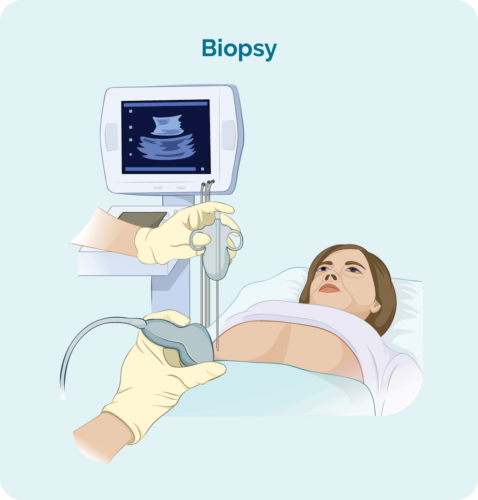
There are a number of tests and scans that you will need to have before you start cancer treatment. It is important for your medical team to do these tests to check how your vital body organs are currently working (function). These are known as ‘baseline’ organ function tests and scans. Your vital body organs include your heart, kidneys and lungs.
Most cancer treatments can cause various side effects. Some of these side effects have the potential of causing short- or long-term harm to some of your vital body organs. Particularly some chemotherapy can cause harm to different body organs. Tests and scans that will be needed depends on the type of cancer treatment that is being given.
Many of these scans will be repeated during and after treatment to ensure that the treatment is not harming these vital organs. If the treatment does affect the organs, the treatment might sometimes either be adjusted or sometimes changed. This is to try and make sure that vital organs are not impacted permanently.
Cardiac (heart) function tests
Some chemotherapy treatments are known to cause harm to the heart and how it functions. It is important that doctors know how your heart functions prior to treatment starting. If you already have a heart that is not functioning as well as it should, this may determine the type of chemotherapy that can be given.
If the heart function lowers to a certain level during treatment, the treatment dose might decrease or be stopped. Chemotherapy used in some lymphoma treatments that can cause harm such as doxorubicin (adriamycin), daunorubicin and epirubicin, are known as anthracyclines.
What are the types of cardiac function tests?
Electrocardiogram (ECG)
An electrocardiogram (ECG) is a test that helps to find problems with the heart muscle, valves, or rhythm. An ECG is a painless test that checks your heart’s function without being invasive. It records the electrical activity of the heart as lines on a piece of paper.
This test is done at a doctor’s office or at a hospital. Either nurses or medical technicians often perform the ECG. A doctor then reviews the test result.
Before having an ECG tell your health care team about all the medications you take. Ask whether you should take them on the day of the test because some medicines can affect the results.
- You usually do not need to restrict your food or drink intake before your ECG.
- You will need to remove your clothing from the waist up during your ECG.
- An ECG takes about 5 to 10 minutes to complete. During an ECG, a nurse or medical technician will place stickers called leads or electrodes on your chest and limbs (arms and legs). Then, they will connect wires to them. These leads collect details about your heart’s electrical activity. You will need to stay still during the test.
- After the test, you can go back to your normal activities, including driving.
Echocardiogram (echo)
An echocardiogram (echo) is a test that helps to find problems with the heart muscle, valves, or rhythm. An echo is an ultrasound of your heart. Ultrasounds use high-frequency sound waves to take a picture of organs inside the body. A wand-like device called a transducer sends out sound waves. Then, the sound waves “echo” back. The test is painless and not invasive.
- An echo is done at a doctor’s office or at a hospital. Sonographers, who are specially trained to use ultrasound machines, often perform an echo. A doctor then reviews the test results.
- Before having your echo, tell your health care team about all the medications you take. Ask whether you should take them on the day of the test because some medicines can affect the results.
- You usually do not need to restrict your food or drink intake before your echo.
- You will need to remove your clothing from the waist up during your echo.
- An echo takes about 30 minutes to 1 hour to complete. During an echo, you will lie on your side on a table and be asked to stay still. The ultrasound technician will apply a small amount of gel to your chest. Then they will move the wand-like transducer around your chest to create pictures of your heart.
- After the test, you can go back to your normal activities, including driving.
