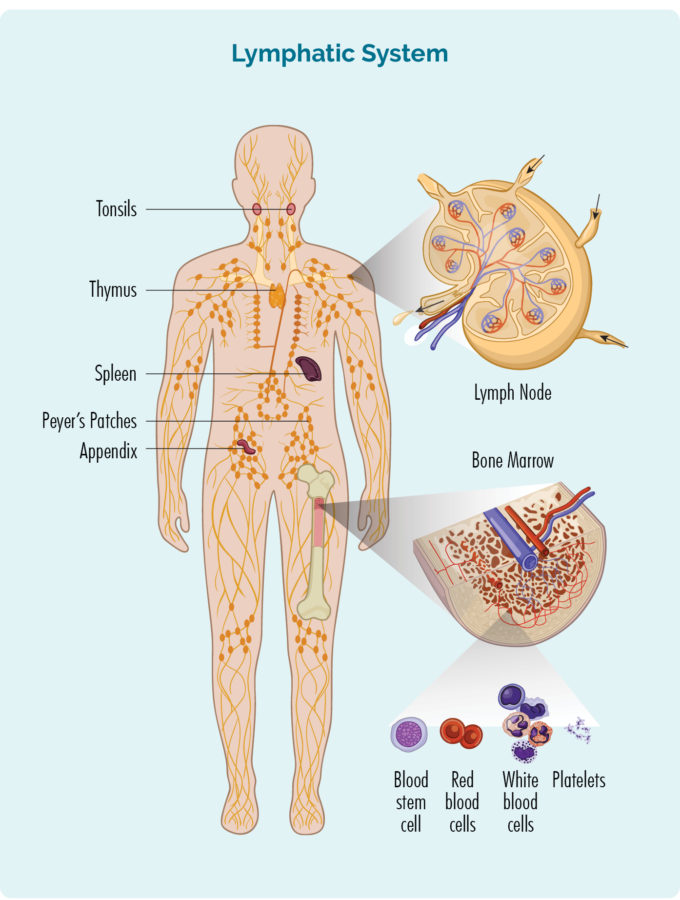
Understanding T-cell Lymphocytes
To understand AITL, you need to know about your T-cell lymphocytes.
T-cell lymphocytes are an important part of our immune system that protect us against infection and disease, and regulate our immune system to prevent autoimmune attacks. Auto immune attacks happen when our immune system is overactive or faulty and begins to fight our own body instead of infection and disease.
T-cells are made in our bone marrow, but before they mature, they travel through our lymphatic system to our thymus where they continue to grow and mature.
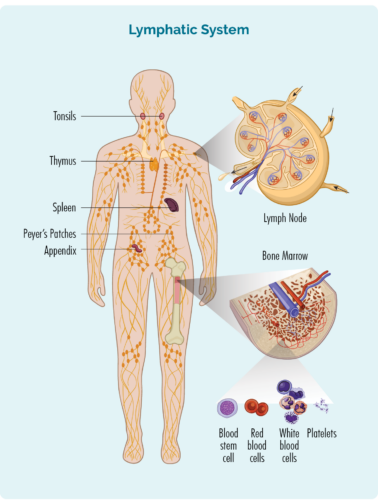
About T-cell Lymphocytes
- T-cells are made in our bone marrow, mature in our thymus, but can live in any part of our lymphatic system – including our lymph nodes.
- T-cells need to be activated to work effectively. They are usually resting in our thymus, lymph nodes or other parts of your lymphatic system, and only wake up and fight infection when other immune cells let them know there is an infection or disease to fight. When they wake up, T-cells can travel to any part of our body to fight the infection or disease.
- Some T-cells are responsible for “regulating” the immune response. This means that once and infection has been destroyed, the “Regulatory T-cells” tell other immune cells to “stand down” so they don’t keep fighting and cause harm to our good cells once the infection is gone.
- After fighting an infection or disease, some T-cells become “Memory T-cells” and they remember everything there is to know about the infection and how to fight it. That way, if we ever get the same infection or disease again, our immune system can fight it a lot more quickly and effectively.
- Some T-cells help other immune cells, such as B-cell lymphocytes to work effectively. These T-cells are called “Helper T-cells”.
