It can sometimes take a while and many tests to be diagnosed with lymphoma. This is because the symptoms of lymphoma are often very similar to symptoms of other, more common illnesses, so your doctor may test you for these other illnesses first. If your symptoms continue, they may decide to test for lymphoma. Tests for lymphoma may be done by your local doctor but often, if they suspect you may have lymphoma, they will refer you to specialist doctor called a haematologist or oncologist for more tests.
You will need a biopsy to diagnose lymphoma, and if you have lymphoma you will need more tests to check the stage and grade of your lymphoma. This page will go through the different types of tests and biopsies used to diagnose lymphoma, scans used to stage lymphoma and other types of tests you may need.
What is Diagnosis, Staging and Grading?
Diagnosis
Staging
Grading
How is lymphoma diagnosed?
To diagnose lymphoma, you will need a biopsy of the area of your body affected. This may mean a you need biopsy of your lymph node, skin, fluid around your spine or bone marrow. In some cases you may need a biopsy of the tissue in your lung, stomach or bowels.
You will not need all these tests. Your doctor will work out the best biopsy based on your individual situation. Click on the headings below to learn about different types of lymph node biopsy.
Types of biopsies
You will have a local anaesthetic to numb the area of your biopsy, and in some cases you may also have general anaesthetic. This will depend on the location of the lymph node or tissue to be biopsied, and how easy it is for the doctor to get to it.
Children will almost always have a general anaesthetic so they sleep through the biopsy. This helps to stop them from becoming distressed, and ensures they stay still during the procedure.
An excisional biopsy is a biopsy that is done during a minor surgical operation. It is the most effective way of diagnosing lymphoma in the lymph node because the whole lymph node is removed and examined in pathology.
When the lymph node to be removed is close to your skin, you may have this procedure done while you are awake. You will have a local anaesthetic to numb the area so you shouldn’t feel pain. You might have some stitches after the procedure that will be covered with a small dressing. Your doctor or nurse will be able to tell you when to get the stitches out and how to manage your dressing to avoid infection.
What if the lymph node is deep inside my body?
If the lymph node is deeper inside your body, you may have a general anaesthetic so you will be asleep during the procedure. You will likely have stitches and a small dressing over them when you wake up. Your doctor or nurse will talk to you about how manage the dressing and when you need to get the stitches removed.
In some cases there can be a delay in getting an excisional biopsy, because it requires surgery, and there can be wait list to get in.
An incisional biopsy is similar to an excisional biopsy, but instead of removing the entire lymph node, only part of the lymph node is removed.
This may be done if the lymph node is particularly large, or your lymph nodes are matted – meaning they have fused together with other lymph nodes. In some cases there can be a delay in getting an excisional biopsy, because it requires surgery, and there can be wait lists.
A core biopsy is used to take a small sample of the lymph node or affected skin if you have a suspicious rash or lump. They are sometimes also called a needle biopsy. It is usually done with a local anaesthetic, and depending on where it is, the doctor may use an ultrasound or CT scan to help guide the needle into the right place.
Because the sample is taken with a hollow needle, the sample is much smaller than an excisional or incisional biopsy. This means that sometimes the cancerous cells may not be picked up in the sample, resulting in lymphoma being missed. But core biopsies can be useful when there is a long delay for an excisional or incisional biopsy. You may need more that one core biopsy to diagnose lymphoma.
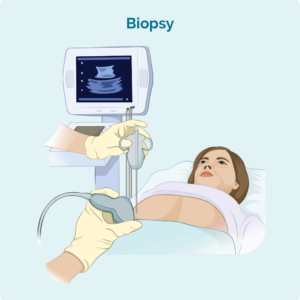
A fine needle biopsy uses a smaller needle that what is used for a core biopsy. It is usually not recommended to diagnose lymphoma because it does not provide a big enough sample to get a reliable result.
However sometimes, a fine needle biopsy may be done to check for other things, and it may pick up lymphoma cells. You will be referred for other tests if it looks like there are lymphoma cells in your biopsy.
While most doctors call you if there is something worrying in your test results, not all do. And rarely, results can get lost or missed. Always make a follow up appointment with your doctor to get results of bloods tests, scans and biopsies.
When to contact your doctor
Contact your doctor or nurse for advice if you get any of the following symptoms:
- Signs of infection including temperature of 38º or more, chills and shakes, puss or unusual discharge from the wound.
- Bleeding that doesn’t stop after putting a cold pack (or frozen peas) over the site, or that fills the whole dressing.