Multigated acquisition (MUGA) scan
Also known as ‘cardiac blood pooling’ imaging or ‘gated blood pool’ scan. A multigated acquisition (MUGA) scan creates video images of the lower chambers of the heart to check whether they are pumping blood properly. It shows any abnormalities in the size of the chambers of the heart and in the movement of blood through the heart.
Doctors also sometimes use MUGA scans as follow-up care to find potential long-term heart side effects, or late effects. Late effects may occur more than 5 years after treatment. Cancer survivors who may need follow-up MUGA scans include:
- People who have had radiation therapy to the chest.
- People who have had a bone marrow/stem cell transplant or certain types of chemotherapy.
A MUGA scan is performed in the radiology department of a hospital or at an outpatient imaging centre.
- You may not be able to eat or drink for 4 to 6 hours before the test.
- You may also be asked to avoid caffeine and tobacco for up to 24 hours before the test.
- Instructions will be given to you before your test. Bring a full list of all your medications you are on.
- When you arrive for your MUGA scan, you may need to remove your clothing from the waist up. This includes jewellery or metal objects that could interfere with the scan.
- The scan may take up to 3 hours to complete. The timing depends on how many pictures are needed.
- The technologist will place stickers called electrodes on your chest to monitor your heart’s electrical activity during the test.
- A small amount of a radioactive material will be injected into a vein in your arm. The radioactive material is called a tracer.
- The technologist will take a small amount of blood from your arm and mix it with the tracer.
- Then the technologist will put the mixture back into your body through an intravenous (IV) line inserted directly into a vein.
The tracer is like a dye. It binds to your red blood cells, which carry oxygen throughout your body. It shows how blood moves through your heart. You will not be able to feel the tracer move through your body.
The technologist will ask you to lie still on a table and place a special camera above your chest. The camera is about 3 feet wide and uses gamma rays to track the tracer. As the tracer moves through your bloodstream, the camera will take pictures to see how well the blood is pumping through your body. The pictures will be taken from many views, and each one lasts about 5 minutes.
You may be asked to exercise in between pictures. This helps the doctor see how your heart responds to the stress of exercise. The technologist may also ask you to take nitro-glycerine to open your blood vessels and see how your heart responds to the medication.
You can expect to return to your normal activities immediately after the test. Drink plenty of fluids and urinate frequently for 1 to 2 days after the scan to help the tracer leave your body.
Respiratory function tests
There are some chemotherapy treatments used in lymphoma treatment that can affect the function of your lungs and affect breathing. Bleomycin is a common chemotherapy used in the treatment of Hodgkin lymphoma. A baseline test is done to see how well your respiratory function is before treatment, again during treatment and often after treatment.
If your respiratory function decreases, this drug may be stopped. There are many clinical trials currently looking at stopping this drug after 2-3 cycles if patients have a complete remission. This is to reduce the risk of respiratory issues.
What is a respiratory (lung) function test?
Lung function tests are a group of tests that measure how well the lungs are working. They measure how much air your lungs can hold and how well you can let the air out of your lungs.
- Spirometry measures how much air you can breathe out from your lungs and how quickly you can do it.
- Lung plethysmography measures how much air is in your lungs after you take a deep breath and how much air is left in your lungs after you breathe out as much as you can.
- Lung diffusion testing measures how well oxygen moves from your lungs into your blood.
Lung function tests are usually done in a special department of a hospital by a trained respiratory therapist.
Tell your healthcare team about all prescription and non-prescription medicines you are taking. You are usually told not to smoke for 4 to 6 hours before you have a pulmonary function test.
Wear loose clothing so that you can breathe comfortably. Avoid eating a heavy meal before pulmonary function tests – it can make it harder for you to take deep breaths.
Spirometry test
Spirometry test is one of the standard lung function tests used to determine both the volume of air that the lungs can inhale and exhale, and the rate at which air can be inhaled and exhaled. The device used is called a spirometer, and most modern spirometers are connected to a computer which instantly computes the data from a test.
You will be asked to breathe using a long tube with a cardboard mouthpiece. The long tube is attached to a computer that measures the amount of air breathed out over time.