What does angioimmunoblastic mean?
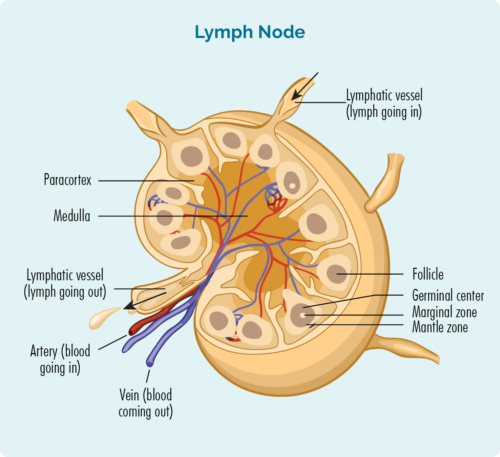
Angio – is a medical name used for blood vessels. In Angioimmunoblastic T-cell Lymphoma, the areas of your body affected by the lymphoma grow extra, small and abnormal blood vessels. This is unique to this subtype of lymphoma.
Immuno – is the name for an immune cell (cells that fight infection and disease) – such as a lymphocyte – in this case, a T-cell lymphocyte.
Blastic – refers to the maturity of the cell. A blast is an immature – not yet fully formed cell.
So Angioimmunoblastic T-cell Lymphoma describes the lymphoma as being from cancerous, immature immune cells (T-cells) with abnormal blood vessels at the site of the lymphoma.
Overview of Angioimmunoblastic T-cell Lymphoma (AITL)
AITL develops when immature T-cells in your lymph nodes or other parts of your lymphatic system become cancerous. We don’t know why this happens in some people, but we know that a change happens in your genes that provide the instructions on how the cells should grow and act. It is thought that if you have had an infection with certain viruses in the past, you may be at increased risk of developing these genetic mutations, however more research is needed to confirm this.
When genetic mutations happen, the cells do not get the right instructions anymore and start to develop with mutations in them that causes them to grow in an uncontrolled way. They become so mutated that they are no longer able to mature and do their job of fighting infection and disease properly.
