Overview of MEITL
MEITL was formerly known as Enteropathy Type Intestinal T-cell Lymphoma Type 2. However, it has been reclassified by the World Health Organisation (WHO) as we learn more about it. The change in classification came in 2017 and is because we now know that, unlike Enteropathy Type Intestinal T-cell Lymphoma Type 1 (now known as EATL), MEITL is not associated with previous intestinal disorders such as coeliac disease.
What is MEITL?
MEITL is a very rare, and an aggressive type of cancer of white blood cells called T-cell lymphocytes. The T-cells that are in the lining of your intestines (bowel) and parts of your gastrointestinal tract are called epithelial T-cells. This is where the name Monomorphic Epitheliotropic Intestinal T-cell Lymphoma comes from.
About T-cell lymphocytes
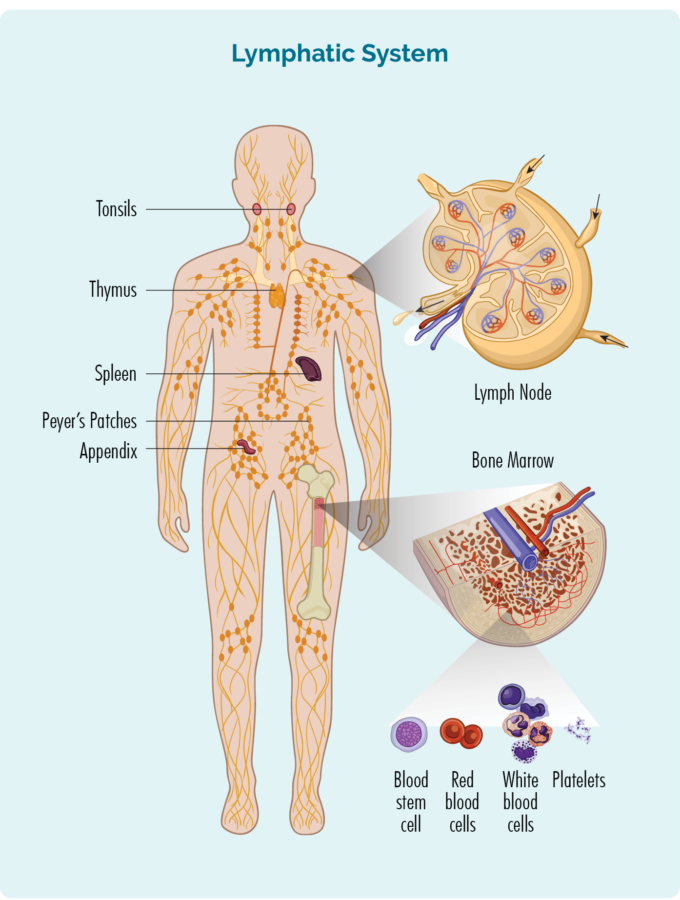
T-cell lymphocytes are specialised white blood cells that support our immune system by fighting infection and disease.
