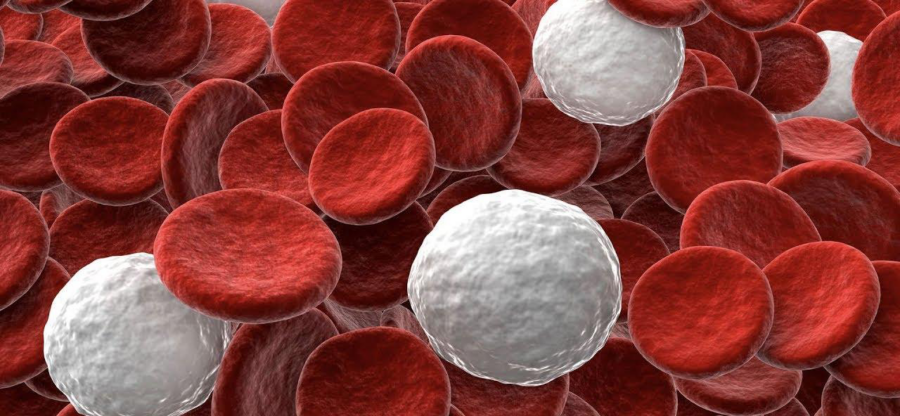
Our blood is made up of a fluid called plasma, red blood cells, white blood cells and platelets. Our white blood cells are part of our immune system and fight infection and disease.
We have different types of white blood cells, each responsible for fighting different types of infections. Neutrophils are the white blood cells we have the most of. They are the first to recognise and fight infections.
Neutropenia is a medical term used when you do not have enough neutrophils - putting you at risk of infection.
What you need to know about neutrophils
Neutrophils make up the majority of our white blood cells. A little over half of all our white blood cells are neutrophils.
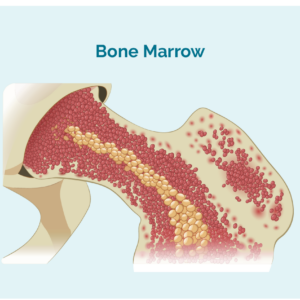
Neutrophils are made in our bone marrow – the spongey middle part of our bones. They spend about 14 days in our bone marrow before being released into our bloodstream.
They can move out of our bloodstream if they need to fight infection in a different part of our body.
Neutrophils are the first cells that recognise and fight germs, infection and disease.
Germs, infection and disease are pathogens. Pathogens are anything not part of us, that has the potential to make us sick. A pathogen may also be one of our own cells that has developed in a way that is harmful to us, such as a cell that has become cancerous.
Neutrophil levels in our blood can fluctuate (change) throughout the day as new ones are made and others die off.
Our body makes about 100 billion neutrophils every day! (That’s about 1 million every second). But each one only lives for 8-10 hours once it enters our blood stream. Some may live for up to a day.
Unlike other white blood cells that fight specific pathogens, neutrophils are non-specific. This means they can fight any pathogen. However, on their own they cannot always eliminate the pathogen.
Neutrophils produce chemicals called cytokines when they fight pathogens. These cytokines send messages to other white blood cells, to let them know there is a pathogen that needs to be eliminated. The more specific white blood cells designed to fight that specific pathogen then springs into action and eliminates it.
Our bodies come into contact with pathogens all the time! Our neutrophils are the reason we don’t get sick all the time.
Our neutrophils activate our immune system to eliminate the pathogen, often even before they have the chance to make us sick.
This page is focusing on neutropenia – low neutrophils leves. However, you may sometimes have high neutrophil levels which you may have questions about. High neutrophils can be caused by:
- steroids (such as dexamethasone or prednisolone)
- growth factor medicine (such as GCSF, filgrastim, pegfilgrastim)
- infection
- inflammation
- diseases like leukemia.
Your normal level of neutrophils is dependent on several factors. These can include:
- your age (babies, children, teenagers, adults, and older adults will have different “normal” levels).
- treatments you are having – some medicines will cause higher levels, and others may cause lower levels.
- whether you are fighting an infection or inflammation.
- the equipment used in pathology and reporting methods.
You have the right to ask for a printed copy of your blood results. In most cases, the report will show your level of neutrophils and then in brackets (….) show the normal range. This will help you work out if your results are normal or not. However, you will need your doctor to explain these to you, because the pathologist reporting does not know your individual circumstances. Your doctor will be able to let you know if the levels are normal for your individual situation.
You may notice that the result does not appear within normal limits. This can cause anxiety and worry – and then be confusing when your doctor does not seem worried. It’s important to remember that your blood test is only one small piece of a much bigger puzzle that is YOU. Your doctor will look at your blood tests along with all the other information they have about you, before making decisions about whether the blood test is something to worry about.
Ask your doctor to explain your results with you, based on your individual clinical circumstances.
What you need to know about Neutropenia
Neutropenia is a very common side-effect of lymphoma treatments. Many treatments work by attacking fast growing cells. Remember we said above, our body makes 100 billion neutrophils every day? This means they can also be targeted by the treatments that fight the lymphoma.
Neutropenia is when your neutrophils levels are too low. If you have neutropenia, you are neutropenic. Being neutropenic puts you at increased risk of infections.