AITL can affect people of any age including children, but is most common in older adults aged over 60 years.
For more information on how and why lymphoma develops click the link below.
A common symptom of AITL is a lump that comes up under your skin in your neck, armpit or groin that you can see or feel. This is caused by a swollen lymph node as it becomes full of cancerous lymphoma cells. Other symptoms can include:
- Loss of appetite
- Shortness of breath
- Stomach or abdominal discomfort or pain
- Joint pain
- Fatigue
- Itchy skin and/or rashes
- B-symptoms
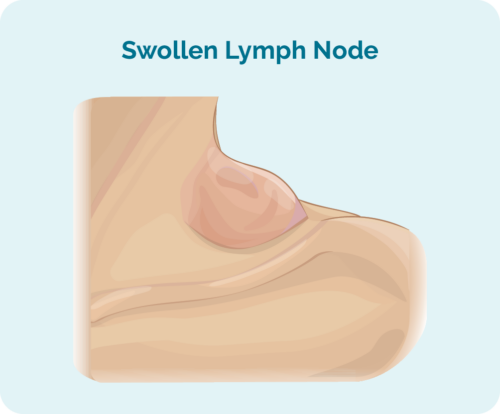
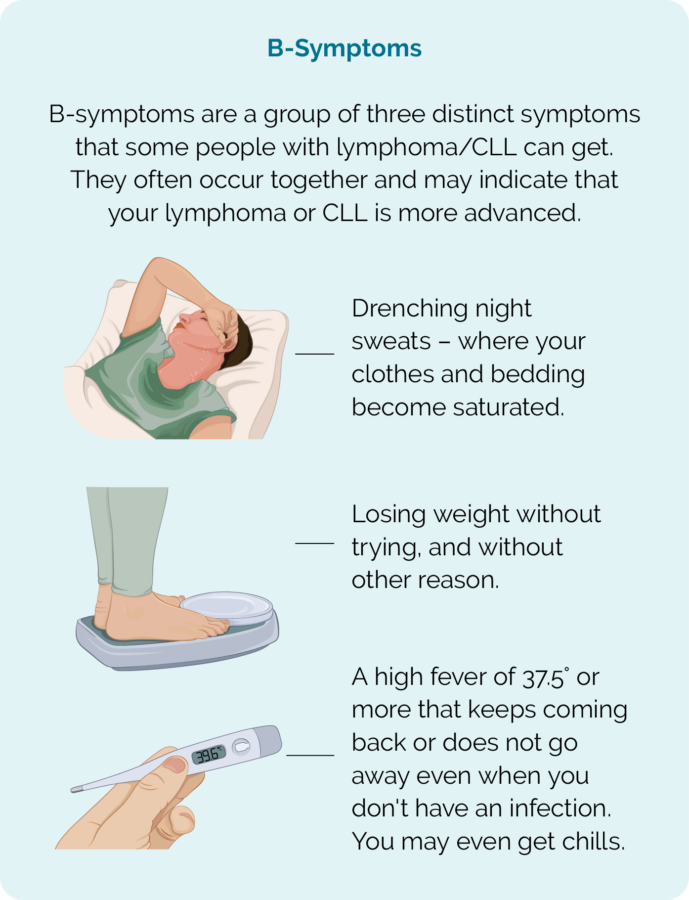
Other symptoms people with lymphoma can get
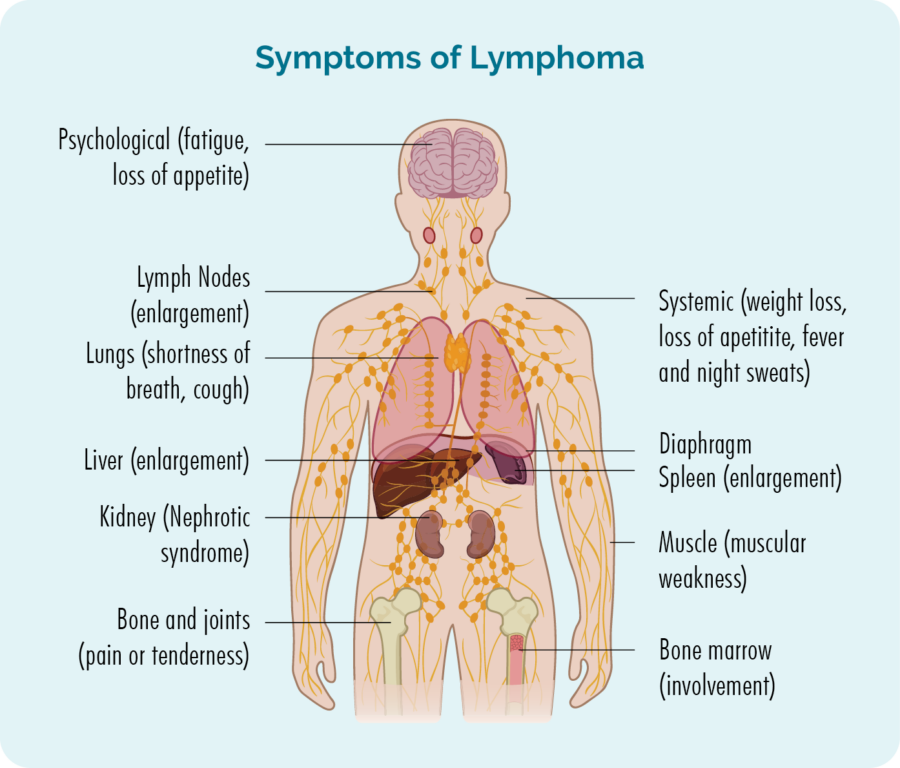
Diagnosis, Staging and Grading of AITL
Diagnosing AITL can sometimes be difficult and can take several weeks.
If your doctor thinks that you may have lymphoma, they will need to organise a number of important tests. These tests are needed to either confirm or rule out lymphoma as the cause for your symptoms. Because there are several different subtypes of AITL, you may have extra tests to find out which one you have. This is important because the management and treatment of your subtype may be different to other subtypes of AITL.