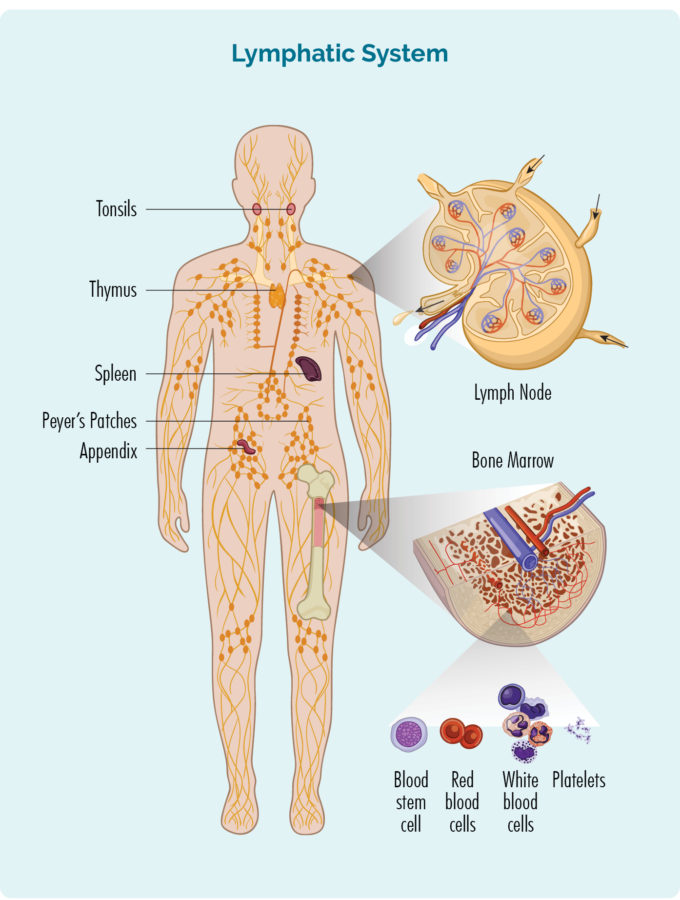
Unlike other blood cells, T-cell lymphocytes do not usually live in our blood, but instead are found in our lymphatic system. However, because their job is to fight infection and disease, they can travel to any part of our body including our blood, skin, stomach, organs and brain.
Some collections of T-cell lymphocytes are also found in our gastrointestinal tract which includes our mouth, stomach and bowels (intestines). MEITL begins when the T-cell lymphocytes in your bowels become cancerous.
Who gets MEITL
Intestinal T-cell Lymphomas are rare, and MEITL is one of the rarer ones. It is more common in people with either Asian or Hispanic background.
Cytogenetics and MEITL
People with certain genetic mutations may also be at increased risk of developing MEITL.
Cytogenetic tests are done to check for genetic variances that may be involved in your disease. For more information on these please see our section on understanding your lymphoma genetics further down on this page. The tests used to check for any genetic mutations are called cytogenetic tests. These tests look to see if you have any changed in chromosomes and genes.
We usually have 23 pairs of chromosomes, and they are numbered according to their size. If you have MEITL, your chromosomes may look a little different.
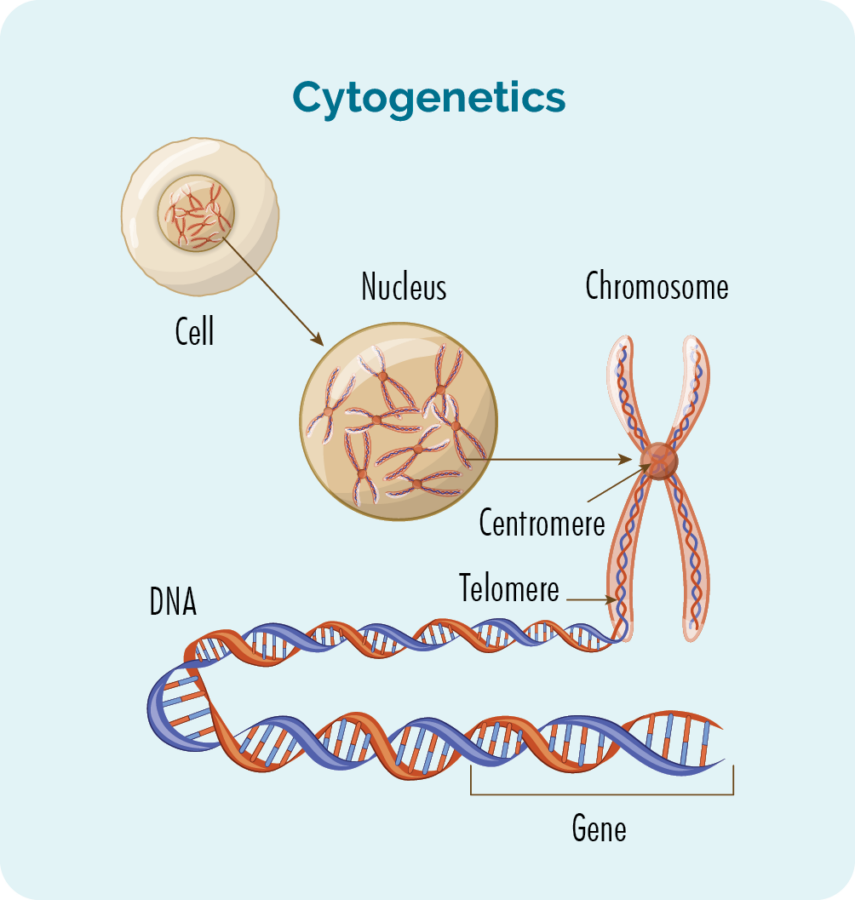
What are genes and chromosomes
Each cell that makes up our body has a nucleus, and inside the nucleus are the 23 pairs of chromosomes. Each chromosome is made from long strands of DNA (deoxyribonucleic acid) that contain our genes. Our genes provide the code needed to make all the cells and proteins in our body, and tells them how to look or act.
