkitt’s.
Many people find that after a cancer diagnosis, or treatment, that their goals and priorities in life change. Getting to know what your ‘new normal’ is can take time and be frustrating. Expectations of your family and friends may be different to yours. You may feel isolated, fatigued or any number of different emotions that can change each day.
The main goals after treatment for your lymphoma is to get back to life and:
- be as active as possible in your work, family, and other life roles
- lessen the side effects and symptoms of the cancer and its treatment
- identify and manage any late side effects
- help keep you as independent as possible
- improve your quality of life and maintain good mental health
Different types of cancer rehabilitation may be recommended to you. This could mean any of a wide range of services such as:
- physical therapy, pain management
- nutritional and exercise planning
- emotional, career and financial counselling.
Summary
- Primary Central Nervous System Lymphoma (PCNSL) is a high-grade aggressive subtype of Non-Hodgkin Lymphoma that is develops in your central nervous system (CNS).
- PCNSL does not usually spread outside of the CNS but can spread to the testes in males.
- PCNSL is different from lymphomas that starts elsewhere in the body and spreads to the CNS (secondary CNS lymphoma) and needs to be treated differently.
- Symptoms of PCNSL are related to the location of the lymphoma, including symptoms related to the functions of your brain, spinal cord and eyes.
- There are several different types of tests you will need to diagnose PCNSL, and these may include procedures where you are given a general or local anaesthetic.
- Treatment for PCNSL is different from other subtypes of lymphoma as medications need to pass through your blood-brain barrier to get to the lymphoma.
- Symptoms may take a while to improve after treatment due to the slow growth of nerve cells, but other symptoms may improve quickly.
- Talk to your doctor about your chances of cure and what to expect from your treatment.
- You are not alone. If you would like to talk to one of our Lymphoma Care Nurses about your lymphoma, treatments and options click the Contact us button at the bottom of the screen.