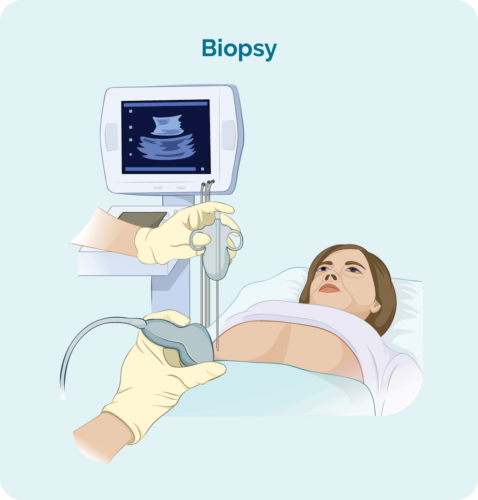
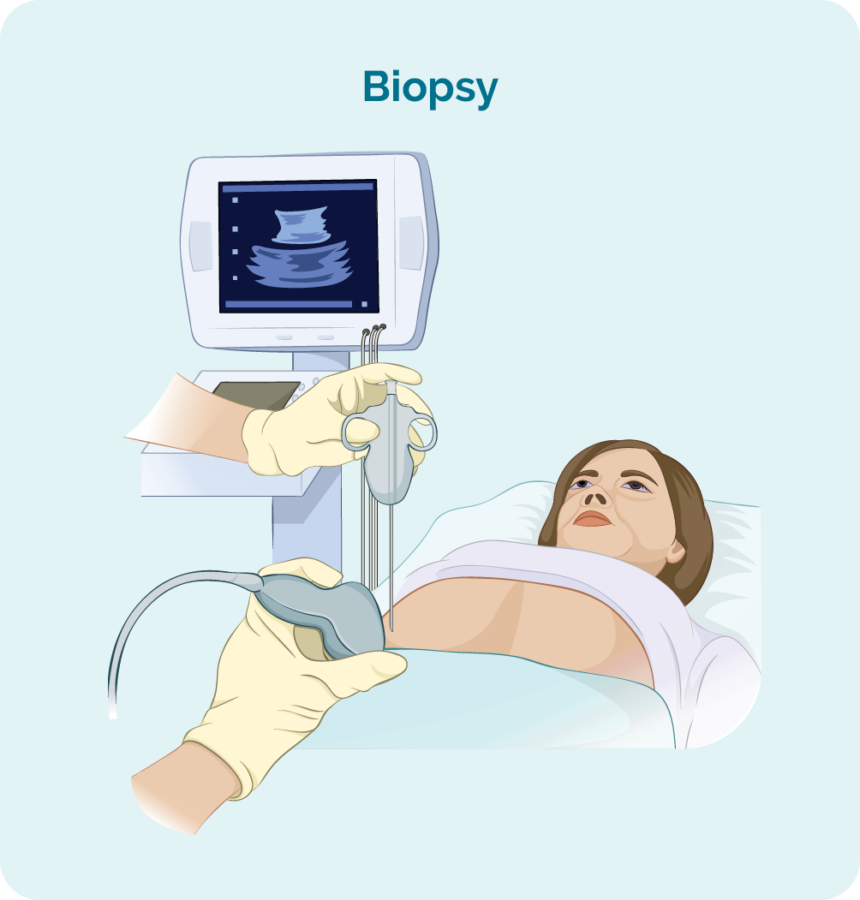
To diagnose AITL you will need a biopsy. A biopsy is a procedure to remove part, or all of an affected lymph node and/ or a bone marrow sample. The biopsy is then checked by a scientist in pathology to see if there are changes that help the doctor diagnose AITL.
When you have a biopsy, you may have a local or general anaesthetic. This will depend on the type of biopsy and what part of your body it is taken from. There are different types of biopsies, and you may need more than one to get the best sample.
Blood tests
Blood tests are taken when trying to diagnose your lymphoma, but also throughout your treatment to make sure your organs are working properly and can cope with your treatment.
Core or fine needle biopsy
Core or fine needle biopsies are taken to remove a sample of swollen lymph node, tumour or affected skin to check for signs of AITL.
Your doctor will usually use a local anaesthetic to numb the area so you don’t feel any pain during the procedure, but you will be awake during this biopsy. They will then put a needle into the swollen lymph node or lump and remove a sample of tissue.