- Pain that does not improve with paracetamol (also known as Panadol, Panamax or Dymadon).
What is a Bone Marrow Biopsy?
A bone marrow biopsy is a procedure done to remove a sample of your bone marrow from inside your bone. It is usually taken from the hip bone, but in some cases can be taken from other bones. This biopsy can be used to help diagnosed some subtypes of lymphoma, and is used to stage other subtypes.
What is a Lumbar puncture?
You may be advised to have a lumbar puncture (LP) if there is a chance you have lymphoma in your central nervous system (CNS), which includes your brain, spinal cord and area behind your eyes.
During an LP, you will lie on your side and the doctor will give you an injection of local anaesthetic into your back. This will numb the area so you shouldn’t feel any pain with the procedure (though the local anaesthetic can sting for a short time).
Once the area is numb, the doctor will put a needle ionto your back, between the bones in your back (vertebrae) and into the area where the cerebral spinal fluid (CSF) is. They will then remove small sample of the fluid to test for lymphoma.
You will have a small dressing over the area the needle went in and you may need to lay flat for 1-4 hours. Your nurses will let you know how long you will need to lay for.
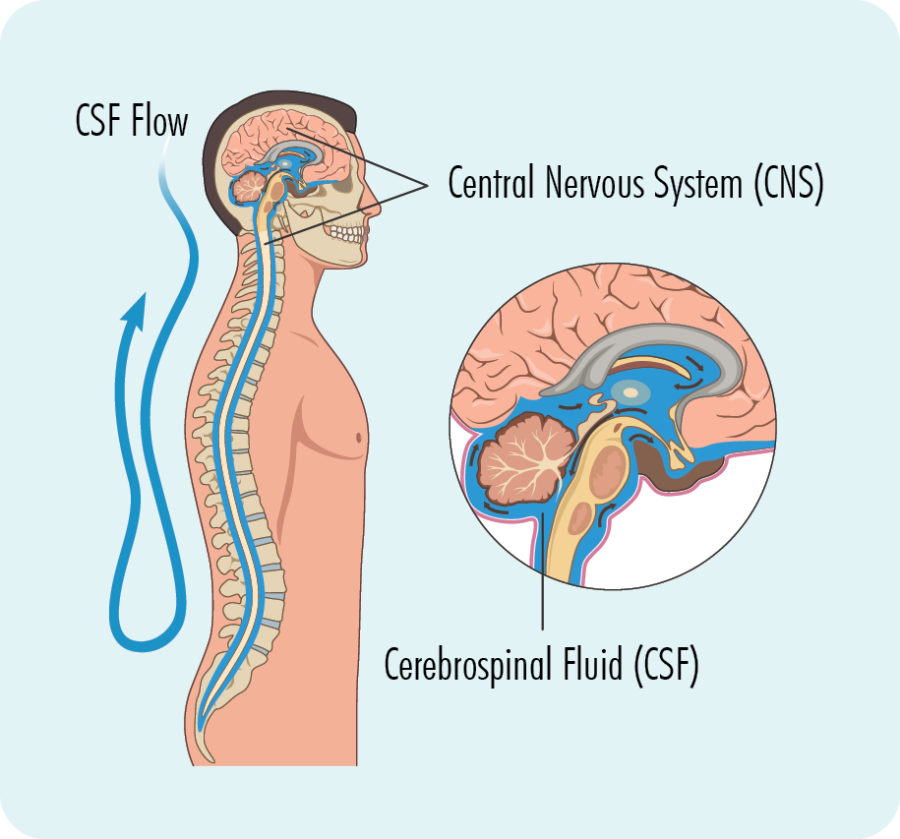
What else is a lumbar puncture used for?
In some cases where you have lymphoma in your CNS, or have a chance that it will spread there, a lumbar puncture is also done to deliver chemotherapy straight into your CSF. When this is done, it is called “intrathecal (IT) chemotherapy”.
What is an Endoscopy
An endoscopy is a procedure used if the doctor thinks you may have lymphoma in your gastrointestinal (GI) tract. Your GI tract includes your:
- mouth
- oesophagus (which is the pipe food goes down from your mouth to your stomach)
- stomach
- small intestines (bowel)
- large intestines
During an endoscopy the radiologist or surgeon inserts a thin tube into your mouth and feeds it through to your oesophagus (pipe that carries food from your mouth to your stomach), stomach and small bowel. This allows them to look at your gastrointestinal tract for signs of lymphoma. They can also take a small biopsy sample during an endoscopy to send to pathology.