You will first be asked to breathe gently through the mouthpiece. You will then be asked to take in the biggest breath you can and then blow it out as hard, fast, and long as you can.
Lung plethysmography test
This test determines:
- Total lung capacity. This is the volume of air in the lungs after a maximal inspiration.
- Functional Residual Capacity (FRC). FRC is the volume of air in the lungs at the end of a quiet resting expiration
- Residual volume which is the volume of air left in the lung after a maximal expiration.
During the test you will be asked to sit in a sealed box that looks a little like a telephone box. There is a mouthpiece inside the box which you will need to breathe in and out of during the test.
The operator will tell you how to breathe in and out of the mouthpiece while measurements are taken. A shutter inside the mouthpiece will open and close to allow various readings to be taken. Depending on the tests required, you may need to breathe in other (inert and harmless) gases as well as air. The whole test generally takes no longer than 4-5 minutes.
Let the doctor know if you are taking any medications, particularly if they are related to breathing difficulties, as you may need to stop taking these before the test. If you catch a cold or other illness that may prevent you breathing properly, you may need to rearrange the test for when you are better.
Do not wear any clothing that might stop you from breathing in and out fully and avoid eating a large meal within two hours of the test, or drinking alcohol (within four hours) or smoking (within an hour) of the test. You should also not do any strenuous exercise in the 30 minutes before the test.
Lung diffusion testing
Measures how well oxygen moves from your lungs into your blood.
During lung diffusion testing, you breathe in a small amount of carbon monoxide gas through a mouthpiece on a tube. After holding your breath for about 10 seconds, you then blow out the gas.
This air is collected in the tube and examined.
You should not smoke or drink alcohol in the 4-hour period before the test. Wear loose fitting clothing so you can breathe properly during the test.
Let your doctor know what medications you are taking and whether to stop taking them before the test.
Renal (kidney) function tests
There are chemotherapy treatments that may affect your kidney function. It is important to check your kidney function before treatment starts, during treatment and sometimes after treatment. Your renal function can also be monitored through blood tests prior to each chemotherapy cycle. These following tests get a more accurate look at how well your kidneys function.
If your kidney function declines during treatment, your treatment dose might be reduced, delayed or stopped all together. This is to help prevent further damage to your kidneys. Common chemotherapies that are used in lymphoma and may cause damage include; ifosfamide, methotrexate, carboplatin, radiotherapy and prior to stem cell transplants.
What are some of the kidney function tests used?
Renal (kidney) scan
A kidney scan is an imaging test that looks at the kidneys.
It is a type of nuclear imaging test. This means that a tiny amount of a radioactive matter is used during the scan. The radioactive matter (radioactive tracer) is absorbed by normal kidney tissue. The radioactive tracer sends out gamma rays. These are picked up by the scanner to take pictures.
When booking a scan, a technologist will provide you with any relevant preparation instructions.
Some instructions may include:
- Patients are usually required to drink 2 glasses of water within 1 hour of the test.
- The radioactive tracer is injected into a vein in your arm. Following administration of the radiotracers, scanning will take place.
- The duration for a scan will vary in length depending on the clinical question being addressed. Scanning time usually takes an hour.
- You can resume normal activity after the scan.
- Increase fluid intake to help flush out the tracer.
Renal ultrasound
A renal ultrasound is a non-invasive exam that uses ultrasound waves to produce images of your kidneys.
These images can help your doctor evaluate the location, size, and shape of your kidneys as well as blood flow to your kidneys. A kidney ultrasound usually includes your bladder.
Ultrasound uses high-frequency sound waves sent out by a transducer pressed against your skin. The sound waves move through your body, bouncing off organs back to the transducer. These echoes are recorded and digitally turned into video or images of the tissues and organs selected for examination.
Instructions about how to prepare and what to expect will be given to you before your appointment.
Some important information includes;
- Drinking 3 glasses of water at least one hour before the exam and not emptying your bladder
- You will be lying face down on an exam table which may be a bit uncomfortable
- Have a cold conductive gel applied to your skin in the area being examined
- The transducer will be rubbed against the area being examined
- Procedure is painless
- You can return to normal activities after the procedure