If your swollen lymph node or lump is deep inside your body the biopsy may be done with the help of ultrasound or specialised x-ray (imaging) guidance.
You might have a general anaesthetic for this (which puts you to sleep for a little while). You may also have a few stitches afterwards.
Core needle biopsies take a bigger sample than a fine needle biopsy.
Excisional node biopsy
Excisional node biopsies are done when your swollen lymph node or tumour are too deep in your body to be reached by a core or fine needle biopsy. You will have a general anaesthetic which will put you to sleep for a little while so you stay still, and feel no pain.
During this procedure, the surgeon will remove the whole lymph node or lump and send it to pathology for testing.
You will have a small wound with a few stitches, and a dressing over the top.
Stitches usually stay in for 7-10 days, but your doctor or nurse will give you instruction on how to care for the dressing, and when to return to have the stitches out.
Diagnosis
Staging
Grading
Staging of Angioimmunoblastic T-cell lymphoma (AITL)
Once your diagnosis of AITL is confirmed you have more tests to see how many areas of your body are affected by the lymphoma. This is called staging.
Staging refers to how much of your body is affected by your lymphoma – or, how far it has spread from where it first started.
T-cells can travel to any part of your body. This means that lymphoma cells (the cancerous T-cells), can also travel to any part of your body. You will need to have more tests done to find this information. These tests are called staging tests and when you get results, you will find out if you have stage one (I), stage two (II), stage three (III) or stage four (IV) lymphoma.
Your stage of AITL will depend on:
- How many areas of your body have lymphoma.
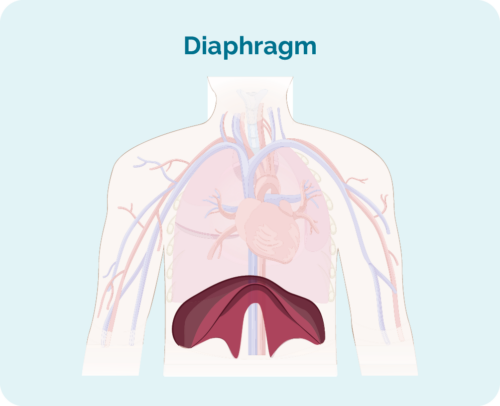
- Where the lymphoma is including if it is above, below or on both sides of your diaphragm (a large, dome-shaped muscle under the rib cage that separates the chest from your abdomen).
- Whether the lymphoma has spread to your bone marrow or other organs such as the liver, lungs, skin or bone.
Stages I and II are called ‘early or limited stage’ (involving a limited area of your body).
Stages III and IV are called ‘advanced stage’ (more widespread).
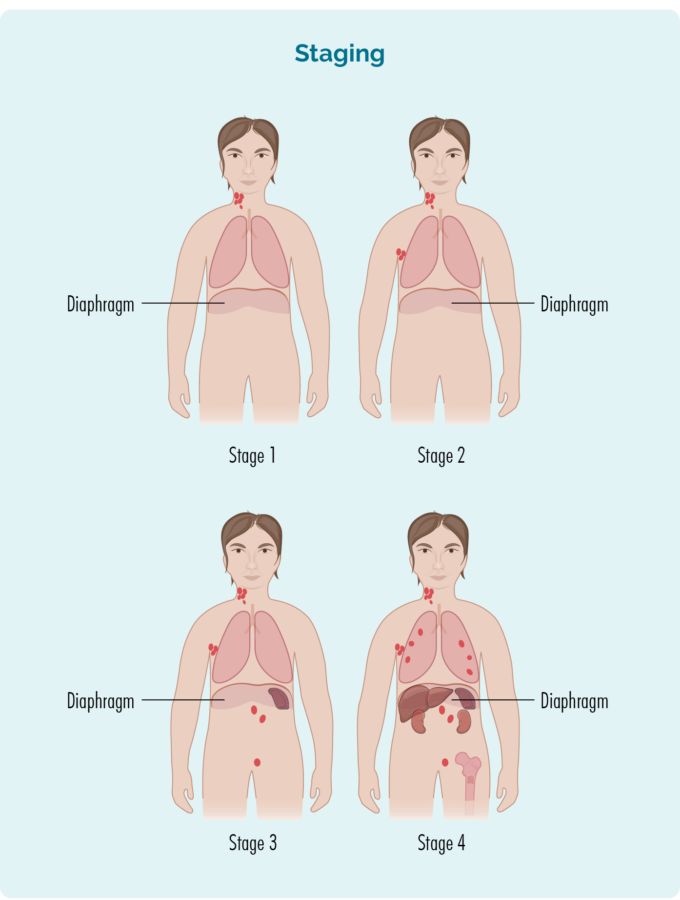
Stage 1 | one lymph node area is affected, either above or below the diaphragm* |
Stage 2 | two or more lymph node areas are affected on the same side of the diaphragm* |
Stage 3 | at least one lymph node area above and at least one lymph node area below the diaphragm* are affected |
Stage 4 | lymphoma is in multiple lymph nodes and has spread to other parts of the body (e.g. bones, lungs, liver) |
Extra staging information
Your doctor may also talk about your stage using a letter, such as A,B, E, X or S. These letters give more information about the symptoms you have or how your body is being affected by the lymphoma. All this information helps your doctor find the best treatment plan for you.