Being neutropenic isn’t in itself life threatening. However, if you get an infection while neutropenic, these infections can very quickly become life-threatening. You need to get medical support immediately. More information on this is further down the page under Febrile Neutropenia.
You are most likely to be neutropenic 7-14 days after you have had chemotherapy. However, neutropenia can happen anytime during your treatments for lymphoma. If your neutrophils are too low, you may need to have your next treatment delayed until they come up to a safer level. When you are having treatment for lymphoma, a safe level for treatment may still be a level that is lower than the normal level.
Neutropenia can also be late side-effect of some monoclonal antibodies such as rituximab and obinutuzumab. Late side-effects can happen months or years after you finish treatment.
If your treatment is likely to make you neutropenic, your haematologist or oncologist might start you on some prophylactic medicine. Prophylactic means preventative. These are given even if you don’t have an infection, to try and stop you getting sick later.
Some types of medicine you might be started on include:
- Anti-fungal medicine such as fluconazole or posaconazole. These prevent or treat fungal infections such as thrush, that you can get in your mouth or genitals.
- Anti-viral medicine such as valacyclovir. These prevent a flare up or treat viral infections such as herpes simplex virus (HSV), which causes cold sores on your mouth or sores on your genitals.
- Anti-bacterial medicine such as trimethoprim. These prevent certain bacterial infections such as bacterial pneumonia.
- Growth factors to increase your white blood cells such as GCSF, pegfilgrastim or filgrastim to help your white blood cells recover quicker after chemotherapy.
I many cases neutropenia cannot be prevented during treatment. However, there are somethings you can do to lessen the impact it has on you.
- Take your prophylactic (preventative) medicines the way your doctor orders them for you.
- Socially distance. Keep 1 -1.5 meters between you and other people when you are out in public. Wear a mask if you cannot socially distance.
- Keep hand sanitiser in your bag or car, or wash your hands with soap and water. Clean hands before and after eating, or touching anything dirty or used by many people – such as shopping trolleys, light switches and door handles and after going to the toilet or changing a nappy.
- Use a good moisturiser on dry hands and skin to prevent cracks that can let germs into your body.
- If you go shopping, go at a quieter time of the day when there are less people around.
- Avoid people if they have recently had a live vaccine – such as many childhood vaccines and shingles vaccines.
- Tell friends and family not to visit if they have even any symptoms of illness such as a runny nose, cough, fevers, rash or are generally feeling unwell and fatigued. Ask visitors to wash their hands when they arrive.
- Avoid animal litter trays or waste. Wash or sanitise your hands after touching animals.
- Hold any cuts under running water for 30-60 seconds to remove any germs, use antiseptic once clean and dry, and put a band aid or other sterile dressing over the cut until healed.
- If you have a central line like a PICC, Implanted port or HICKMANS make sure any dressings are kept clean and dry, and do not lift from your skin. Report any pain or discharge to your nurse immediately. If your dressing over the central line becomes dirty, or does not stick to your skin, report to your nurse immediately.
- Eat a protein rich healthy diet. Your body needs extra energy to replace the healthy cells including neutrophils, damaged or destroyed by your treatment. Protein is needed to make these cells.
- Wash fruit and vegetable before eating or cooking. Eat only freshly prepared foods or those frozen right after cooking. Reheat so the food is hot all the way through. Avoid buffets and all you can eat restaurants.
- Eat foods with lower chance of causing infection – See table below.
Neutropenic Diet | |
Do Eat | AVOID |
Pasteurized Milk Pasteurized yoghurt Hard cheeses Hard ice-cream Jelly Fresh bread (no mouldy bits) Cereal Whole grains Chips Cooked Pasta Eggs – cooked through Meat – cooked to well done Tinned meats Water Instant or brewed coffee and tea Freshly washed fruits and vegetables. | Unpasteurized milk and yoghurt Soft cheeses and cheeses with mould (such as brie, feta, cottage, blue cheese, camembert) Soft serve ice-cream Runny eggs Egg nog or smoothies with raw eggs Undercooked meats – Meat with blood or raw sections Cold meats Smoked meats Sushi Raw fish Shellfish Dried fruits Buffets and salad bars Salads not freshly made Leftovers Apple cider Probiotics and live cultures. |
Food handling
- Always wash hands thoroughly before eating.
- Always wash hands before and after preparing food.
- Always use separate chopping boards for meat, poultry, and fish.
- Keep raw meat, seafood, and eggs away from ready to eat foods. Avoid raw and undercooked meat or poultry. Do not eat foods with raw egg in it. Do not eat smoked meats or fish.
- Discard sponges and wash dish towels regularly.
- Cook food thoroughly at proper temperatures.
- Wrap and refrigerate leftovers or freeze within one hour of preparation to limit growth of bacteria.
- Make sure honey and dairy are pasteurised. Avoid mould ripened cheeses, blue cheeses and soft cheeses.
- Do not eat foods that have passed the expiry dates.
- Do not buy or use foods in cans that are dented or damaged.
- Avoid food from deli-counters.