This will be done with a sedative and anaesthetic so you should not feel any pain or even remember procedure. In some cases you may have a general anaesthetic so you will sleep through the endoscopy.
What scans do I need?
There are several types of scans that are useful to help diagnose or stage lymphoma, and track how your lymphoma is responding to treatment. Before having any scan, please let the radiographers know if you:
- are, or could be pregnant, or if you are breastfeeding.
- have a fear of enclosed spaces (claustrophobia).
- have difficulty laying or standing in certain positions.
- have any pain or nausea.
- have any allergies.
To learn more about the different types of scans and why they might be used, click on the headings below.
An ultrasound is a scan that uses sound waves to make a picture. The ultrasonographer (person doing the ultrasound) will put some gel over the area being checked, and use a wand-like device to run over your skin, which sends sound waves into your body. As the waves bounce back it creates a picture of the inside of your body.
Ultrasounds are often used to help find swollen lymph nodes so the doctor can take a biopsy. It can also be used to help find good veins or look at organs in your body.
Depending on what part of your body is being checked, you may need to drink water and have a full bladder for the ultrasound.
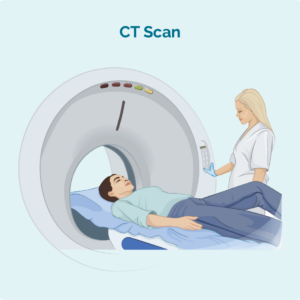 A CT scan is a scan that can look at the inside of your body and give a 3D image. It is usually used when only a certain part of your body needs to be seen, such as your chest or abdomen. They can provide an image of your body from front to back and top to bottom. Scans are often used to check for tumours, swollen lymph nodes and other conditions.
A CT scan is a scan that can look at the inside of your body and give a 3D image. It is usually used when only a certain part of your body needs to be seen, such as your chest or abdomen. They can provide an image of your body from front to back and top to bottom. Scans are often used to check for tumours, swollen lymph nodes and other conditions.
You may need to have an injection with a fluid called contrast, that helps make clearer pictures. Contrast is injected quickly, and has a strange side effect of making you feel like you have wet your pants. It can feel very warm and be unnerving, but does not last long.
You will lay on a bed that moves in and out of the CT machine. It is very quick and usually only takes about 10-15 minutes.
MRI scans use magnets and radio waves to create an picture of the inside of your body. It is similar to a CT scan in that you will lay on a bed and be moved in and out of the MRI machine. However, MRI scans can take longer, and depending on what part of your body is being scanned, can take 15 – 90 minutes (1 and half hours). It is also a very noisy scan as the magnets move around inside the machine.
If you have trouble with loud noises, or in enclosed spaces, please let the nurses know before your scan so they can make you more comfortable. They often have headphones so you can listen to music, or you may need some anti-anxiety medicine to help you feel calm – however, many people do not need this.
If you have lymphoma in your brain or spinal cord, you will likely have an MRI scan, but you can also have an MRI for other reasons too when your doctor wants to look at different parts of your body.
Images from an MRI look like the below picture.
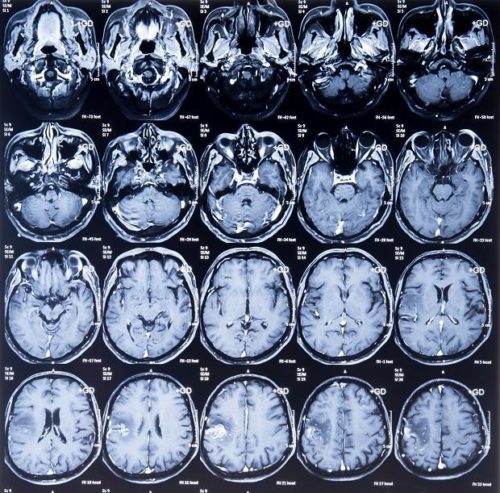
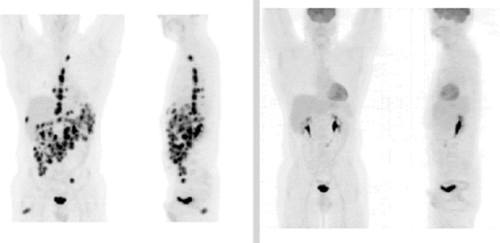
PET scans provide an image of the inside of your whole body, and lights up areas that are affected by lymphoma. You will be given an injection of a radioactive medicine that any cancerous cells absorb, making them stand out on the PET scan. It takes around 30-60 minutes to do, but you should allow at least 2 hours for the appointment over all.