Letter | Meaning | Importance |
A or B |
|
|
E & X |
|
|
S |
|
(Your spleen is an organ in your lymphatic system that filters and cleans your blood, and is a place your B-cells rest and make antibodies) |
Tests for staging
To find out what stage you have, you may be asked to have some of the following staging tests:
Computed tomography (CT) scan
These scans takes pictures of the inside of your chest, abdomen or pelvis. They provide detailed pictures that provide more information than a standard X-ray.
Positron emission tomography (PET) scan
This is a scan that takes pictures of the inside of your whole body. You will be given and needle with some medicine that cancerous cells – such as lymphoma cells absorb. The medicine that helps the PET scan identify where the lymphoma is and the size and shape by highlighting areas with lymphoma cells. These areas are sometimes called “hot”.
Lumbar puncture
A lumbar puncture is a procedure done to check if you have any lymphoma in your central nervous system (CNS), which includes your brain, spinal cord and an area around your eyes. You will need to say very still during the procedure, so babies and children may have a general anaesthetic to put them to sleep for a little while the procedure is done. Most adults will only need a local anaesthetic for the procedure to numb the area.
Your doctor will put a needle into your back, and take out a little bit of fluid called “cerebral spinal fluid” (CSF) from around your spinal cord. CSF is a fluid that acts a bit like a shock absorber to your CNS. It also carries different proteins and infection fighting immune cells such as lymphocytes to protect your brain and spinal cord. CSF can also help drain any extra fluid you may have in your brain or around your spinal cord to prevent swelling in those areas.
The CSF sample will then be sent to pathology and checked for any signs of lymphoma.
Bone marrow biopsy
- Bone marrow aspirate (BMA): this test takes a small amount of the liquid found in the bone marrow space.
- Bone marrow aspirate trephine (BMAT): this test takes a small sample of the bone marrow tissue.
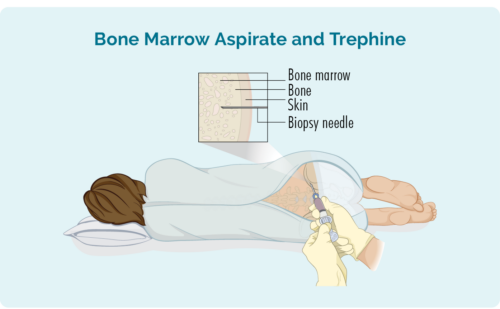
The samples are then sent to pathology where they are checked for signs of lymphoma.
The process for bone marrow biopsies can differ depending on where you are having your treatment, but will usually include a local anaesthetic to numb the area.
In some hospitals, you may be given light sedation which helps you to relax and can stop you from remembering the procedure. However many people do not need this and may instead have a “green whistle” to suck on. This green whistle has a pain killing medication in it (called Penthrox or methoxyflurane), that you use as needed throughout the procedure.
Make sure you ask your doctor what is available to make you more comfortable during the procedure, and talk to them about what you think will be the best option for you.
More information on bone marrow biopsies can be found at our webpage here.