Infection and neutropenia
Infections can start anywhere in your body when you are neutropenic. The most common infections you can get include infections in your:
- airways – such as infuenza (Flu), colds, pneumonia and COVID
- digestive system – such as food poisoning, or other bugs that can cause diarrhea or vomiting
- bladder or urinary tract infections
- central lines or other wounds.
Being neutropenic means your body cannot fight the infection as it normally would. Many of the symptoms we get when we have an infection are from the immune response to the infection rather than the infection itself. You may not get all the same signs of infections as you normally would.
Normal signs of infection
The normal immune response to infection releases cytokines and other chemicals from our immune cells and the destroyed pathogens. This process, as well as the removal of destroyed cells is what causes many of our symptoms. Normal symptoms of this process include:
- redness and swelling.
- puss – a yellowy or white thick discharge.
- pain.
- fever (high temperature) – Normal temperature is 36 degrees to 37.2 degrees. Some fluctuations are normal. But if your temperature is 38 degrees or higher, notify your doctor or nurse immediately.
- low fever less than 35.5 degrees can also indicate infection.
- foul smell.
Febrile neutropenia
 Febrile neutropenia associated with an infection is a medical emergency. Febrile neutropenia means you are neutropenic, and have a temperature of more than 38 degrees. However, having a temperature of less then 35.5 degrees can also indicate infection and can become life-threatening.
Febrile neutropenia associated with an infection is a medical emergency. Febrile neutropenia means you are neutropenic, and have a temperature of more than 38 degrees. However, having a temperature of less then 35.5 degrees can also indicate infection and can become life-threatening.
Let your nurse or doctor know if you have a temperature of 38 degrees or more, or if your temperature is less than 36 degrees.
However, not all cases of febrile neutropenia are due to infections. In some cases, you may have a fever more than 38 degrees, even if you don’t have an infection. If this happens while you are neutropenic, it will be treated as though you have an infection until infection is ruled out. Some medicines such as the chemotherapy cytarabine can cause a rise in your temperature, even without infection.
When to go to the emergency room
As mentioned above, febrile neutropenia is a medical emergency. Do not hesitate to call an ambulance or get someone to drive you to the emergency room at your nearest hospital if you have had treatment for your lymphoma and have any of the following symptoms:
- fever of 38 degrees or more – even if it has gone down since you last checked
- your temperature is less than 36 degrees
- your temperature has changed more than 1 degree from what it normally is – For example – If your temperature is normally 36.2 degrees and it is now 37.3 degrees. Or if it is normally 37.1 degrees and it is now 35.9 degrees
- rigors – (shaking) or chills
- dizziness or changes to your vision – this could indicate your blood pressure is dropping which can be a sign of infection
- changes in your heartbeat, or feeling your heart beating more than usual
- diarrhea, nausea or vomiting
- cough, shortness of breath or wheezing
- any signs of infections as listed above
- you generally feel very unwell
- have a sense something is wrong.
What to expect when you go to the hospital
When you call an ambulance or arrive at the emergency department, let them know:
- You have lymphoma (and the subtype)
- What treatments you have had and when
- You may be neutropenic
- You have a fever
- Any other symptoms you have.
You will likely have a blood test done to check your neutrophils levels, and a septic screen.
A septic screen is a term used for a group of tests to check for infections. These include the below:
- Blood tests called “blood cultures”. These will likely be taken from all lumens of your central line if you have one, as well as directly from your arm with a needle.
- Chest X-Ray.
- Urine sample.
- Stool (poo) sample if you have diarrhea.
- Swabs from any sores on your body or in your mouth.
- Swabs from around your central line if it looks infected.
- Respiratory swabs if you have symptoms of COVID, cold, flu or pneumonia.
If an infection is suspected, you will be started on antibiotics even before the results come in. You will be started on a broad-spectrum antibiotic which is effective at treating many different types of infections. You may have more than one type of antibiotic.
You will be admitted to hospital so the antibiotics can be given intravenously (into your blood stream through a cannula or central line) so they take effect quicker.
Once the results of your swabs, blood tests and other samples come in, your doctor may change your antibiotics. This is because once they know what germ is making you sick, they can pick a different antibiotic that is more effective at fighting that particular germ. However, it can take several days for these results to come in, so you will stay on the broad-spectrum antibiotics during this time.
Summary
- Neutropenia is a very common side-effect of treatments for lymphoma.
- You are more likely to be neutropenic 7-14 days after chemotherapy however, neutropenia can also be a late side-effect of some treatments, starting months to even years after treatment.
- You are more likely to get infections when you are neutropenic.
- Take all your prophylactic medications as you are instructed, and take precautions to avoid infections.
- If you are neutropenic, avoid foods more likely to carry germs.
- Infections while you are neutropenic can quickly become life-threatening.
- If you have had treatment for lymphoma, or know you are neutropenic, get immediate medical help if you have any signs of infections. Call an ambulance or go to your nearest emergency department
- You may not get normal symptoms of infection while neutropenic.
- If you have febrile neutropenia, you will be admitted to hospital for intravenous antibiotics.
- If you are not sure, of have any questions, do not hesitate to contact our Lymphoma Care Nurses Monday – Friday Eastern Standard Time.