Common cytogenetic changes in people with MEITL
There are many different cytogenetic changes that can happen in people with lymphoma. Some of the common ones seen in people with MEITL includes mutations to tumour suppressor genes.
Tumour suppressor genes are genes that instruct the immune system to recognise and destroy cancerous cells. However, when there is a mutations in the tumour suppressor gene, your immune system does not get the right instructions, and so instead of recognising and destroying the lymphoma, it lets the cancer continue to grow and multiply.
This can happen if you have a mutation in a gene called SETD2 or if you have a part of one of your chromosomes (3p21) is missing.
Other changes that can happen that can result in MEITL developing is a mutation in the JAK-STAT pathway. This pathway is communication network between some of your proteins that also provide information to your immune system on how to regulate your cells and destroy cancerous ones. When there is a change to how these proteins communicate with each other, MEITL can grow.
Symptoms of MEITL
Some symptoms of lymphoma are common in all people with any type of lymphoma, and some are related to the type and location of lymphoma you have. If you experience any of the below symptoms see your doctor for a check up.
Symptoms of MEITL
- abdominal pain or cramps (tummy ache)
- diarrhea (runny poo)
- unusual bleeding when you go to the toilet
- an obstruction in your bowels which can cause pain, swelling, difficulty with passing wind and/or poo, bleeding, nausea and vomiting
- loss of appetite and/or weight loss
- skin rash with itchy blisters or raised patches.
- B-symptoms (see picture).
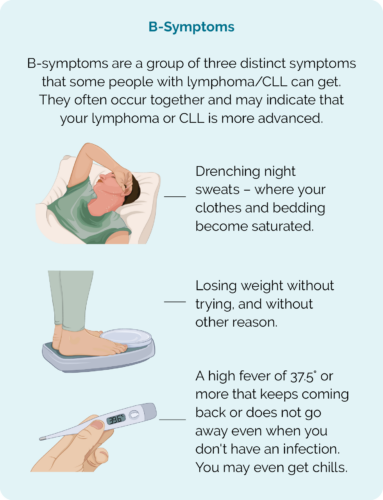
General symptoms of lymphoma
- fatigue
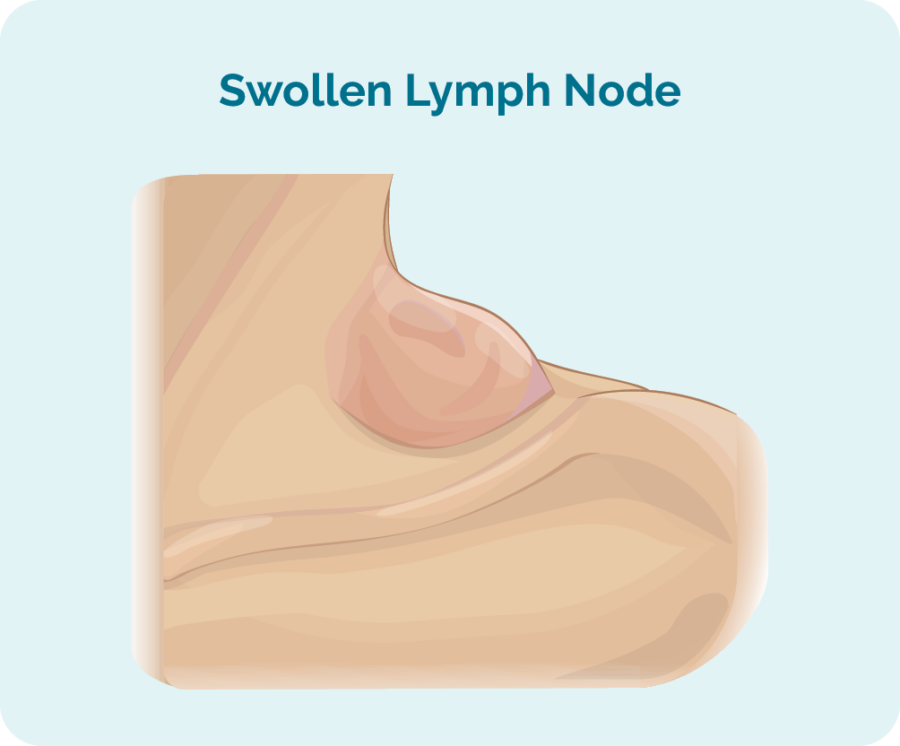
- swollen lymph nodes (a lump that comes up under your skin, usually in your neck, armpit or groin)