Your lymphoma cells have a different growth pattern, and look different to normal cells. The grade of your lymphoma is how quickly your lymphoma cells are growing – whether it’s indolent or aggressive. The more aggressive your AITL is, the more different they will look to normal cells.
The grades are Grades 1-4 (low, intermediate, high). If you have a higher grade lymphoma (more aggressive), your lymphoma cells will look the most different from normal cells, because they are growing too quickly to develop properly. An overview of the grades is below.
- G1 – low grade – your cells look close to normal, and they grow and spread slowly.
- G2 – intermediate grade – your cells are starting to look different but some normal cells exist, and they grow and spread at a moderate rate.
- G3 – high grade – your cells look fairly different with a few normal cells, and they grow and spread faster.
- G4 – high grade – your cells look most different to normal, and they grow and spread the fastest.
All this information adds to the whole picture your doctor builds to help decide the best type of the treatment for you.
It is important that you talk to your doctor about your own risk factors so you can have clear idea of what to expect from your treatments.
Treatment for Angioimmunoblastic Lymphoma (AITL)
Once all of the results from the biopsy and the staging scans have been completed, your doctor will review them to decide the best possible treatment for you.
Doctors take into consideration many factors about the lymphoma and the patient’s general health to decide when and what treatment is required. This is based on:
- What subtype and stage of AITL you have.
- Any symptoms you are getting.
- How your body is being affected by the lymphoma.
- Your age.
- Your general health and wellbeing and any other conditions you are having treatment for.
- Your preferences for treatment once you have all the information needed to make an informed choice.
First-line treatment
The first time you start treatment for AITL it is called first-line treatment. Click on the headings below to learn more about the treatment protocols.
The standard first-line treatment for AITL may include:
- BV-CHP – This protocol includes the antibody conjugate Brentuximab vedotin, a steroid called prednisolone and 2 chemotherapies called doxorubicin and cyclophosphamide. You may have up to 8 cycles with each cycle being 21 days (3 weeks) long. You will have the steroid as a tablet on the first 5 days of every cycle, and you will have the brentuximab vedotin and both chemo’s on day 1 of each cycle.
- CHOP – This protocol includes 3 chemotherapies – cyclophosphamide, doxorubicin, vincristine and a steroid called prednisolone. You may have up to 8 cycles of this treatment. Each cycle will either last 2 weeks (CHOP 14) or 3 weeks (CHOP 21) long. You will have the steroid on the first 5 days of each cycle and all the chemotherapy on day 1. If you have CHOP 14, you will also have a pegfilgrastim injection on the 4th day of each cycle. This is a growth factor and will help your white cells recover quicker in time for the next cycle.
- CHOEP – this is the same as CHOP but includes a 3rd chemo called etoposide that you will have from days 1 to 3. Like CHOP, you may have this every 14 days or every 21 days.
- High-dose chemotherapy followed by autologous stem cell transplant (ASCT)
- Clinical trial participation
Second-line and other treatments
Many people have a good response from first-line treatment and will go into remission. This where there is no detectable sign of lymphoma left in your body. But it is common for the AITL to come back after a time in remission, this is called a relapse.
In some cases, your AITL may not improve with the first-line treatment. If this happens, your AITL is said to be refractory (or not responding) to treatment.
If you have refractory AITL or have relapsed, you will need to start a different treatment. This next treatment is called second-line treatment.
Standard second-line treatments can include any of the above first-line treatments or:
- Brentuximab vedotin – antibody conjugate. You may have this on its own if you have the CD30 protein on your lymphoma cells. You can have up to 16 cycles, with each cycle being 21 days (3 weeks) long. You will have the brentuximab vedotin on the first day of each cycle.
- Romidepsin – chemotherapy – this medicine is registered with the Therapeutic Goods Administration (TGA), making it available in Australia, but not listed on the Pharmaceutical Benefits Scheme (PBS). This means it may be expensive to access. Learn about alternative access to treatments not registered with the TGA or listed on PBS by watching the video below.
- Pralatrexate – chemotherapy. You will have this treatment once a week for 6 weeks. You will then have a 1 week break, and have the next treatment 2 weeks after the 6th treatment. You will then start the weekly treatments for another 6 weeks have a 1 week break and start again. You can stay on this medicine with these cycles for as long as the treatment is working and any side-effects are manageable. You will also have another medicine called leucovorin (folic acid) on the 2 days after you have the pralatrexate. This helps to reduce severe side-effects.