You will need to lay and will have special rests for your arms and legs to make sure you they can get best pictures. If you have trouble staying in a position for a long time, please let the staff know so they can make sure you as comfortable as possible.
You may be asked to avoid some foods and drinks in the days leading up to your PET scan. If you have not been given instructions, please call the nuclear medicine department where you are having your PET scan for advice.
Because of the radioactive medicine you will be given, you will need to avoid being around pregnant women or young children for up to one full day (24 hours).
Blood tests
You will likely have several blood tests while going through testing for a diagnosis of lymphoma. If you have lymphoma and are having treatment, you will also have blood tests throughout your treatment. Some of the more common blood tests used when you have lymphoma are listed below. However, the blood tests you have will depend on your individual situation.
Full Blood Count
This is one of the most common blood tests you will have. It tells the doctors about the numbers, types, shape and sizes of cells in your blood. The different cells that are looked at in this test are;
- Red Blood Cells (RBCs) these cells carry oxygen around your body.
- White Blood Cells (WBCs) are an important part of our immune system and help keep us healthy be fighting infection and disease. There are different types of WBCs (neutrophils, eosinophils, basophils and others). Each cell has a specific role in fighting infection. Lymphocytes are also white blood cells, but only small numbers are usually found in your blood, as they live mostly in your lymphatic system.
- Platelets help your blood to clot, preventing bruising and bleeding.
Blood group and crossmatch
You will have this if you need a blood transfusion, to make sure they get the right blood for you.
Liver function tests (LFTs)
Are used to see how well your liver is working.
Kidney function tests
Are used to check how well your kidneys are working.
Lactate dehydrogenase (LDH)
LDH checks for tissue cell damage in your body.
C-Reactive Protein (CRP)
CRP is used to check for signs of inflammation in your body.
Erythrocyte sedimentation rate (ESR)
ESR also checks for signs of inflammation in your body.
Plasma Viscosity (PV)
PV refers to the thickness of your blood. This is an important test to have if you have a subtype of lymphoma called Waldenstrom’s macroglobulinemia.
Serum protein electrophoresis (SPEP)
SPEP measures abnormal proteins in your blood if you have a subtype of lymphoma called Waldenstrom’s macroglobulinemia.
International normalised ratio (INR) and Prothrombin Time (PT)
INR and PT tests measure how long it takes for your blood to begin to form clots. You may have this done before a surgical procedure, lumbar punctures or bone marrow biopsies.
Screening for exposure to viruses
These are tested as some lymphomas are more common in people with certain viruses. If you have these viruses, your doctor will need to consider these when choosing the right treatment plan for you. Some viruses that you may be screened for include;
- Human immunodeficiency virus (HIV)
- Hepatitis B and C
- Cytomegalovirus (CMV)
- Epstein Barr virus (EBV).
The medical team might suggest other blood tests depending on the individual circumstances.
Before you start treatment, your doctor will also want to do more tests to make sure your body is able to tolerate the planned treatment. You can learn more about the different baseline tests and organ function tests by clicking the link below.
What are Cytogenetic tests?
Some poeple with lymphoma have changes in their DNA and genes. These changes are important because they can give information about what the best type of treatment for you will be. You may be offered several types of tests that check the DNA and genes on your lymphoma cells, or that check for different proteins found on your lymphoma cells.
It can take several weeks to get these test results back.
To learn more about these tests, click the link below.
Waiting for results
You will not get any results, when you have a scan or other test. A report will be written up and sent to your doctor, and can take up to a week.
Ask when your doctor will have the reports so you can make an appointment to get your results. Your doctor may want to wait until they have all the results of your tests before they see you so they can give you the best information. This is because each test only gives one part of the picture, and your doctor will need all your results to make a proper diagnosis, and decide on the best types of treatment – if you need to have treatment.
It can be a stressful time waiting for results. It is good to talk to your family and friends about how you are feeling. You can also reach out to our Lymphoma Care Nurses by clicking on the Contact Us button at the bottom of this page.
Summary
- There are many different tests you will need to get a diagnosis of lymphoma, find out your subtype, stage your lymphoma and during your treatment for lymphoma.
- Tests can include blood tests, biopsies, scans and cytogenetic tests.
- It can take several weeks to get all your results, but it is important for your doctor to have all the information before they can give you a diagnosis, or make a treatment plan for you.
- If you are struggling while waiting for test results you can contact Lymphoma Australia nurses by clicking the Contact us button at the bottom of the page.