- an enlarged spleen or liver
- bleeding and bruising more than usual
- infections that don’t go away or keep coming back.
How is MEITL diagnosed?
Because MEITL is an aggressive type of lymphoma, you will likely have symptoms for less than 3 months before getting diagnosed. Though for some people it can take longer. It is important to openly discuss any symptoms you have with your doctor so they can plan the right tests for you.
Your doctor will likely start with some blood tests and a stool sample (sample of your poo), to rule out other causes such as infection or allergies.
Changes to your blood tests
If you have MEITL some changes in your blood tests may include:
- high lactate dehydrogenase (LDH) level
- low albumin
- low red blood cells or haemoglobin (anaemia).
There are other reasons that can cause similar changes in your blood tests, so it is important to talk to your doctor about all of your results.
Scans and Tests
There are many different tests and scans your doctor might recommend for you to help diagnose, or stage your MEITL.
- Endoscopy (or capsule endoscopy where you swallow a tiny capsule type of camera which takes pictures of the inside of your stomach and bowels)
- Bone marrow biopsy
- Computed tomography (CT) scan
- Magnetic resonance imaging (MRI) scan
- Positron Emission Tomography (PET) scan
- Tests on your heart, liver and kidneys (to make sure they are strong enough to cope with the chosen treatment)
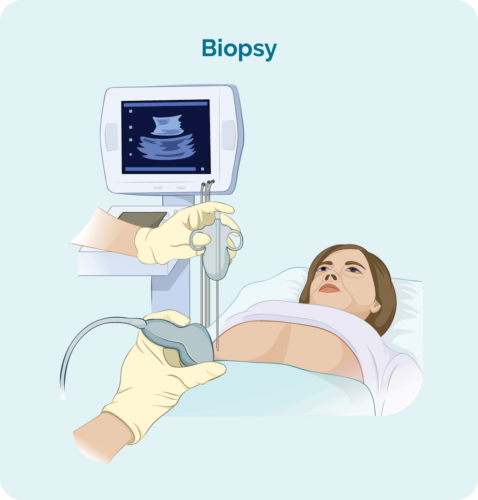
- Biopsy
Treatment for MEITL
Because MEITL is so rare, there are no steadfast treatment options. However, treatments are based on treatments that have been the most effective in other T-cell lymphomas, or in people with lymphoma that have similar genetic mutations. With more clinical trials, we hope that new and effective treatment options will be identified to standardise the treatment for people with MEITL.