- GDP – includes a steroid dexamethasone, and 2 chemo’s – gemcitabine and cisplatin. You can have up 6 cycles of this treatment with each cycle being 21 days (3 weeks) long. You will have the steroid on the first 4 days of every treatment, both chemo’s on day 1 and only the gemcitabine on day 8. You may be offered this treatment if your treatment plan is to go on to have a stem cell transplant.
- High-dose chemotherapy followed by allogeneic stem cell transplant
- Radiotherapy
- Clinical trials.
Video - Alternative access to medicine
Common Side-effects of Treatment
There are many different side effects of the treatment and these are dependent on the treatment that has been given. The treating doctor and/or cancer nurse can explain the specific side effects prior to the treatment. Some of the more common side effects of treatment may include:
- Anaemia (low red blood cells carry oxygen around the body)
- Thrombocytopenia (low platelets that help bleeding and clotting)
- Neutropenia (low white blood cells help with immunity)
- Nausea and vomiting
- Bowel problems such as constipation or diarrhea
- Fatigue – tiredness or lack of energy that does not improve with rest or sleep.

What is the prognosis of AITL?
The prognosis of a disease refers to how it is likely to progress, and how it is likely to respond to treatment.
In most cases you will need to start treatment very soon after you get diagnosed with AITL. This is because it usually an aggressive subtype of lymphoma that will spread quickly and cause you to become very unwell without treatment. In very rare cases, if your AITL is an indolent subtype, you may not need start treatment straight away.
There are individual and disease related factors that can impact prognosis.
Individual factors | Disease related factors |
Age Overall health & well being Other illnesses or medication needed Ability to tolerate treatment Personal preferences about treatment | Subtype of AITL Stage & grade of AITL Genetic mutations Response to treatment How many times (or lines) of treatment you have had in the past |
What happens after treatment?
Your doctor will want to still see you regularly after your treatment ends to monitor your progress and make sure you have no signs of relapse, or late effects.
Late Effects
Sometimes a side effect from treatment may continue or develop months or years after treatment has completed. This is called a late effect. Your doctor will continue to monitor you after you finish treatment to pick up any late effects early so they can be managed appropriately. The type of late effects you get will depend on the type of treatment you had.
Make sure you ask your doctor what late-effects to expect and when and how you should report to them.
Living well
A healthy lifestyle, or some positive lifestyle changes after treatment can be a great help to your recovery. There are many things you can do to help you live well with AITL.
Many people find that after a cancer diagnosis, or treatment, that their goals and priorities in life change. Getting to know what your ‘new normal’ is can take time and be frustrating. Expectations of your family and friends may be different to yours. You may feel isolated, fatigued or any number of different emotions that can change each day.
Goals after treatment
The main goals after treatment for your AITL is to get back to life and:
- be as active as possible in your work, family, and other life roles
- lessen the side effects and symptoms of the cancer and its treatment
- identify and manage any late side effects
- help keep you as independent as possible
- improve your quality of life and maintain good mental health.
Cancer Rehabilitation
Different types of cancer rehabilitation may be recommended to you. This could mean any of a wide range of services such as:
- physical therapy, pain management
- nutritional and exercise planning
- emotional, career and financial counselling.
Summary
- Angioimmunoblastic T-cell Lymphoma (AITL) is subtype of Peripheral T-cell Lymphoma – a type of Non-Hodgkin Lymphoma.
- AITL means the cancer arises from immature immune cells (T-cells) with abnormal blood vessels at the site of the lymphoma.
- AITL is usually aggressive and needs treatment very soon after diagnosis.
- Treatment may include chemotherapy, radiotherapy, immune therapies, targeted therapies or stem cell transplants.
- You may have a good response to your treatment, but it is not uncommon for AITL to relapse and need more treatment.
- Report all symptoms, including B-symptoms to your doctor.
- Ask your doctor about what to expect from your treatment.
- Reach out to our Lymphoma Care Nurses if you would like to chat about your lymphoma or the treatments for it – Click on the Contact Us button at the bottom of the screen for details.