Before treatment starts you will need to be well enough to tolerate the toxic treatments. This can sometimes make it difficult to start, as most people with MEITL are quite unwell when first diagnosed. But your doctor will work with you, and keep a close on you to make sure your body can tolerate the treatment.
First-line treatment
The first time you start treatment it is called first-line treatment. Chemotherapy is the most common type of treatment you would have, and it is often followed by an autologous stem cell transplant.
Common chemotherapy protocols you may be offered are:
- CHOP – a combination of 3 chemotherapy medications called cyclophosphamide, doxorubicin and vincristine, as well as a steroid called prednisolone.
- CHEOP – the same as medication as CHOP with an extra chemotherapy called etoposide.

Second-line treatment
If you have a refractory lymphoma, or you have relapsed, you will need a second-line treatment.
Refractory Lymphoma
Remission Complete & Partial
A partial remission means you still have lymphoma in your body, but it is less than half of what you had before starting treatment.
Relapse
Treatment for Refractory or Relapsed MEITL
There are several different types of treatment your doctor may want to try if you have refractory or relapsed MEITL.
Some of the treatments include:
- High dose chemotherapy followed be stem cell transplant using your own stem cells – an autologous stem cell transplant
- High dose chemotherapy using a donor’s (somebody else’s) stem cells – an allogeneic stem cell transplant
- Different types of chemotherapy
- Romidepsin
- Brentuximab vedotin
- Pralatrexate
- Radiotherapy
- Clinical trial
Clinical Trials
It is recommended that anytime you need to start new treatments you ask your doctor about clinical trials you may be eligible for. Clinical trials are important to find new medicines, or combinations of medicines to improve treatment of MEITL in the future.
They can also offer you a chance to try a new medicine, combination of medicines or other treatments that you would not be able to get outside of the trial. If you are interested in participating in a clinical trial, ask your doctor what clinical trials you are eligible for.
There are many treatments and new treatment combinations that are currently being tested in clinical trials around the world for patients with both newly diagnosed and relapsed MEITL.
Common side-effects of treatment
Side effects of treatment will depend on the type of treatment you are having. Your haematologist or specialist cancer nurse will be able to talk to you about what to expect from your treatment and how to mange your symptoms, however some of the more common side-effects include:
Hair loss, including hair on your head as well as all the hair on your body.
Changes to your bowel motions, including diarrhoea or constipation.
Mouth ulcers, pain or changes to the way things taste.
Fatigue, which is extreme tiredness not improved with rest or sleep.
Low blood counts including low haemoglobin, low platelets and low white cells.
Changes to sensation including numbness, pins & needles, tingling, pain (peripheral neuropathy)
What to expect when treatment finishes
When you finish your treatment your haematologist will still want to see you regularly. You will have regular check-ups including blood tests and scans. How often you have these tests will depend on your individual circumstance and your haematologist will be able to tell you how often they want to see you.
It can be an exciting time or a stressful time when you finish treatment – sometimes both. There is no right or wrong way to feel. But it is important to talk about your feelings and what you need with your loved ones.
Support is available if you are having a difficult time coping with the end of treatment. Talk to your treating team – your haematologist or specialist cancer nurse as they may be able to refer you for counselling services within the hospital. Your local doctor (general practitioner – GP) can also help with this.
Lymphoma Care Nurses
You can also give one of our Lymphoma Care Nurses or email. Just click on the “Contact Us” button at the bottom of the screen for contact details.
Summary
- MEITL is a rare and aggressive cancer of your white blood cells called T-cell lymphocytes.
- MEITL usually starts in your small bowel, but can spread to other parts of your body.
- Symptoms of MEITL can include pain or cramps in your tummy, diarrhoea or difficulty passing wind or stool, bleeding when you go to the toilet, loss of appetite and weight loss as well as B-symptoms.
- You will need several different types of tests and scans to diagnose and stage MEITL.
- Treatment will usually include chemotherapy and a possible stem cell transplant.
- You may need more than one type of treatment.
- You are not alone, talk to your treating team if you need extra support, or give our Lymphoma Care Nurses a call.